14/06/2004
Breast pain, medically known as mastalgia, is an incredibly common experience, affecting as many as two-thirds of women at some point in their lives. It's a sensation that can range from a subtle tenderness to a sharp, burning ache, and while it often resolves on its own, it frequently prompts worry. Many find that this discomfort aligns with significant life stages, such as menstruation, pregnancy, or menopause, naturally leading to the question: is there a direct link between breast pain and hormonal fluctuations? This article aims to shed light on that connection, explore other potential causes, and provide practical advice for managing this prevalent concern.
- What is Breast Pain (Mastalgia)?
- The Dominant Factor: Cyclical Breast Pain and Hormones
- Beyond Hormones: Non-Cyclical Breast Pain
- Why Just One Side? Unilateral Breast Pain Explained
- Breasts Sore Around Your Period? Understanding Cyclical Patterns
- When to Consult a Healthcare Professional
- Effective Strategies for Managing Breast Pain
- The Emotional Impact of Breast Pain
- Proactive Steps for Breast Health: A Lifelong Commitment
- Frequently Asked Questions (FAQs)
- Conclusion – Navigating Breast Pain with Confidence
What is Breast Pain (Mastalgia)?
Breast pain can manifest in various ways, from a dull, heavy ache to a stabbing, shooting pain. While it's understandable to feel concerned when experiencing such discomfort, it's crucial to understand that breast pain is very rarely a sign of a serious underlying condition like cancer. In the vast majority of cases, it's benign and often temporary.
However, if your breast pain persists for several weeks, if it worsens over time, or if it's accompanied by other symptoms such as a new lump, nipple discharge, or changes to the skin of your breast, it is always wise to seek medical advice. A healthcare professional can provide reassurance and rule out any more serious issues, though most women find that simple lifestyle adjustments are often enough to alleviate their symptoms.
The Dominant Factor: Cyclical Breast Pain and Hormones
When categorising breast pain, two distinct types emerge: cyclical and non-cyclical. The former, cyclical breast pain, is by far the most common and is directly attributed to the ebb and flow of hormones within a woman's body. This type of pain typically follows a predictable pattern, often intensifying in the days leading up to a menstrual period and subsiding once menstruation begins.
The primary culprits behind cyclical breast pain are the fluctuating levels of oestrogen and progesterone. These two hormones play a crucial role in preparing the body for a potential pregnancy each month. As their levels rise, particularly in the luteal phase (the second half of the menstrual cycle), they directly affect the breast tissue. This hormonal stimulation can lead to several changes:
- Tissue Swelling and Tenderness: Oestrogen and progesterone can cause the milk glands and ducts within the breasts to enlarge and swell, making the breasts feel heavier, fuller, and more tender to the touch.
- Water Retention: Hormonal changes can also lead to increased fluid retention throughout the body, including within the breast tissue. This added fluid can contribute to a feeling of tightness, fullness, and discomfort.
- Fibrocystic Changes: Occasionally, these hormonal fluctuations can contribute to what is known as fibrocystic change. This is a benign condition where fluid-filled cysts and fibrous tissue develop in the breast, making them feel lumpy or rope-like. These cysts can sometimes cause localised tenderness or pain.
It's estimated that around three-quarters of all breast pain complaints are cyclical in nature, underscoring the significant role that hormonal changes play. If you're experiencing cyclical breast pain, your doctor might suggest charting your pain for a few weeks. This involves noting when the pain occurs, its intensity, and its relationship to your menstrual cycle. Such a record can be invaluable in helping your healthcare provider accurately diagnose the cause and recommend the most appropriate course of action.
Beyond Hormones: Non-Cyclical Breast Pain
While hormones are a leading cause, they don't account for every instance of breast pain. Non-cyclical breast pain, by definition, does not follow a pattern related to the menstrual cycle and is often less predictable. This type of pain typically arises from factors unrelated to hormonal shifts, often stemming from the breast tissue itself or the surrounding structures.
Common causes of non-cyclical breast pain include:
- Trauma or Injury: A direct blow to the breast, even a minor one, can cause bruising and localised pain. This could be from an accidental bump, a sports injury, or even a seatbelt during a sudden stop.
- Inflammation: Conditions like costochondritis, an inflammation of the cartilage that connects the ribs to the breastbone, can cause sharp, localised pain that can be mistaken for breast pain. Other inflammatory conditions affecting the breast tissue itself, though less common, can also occur.
- Muscle Strain: The pectoral muscles lie beneath the breast tissue. Strenuous exercise, especially activities that heavily involve the chest muscles, can lead to muscle strain or soreness that radiates into the breast area. This is particularly common if you're not wearing a properly supportive bra during physical activity, as the movement can put stress on the chest area, especially for women with larger breasts.
- Ill-fitting Bras or Foreign Objects: A bra that digs into the breast tissue, particularly if the underwire is improperly fitted or bent, can cause significant soreness and discomfort. Similarly, any foreign object pressing against the breast can lead to localised pain.
Distinguishing between cyclical and non-cyclical pain is key to effective management. While cyclical pain often responds to strategies that address hormonal balance, non-cyclical pain requires identifying and treating the specific underlying cause.
Why Just One Side? Unilateral Breast Pain Explained
Experiencing pain in just one breast can be particularly unsettling. While it's common for both breasts to feel tender during hormonal fluctuations, unilateral pain often prompts greater anxiety about more serious conditions. However, it's important to remember that many causes of one-sided breast pain are benign.
Here are some common reasons why you might experience discomfort specifically in one breast:
- Hormonal Fluctuations (Uneven Sensitivity): Even though hormones affect both breasts, it's possible for one breast to be more sensitive to these fluctuations than the other. This can lead to a more pronounced feeling of swelling, tenderness, or pain on one side. Natural variations in hormone receptor distribution can contribute to this asymmetry.
- Cysts: Breast cysts are fluid-filled sacs that can develop within the breast tissue. They are usually benign and are most common in women aged 35-50. If a cyst forms in one breast, it can cause localised pain, tenderness, or a palpable lump in that specific area. While generally harmless, larger cysts can sometimes be drained if they are causing significant discomfort.
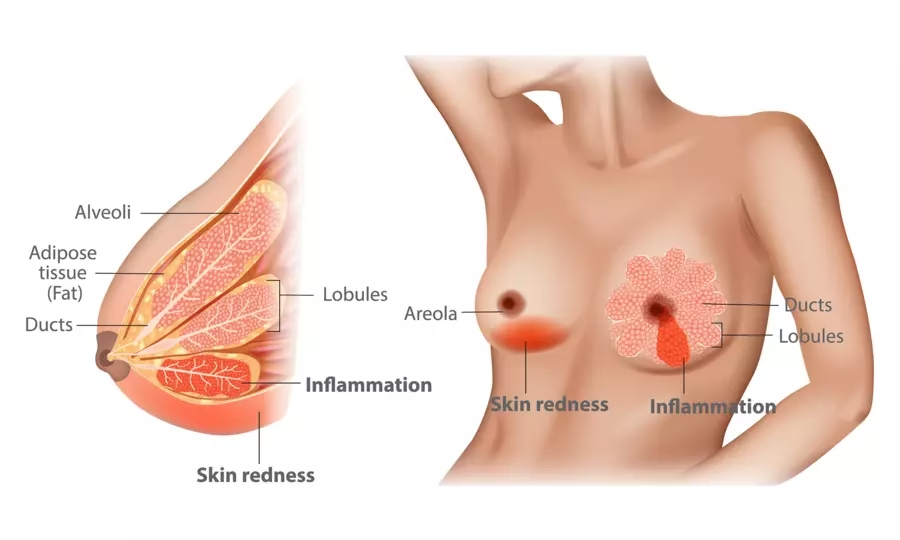
- Infections (Mastitis): Mastitis is an inflammation of the breast tissue, often accompanied by an infection. While commonly associated with breastfeeding, it can affect any woman. Symptoms typically include redness, warmth, swelling, and significant pain in the affected breast. It may also be accompanied by fever and flu-like symptoms. Mastitis usually requires antibiotic treatment.
- Fibrocystic Changes (Localised): While fibrocystic changes can affect both breasts, it's possible for the cysts or fibrous tissue to be more prominent or cause more discomfort in one breast than the other. This can lead to a feeling of lumpiness or tenderness localised to one side.
- Injury or Trauma: As mentioned earlier, a direct injury or trauma to one breast can cause localised pain, bruising, and swelling. This could be from a fall, a sports impact, or even a pet jumping on your chest.
- Other Localised Issues: Less commonly, a benign tumour (such as a fibroadenoma), a blocked milk duct (even outside of breastfeeding), or even a strained muscle in the chest wall on one side can manifest as pain seemingly originating from a single breast.
Understanding these potential causes can help alleviate anxiety, but persistent one-sided pain should always be evaluated by a healthcare professional to ensure an accurate diagnosis.
| Cause of Unilateral Pain | Description | Typical Characteristics |
|---|---|---|
| Hormonal Fluctuations | One breast may be more sensitive to normal oestrogen/progesterone changes. | Tenderness, fullness, often cyclical but pronounced on one side. |
| Breast Cysts | Fluid-filled sacs in breast tissue. | Localised pain, tenderness, often a palpable lump. |
| Infection (Mastitis) | Inflammation of breast tissue, often bacterial. | Redness, warmth, swelling, significant pain, fever. |
| Fibrocystic Changes | Benign lumps/fibrous tissue more noticeable on one side. | Lumpiness, tenderness, often cyclical. |
| Injury/Trauma | Physical impact or strain to the breast/chest wall. | Localised pain, bruising, soreness. |
Breasts Sore Around Your Period? Understanding Cyclical Patterns
Many women report their breasts feeling sore or tender 'around' their menstrual period, sometimes even specifically asking why they hurt 'after' their period. It's important to clarify the typical pattern of cyclical breast pain, which is indeed driven by hormones.

Generally, breast soreness associated with your menstrual cycle tends to begin three to five days *before* your period is due. This timing aligns perfectly with the peak in oestrogen and progesterone levels that occurs just before menstruation. These elevated hormones cause the breast tissue to swell and retain fluid, leading to the characteristic feeling of tenderness, heaviness, and sometimes sharp pain.
The good news is that for most women, this pain typically *subsides* or stops hurting once the menstrual period begins or shortly thereafter. As menstruation starts, the levels of oestrogen and progesterone drop significantly, allowing the breast tissue to return to its normal state, and the associated discomfort usually resolves. So, if you experience soreness *after* your period, it might be a lingering effect from the pre-menstrual phase, or it could indicate a non-cyclical cause that warrants investigation.
When to Consult a Healthcare Professional
While most breast pain is benign and often resolves on its own, there are instances when seeking medical advice is prudent. It's always better to be safe and have any concerns addressed by a doctor, especially if you notice any of the following:
- Persistent breast pain that doesn't improve after a few weeks.
- Pain that is localised to one specific area and doesn't fluctuate with your menstrual cycle.
- Pain that is accompanied by a new lump or thickening in the breast or armpit.
- Any changes to the skin of the breast, such as redness, dimpling, puckering, or an 'orange peel' texture.
- Nipple discharge, especially if it's bloody or clear.
- Nipple changes, such as inversion (turning inwards) or scaling.
When you consult a healthcare provider, they will typically begin with a thorough medical history, asking about your symptoms, their duration, their relationship to your menstrual cycle, and any other relevant health information. This will usually be followed by a physical examination.
Physical Examination
During a physical examination, the clinician will carefully examine both breasts, feeling for any lumps, areas of tenderness, swelling, or changes in texture. They will also inspect the skin of your breasts and nipples for any visible abnormalities. This hands-on assessment is a crucial first step in determining the nature of your breast pain.
Imaging Tests
Depending on their findings during the physical exam and your medical history, your doctor may recommend further imaging tests to get a clearer picture of your breast tissue. These might include:
- Mammogram: An X-ray of the breast, often used for screening for breast cancer, but also useful for investigating lumps or pain.
- Ultrasound: This uses sound waves to create images of the breast's internal structures. It's particularly good at distinguishing between fluid-filled cysts and solid masses. It's often used in conjunction with a mammogram, especially for younger women or those with dense breast tissue.
These diagnostic tools help your doctor to accurately identify the cause of your pain and rule out any serious conditions.
Effective Strategies for Managing Breast Pain
Regardless of whether your breast pain is cyclical or non-cyclical, there are several strategies you can employ to help alleviate the discomfort and improve your quality of life.
Lifestyle Adjustments
- Wear a Supportive Bra: This is perhaps one of the simplest yet most effective measures. A well-fitting, supportive bra can significantly reduce breast movement, which in turn minimises strain on the breast tissue and surrounding ligaments. This is particularly important during exercise, where a high-impact sports bra can make a considerable difference. Ensure your everyday bra offers good support and fits correctly, especially if you have larger breasts.
- Dietary Changes: While scientific evidence is mixed, some women report a reduction in cyclical breast pain by making certain dietary adjustments. Reducing caffeine intake (found in coffee, tea, chocolate, and some soft drinks) is a commonly suggested strategy. Similarly, some find relief by reducing their intake of high-fat foods and increasing their consumption of complex carbohydrates. Increasing your intake of flaxseed or evening primrose oil, which contain essential fatty acids, has also been anecdotally helpful for some, though always consult a doctor before taking supplements.
- Pain Relievers: Over-the-counter pain medications such as paracetamol (acetaminophen) or non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can help manage mild to moderate breast pain. Always follow the dosage instructions carefully.
Medical Interventions
- Antibiotics: If your breast pain is due to an infection like mastitis, your doctor will prescribe a course of antibiotics to clear the infection.
- Monitoring Cysts: If benign cysts are identified and are not causing severe pain or complications, your doctor may recommend a 'wait and see' approach, as many cysts resolve on their own over time. Larger or painful cysts can sometimes be drained.
- Hormone Therapy Adjustments: In some cases of severe cyclical breast pain, a doctor might discuss adjusting or prescribing hormonal medications, though this is less common and usually reserved for cases that don't respond to other measures.
The Emotional Impact of Breast Pain
It's important to acknowledge that experiencing persistent or unexplained breast pain can have a significant emotional impact. Many women naturally worry about serious conditions like breast cancer, and this anxiety can add another layer of distress to the physical discomfort. It’s essential to recognise these feelings and understand that while it’s natural to worry, most cases of breast pain are benign.
Openly discussing your concerns with supportive friends or family members can provide emotional relief. If anxiety or stress related to your breast pain becomes overwhelming, seeking professional counselling or support from a mental health professional can also be incredibly beneficial. Remember, addressing your emotional well-being is just as important as managing the physical symptoms.
Proactive Steps for Breast Health: A Lifelong Commitment
Maintaining overall breast health is a crucial aspect of women's well-being, regardless of age or whether you currently experience breast pain. Taking proactive steps can help you become familiar with your breasts, recognise changes, and potentially detect issues early.

| Preventive Measure | Description | Benefit |
|---|---|---|
| Regular Self-Exams | Perform monthly self-examinations to become familiar with the normal look and feel of your breasts. | Helps you recognise any new or unusual changes promptly. |
| Scheduled Mammograms | Follow recommended guidelines for regular mammogram screenings based on your age and risk factors. | Detects abnormalities, including early-stage cancers, often before they can be felt. |
| Healthy Lifestyle Choices | Maintain a balanced diet rich in fruits, vegetables, and whole grains, and engage in regular physical activity. | Supports overall health and may reduce the risk of certain breast conditions. |
| Avoid Smoking & Limit Alcohol | Eliminate tobacco products and consume alcohol in moderation. | Reduces the risk of various health issues, including some breast conditions. |
| Consult Healthcare Providers Regularly | Attend routine check-ups and discuss any breast-related concerns with your doctor without delay. | Ensures timely evaluation and professional advice for any symptoms or worries. |
Staying informed about your personal health history, including any family history of breast conditions, also plays a vital role in understanding your individual risks and guides your preventive health strategy.
Frequently Asked Questions (FAQs)
Q: Is breast pain always serious?
A: No, breast pain is rarely a sign of a serious condition like cancer. Most cases are benign and often related to hormonal changes or minor injuries.
Q: Can men experience breast pain?
A: Yes, though less common, men can also experience breast pain (gynecomastia), often due to hormonal imbalances, medication side effects, or certain medical conditions. They should also seek medical advice if concerned.
Q: Do certain foods worsen breast pain?
A: While scientific evidence is limited, some women report that reducing caffeine intake, high-fat foods, and increasing certain fatty acids (like those in flaxseed or evening primrose oil) can help alleviate cyclical breast pain.
Q: How long does cyclical breast pain usually last?
A: Cyclical breast pain typically begins a few days before your menstrual period and usually subsides once your period starts or shortly thereafter.
Q: When should I be worried about one-sided breast pain?
A: While many causes are benign, you should be concerned and seek medical advice if one-sided pain is persistent, severe, accompanied by a new lump, skin changes, or nipple discharge.
Understanding why you might experience breast pain, whether it's a general tenderness or discomfort localised to just one side, involves recognising a range of potential causes. From the widespread influence of hormonal fluctuations during different life stages to specific issues like cysts, infections, or physical trauma, many factors can contribute to this common complaint.
While it’s natural to feel worried when faced with breast pain, particularly when it's persistent or unilateral, the vast majority of cases are benign. Being proactive about your breast health through regular self-examinations, adhering to screening guidelines, and maintaining a healthy lifestyle are all crucial steps. Most importantly, never hesitate to consult a healthcare professional if you have any concerns or if your pain doesn't resolve. Empowering yourself with knowledge and seeking timely medical advice can significantly alleviate anxiety and contribute to your overall well-being.
If you want to read more articles similar to Understanding Breast Pain: Hormones & More, you can visit the Automotive category.
