11/07/2002
Crohn's disease, a chronic inflammatory condition affecting the digestive tract, can present a challenging journey for those living with it. Characterised by inflammation that can impact any part of the gastrointestinal system, from mouth to anus, it most commonly targets the junction between the small and large intestines. This persistent inflammation can lead to a myriad of symptoms, including severe abdominal pain, persistent diarrhoea, and sometimes, painful fissures or fistulas around the anus. While there's currently no cure, the primary goal of treatment is to effectively manage symptoms, reduce inflammation, correct nutritional deficiencies, and ultimately, improve the patient's quality of life. This article delves into the various treatment approaches, with a specific focus on the role of antibiotics, alongside other crucial medical and lifestyle interventions.
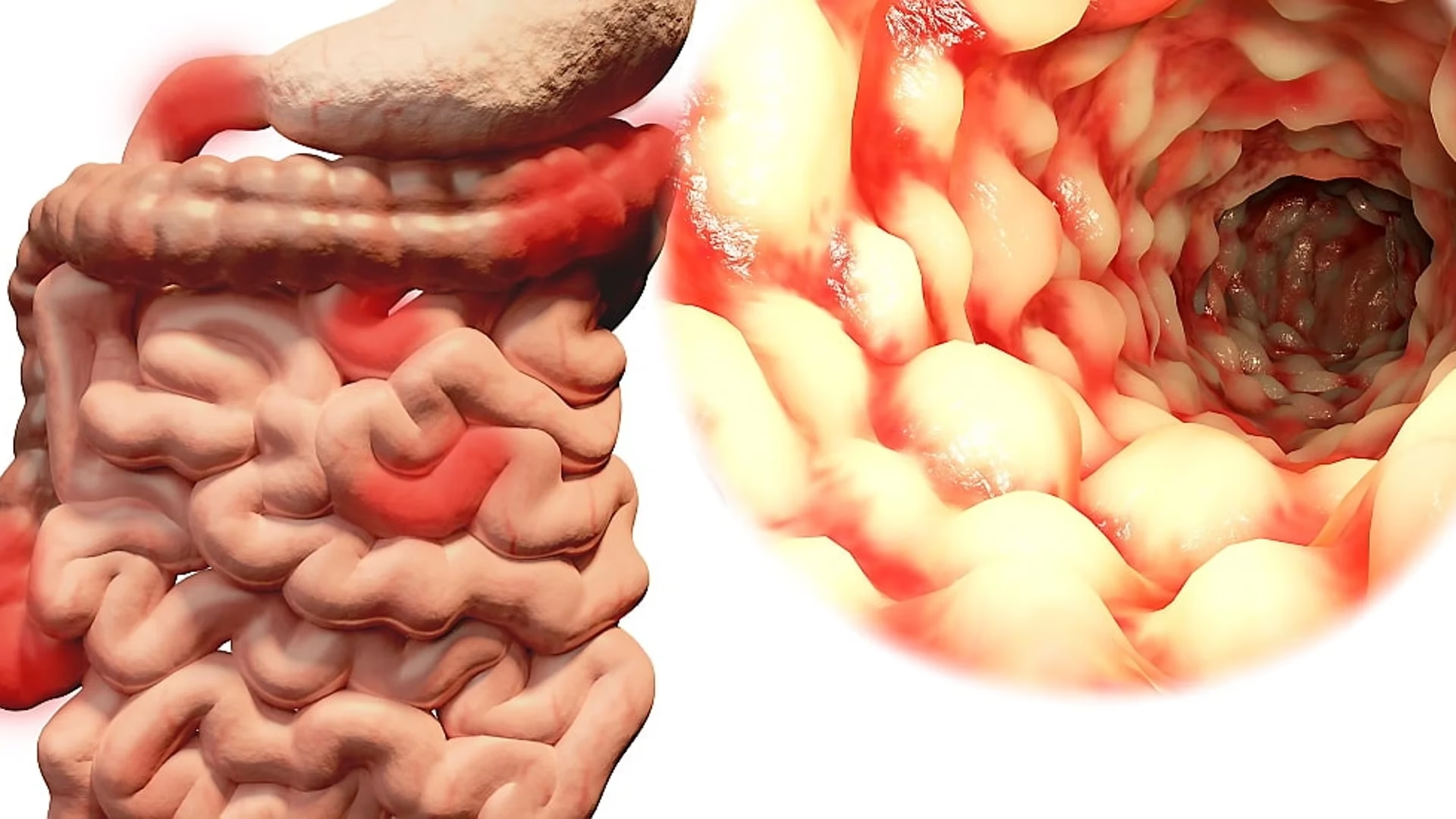
- Understanding Crohn's Disease and Its Impact
- The Broad Spectrum of Crohn's Treatment
- Nutritional Management: Supporting the Body
- Lifestyle Adjustments for Better Management
- Living with Crohn's: Empowering Self-Management
- Comparative Overview of Crohn's Disease Medications
- Frequently Asked Questions About Crohn's Disease Management
- Are antibiotics a cure for Crohn's disease?
- When are antibiotics typically prescribed for Crohn's?
- Can diet alone control Crohn's disease?
- Is smoking cessation really that important for Crohn's patients?
- What are the main goals of Crohn's disease treatment?
- What is Exclusive Enteral Nutrition (EEN)?
Understanding Crohn's Disease and Its Impact
Crohn's disease is one of the two main forms of Inflammatory Bowel Disease (IBD), sharing similarities with ulcerative colitis. Unlike ulcerative colitis, which is typically confined to the large intestine, Crohn's can affect patches of the digestive tract, leaving healthy areas in between. The inflammation can penetrate deep into the bowel wall, leading to complications such as strictures (narrowed sections of the bowel due to scarring and inflammation), which can cause severe pain and obstruction, and fistulas, abnormal connections between parts of the bowel, or between the bowel and other organs or the skin. The unpredictable nature of the disease, with periods of remission followed by debilitating flares, makes long-term management a complex but essential aspect of living with Crohn's.
The Broad Spectrum of Crohn's Treatment
The approach to treating Crohn's disease is highly individualised, depending on the affected areas of the bowel, the severity of the condition, the presence of complications, and the patient's response to previous treatments. A multidisciplinary approach often involves medication, nutritional support, and in some cases, surgery. The aim is not just to alleviate immediate symptoms but to achieve and maintain remission, allowing the body to heal and preventing further complications.
Pharmacological Interventions: A Multi-Pronged Approach
Medication forms the cornerstone of Crohn's management, with various classes of drugs targeting different aspects of the disease.
Corticosteroids: Rapid Relief for Acute Flares
Corticosteroids, such as prednisolone or budesonide, are potent anti-inflammatory drugs often used to quickly suppress inflammation during active disease flares. They can provide rapid relief from symptoms like pain and diarrhoea. However, their use is strictly limited to short-term periods, typically no more than 3-4 months, due to the risk of significant side effects. These can include increased susceptibility to infections, bone thinning, weight gain, and mood changes. They are not suitable for long-term maintenance therapy.
Biologic Therapies: Revolutionising Treatment
Biological medicines have transformed the landscape of Crohn's disease treatment, particularly for moderate to severe cases that haven't responded to conventional therapies. These drugs target specific proteins in the immune system that drive inflammation. The most commonly used biologics include TNF-alpha blockers like Infliximab and Adalimumab, which block Tumour Necrosis Factor-alpha, a key inflammatory protein. Newer biologics such as Vedolizumab and Ustekinumab, which target different inflammatory pathways, are also increasingly being used. While highly effective in inducing and maintaining remission, biologics can increase the risk of serious infections, and their long-term effects are still under ongoing study. They represent a significant advancement, offering hope for many patients who previously had limited options.
Immunosuppressants: Modulating the Immune Response
Immunosuppressants, like Azathioprine, Mercaptopurine, and Methotrexate, work by dampening the overall immune system activity to reduce inflammation. Azathioprine has historically been a cornerstone of Crohn's treatment, often used in combination with corticosteroids to allow for a reduction in steroid dosage, thereby mitigating their long-term side effects. Common side effects can include nausea, vomiting, diarrhoea, and a reduced ability to fight off infections. While still used, their role has somewhat diminished with the advent of biologics, which are often preferred due to their more targeted action and potentially better efficacy profile for some patients.
Antibiotics: A Targeted Approach for Specific Complications
Unlike other medications that directly target inflammation, antibiotics are not a primary treatment for the underlying inflammation of Crohn's disease. Instead, they are prescribed to manage specific complications that can arise due to the disease's effects on the bowel. The unique challenges of Crohn's, such as narrowed sections of the bowel (strictures), the formation of fistulas, or changes following previous surgery, can create environments where bacteria can thrive abnormally.
- Bacterial Overgrowth: Strictures or areas of stagnant bowel can lead to an overgrowth of bacteria in the small intestine, causing symptoms like bloating, gas, and worsening diarrhoea. Antibiotics are used to reduce this bacterial load and alleviate associated symptoms.
- Fistulas and Abscesses: Crohn's disease can lead to the formation of fistulas (abnormal tunnels) and abscesses (collections of pus), particularly around the anus (perianal disease). Antibiotics play a crucial role in treating these infections, often in conjunction with surgical drainage if an abscess is present.
- Post-Surgical Infections: Following surgery for Crohn's disease, antibiotics may be used to prevent or treat infections at the surgical site or within the abdominal cavity.
The most commonly used antibiotics for these specific Crohn's-related complications include Metronidazole, Ampicillin, Cephalosporin, Ciprofloxacin, and Tetracycline. The choice of antibiotic depends on the suspected type of infection, its location, and the patient's individual circumstances. It's important to reiterate that antibiotics are used to treat bacterial complications, not the inflammatory process of Crohn's itself, and their use is typically for specific, often short-term, periods.
Symptomatic Relief
Beyond addressing inflammation and infection, some medications are used to manage specific symptoms. Anti-diarrhoeal agents like Loperamide can help reduce the frequency and urgency of bowel movements. For patients who have undergone a resection of the small intestine, which can lead to bile acid malabsorption and diarrhoea, bile acid binders such as Cholestyramine may provide relief.
Nutritional Management: Supporting the Body
Proper nutrition is vital for individuals with Crohn's disease, especially given the potential for malabsorption and nutritional deficiencies. While no specific diet has been definitively proven to prevent or treat Crohn's (with one notable exception), dietary adjustments can significantly help manage symptoms and support overall health.
Dietary Considerations
Patients are generally advised to maintain a nutritious diet and identify any foods that appear to worsen their symptoms. Common triggers can include dairy products, alcohol, spicy foods, fried foods, and high-fibre foods, particularly if strictures are present. In cases of strictures, foods that are difficult to digest, such as mushrooms, citrus fruits, or asparagus, should be avoided to prevent obstruction. A dietitian can provide personalised advice and support.
Nutritional Supplements
Due to potential malabsorption, many Crohn's patients benefit from nutritional supplements. Folic acid supplementation is often recommended, as the disease and certain medications can impair its absorption. In children, where growth may be stunted due to the disease, calorie-rich nutritional drinks or even intravenous nutrition may be used to ensure adequate caloric intake.
Exclusive Enteral Nutrition (EEN)
Exclusive enteral nutrition (EEN) is a highly effective dietary therapy, particularly in children and adolescents, where it has shown similar efficacy to corticosteroids in inducing remission. This treatment involves consuming only liquid nutritional formulas, often via a feeding tube, for a period, typically around six weeks. EEN not only helps alleviate acute symptoms but has also been shown to promote healing of the intestinal lining, a significant advantage over corticosteroids which primarily suppress symptoms. While challenging due to the restriction from solid foods, EEN can be a powerful tool, particularly for disease affecting the small and large bowel.
Lifestyle Adjustments for Better Management
Beyond medical and nutritional therapies, certain lifestyle modifications can play a crucial role in managing Crohn's disease and improving overall well-being.
The Vital Role of Smoking Cessation
Perhaps one of the most impactful lifestyle changes a person with Crohn's can make is to stop smoking. Smoking cessation is critical because smoking is strongly associated with a more severe disease course, increased frequency of flares, and a higher risk of needing surgery. Quitting smoking can significantly improve disease outcomes and reduce the likelihood of complications.
Stress Management and Sleep
While stress doesn't cause Crohn's, it can certainly exacerbate symptoms. Learning and implementing stress reduction techniques, such as mindfulness, meditation, or yoga, can be beneficial. Similarly, ensuring adequate and restorative sleep is important for overall health and can help the body cope with the demands of a chronic illness.

Physical Activity
Regular physical activity is generally beneficial for health. When the disease is in remission and there is no active inflammation, individuals with Crohn's can typically engage in physical activity as they wish. However, during active flares, intense or prolonged exercise, or activities that increase abdominal pressure (like heavy lifting), might need to be modified or avoided.
Oral Health
Crohn's disease can impact nutrient absorption, leading to a need for frequent snacking, which in turn can increase the risk of dental cavities. Regular dental check-ups and meticulous oral hygiene are therefore particularly important. Patients with Crohn's may also be eligible for special dental care subsidies.
Hydration
During periods of severe diarrhoea, there's a significant risk of dehydration and electrolyte imbalance. It is crucial to drink plenty of fluids and ensure adequate intake of salt and sugar to replenish what is lost. A good indicator of sufficient hydration is maintaining normal urine output despite diarrhoea.
Living with Crohn's: Empowering Self-Management
Living with a chronic condition like Crohn's disease requires ongoing self-management and a proactive approach to one's health.
Patient Education and Engagement
Understanding your condition and its treatment is empowering. Patients are encouraged to learn about their disease, their medications, and why they are prescribed. Keeping a symptom diary can help identify triggers and patterns in the disease's behaviour, aiding both the patient and their healthcare team in making informed decisions.
Maintaining Communication with Healthcare Teams
Establishing a strong, open relationship with your healthcare team, including your gastroenterologist and specialist nurse, is paramount. Regular follow-up appointments, often involving blood and stool tests, help monitor disease activity and treatment effectiveness. Knowing who to contact during a flare-up or with new symptoms provides reassurance and facilitates timely intervention.
Utilising Support Networks
Connecting with others who have Crohn's disease through patient organisations can be incredibly beneficial. Sharing experiences, tips, and emotional support can alleviate feelings of isolation and provide practical advice for navigating daily challenges. Organisations like the National Association for Colitis and Crohn's Disease (NACC) in the UK offer valuable resources and community support.
Travel Tips
When travelling abroad, it's important to carry documentation for your medications, such as a prescription or a doctor's letter, to demonstrate their medical necessity. This can prevent issues with customs and ensures access to your vital treatments.
Comparative Overview of Crohn's Disease Medications
To summarise the diverse pharmacological approaches, here's a brief comparison of the main drug classes:
| Medication Class | Primary Use | Duration of Use | Key Considerations |
|---|---|---|---|
| Corticosteroids | Rapidly reduce acute inflammation during flares. | Short-term (max 3-4 months). | Significant side effects, not for long-term maintenance. |
| Biologic Therapies | Induce and maintain remission in moderate to severe disease. | Long-term. | Highly effective, but increased infection risk, higher cost. |
| Immunosuppressants | Suppress immune system to reduce inflammation; maintain remission. | Long-term. | Side effects (nausea, infection risk), often combined with steroids, less common than biologics now. |
| Antibiotics | Treat specific bacterial complications (overgrowth, fistulas, abscesses, post-surgery). | Short-term, targeted. | Not for underlying inflammation; specific bacterial issues only. |
Frequently Asked Questions About Crohn's Disease Management
Are antibiotics a cure for Crohn's disease?
No, antibiotics are not a cure for Crohn's disease. They are used to treat specific bacterial complications that can arise from the disease, such as bacterial overgrowth in the bowel, fistulas, or abscesses. They do not treat the underlying chronic inflammation that defines Crohn's.
When are antibiotics typically prescribed for Crohn's?
Antibiotics are prescribed when there's evidence of bacterial infection or overgrowth. This includes situations like small intestinal bacterial overgrowth (SIBO) due to strictures, infected fistulas or abscesses, and sometimes as a preventive measure after certain surgeries to reduce infection risk.
Can diet alone control Crohn's disease?
While diet plays an important role in managing symptoms and ensuring adequate nutrition, it cannot typically control the underlying inflammation of Crohn's disease on its own, with the exception of Exclusive Enteral Nutrition (EEN) in specific cases, particularly in children. Most patients require medication to achieve and maintain remission.
Is smoking cessation really that important for Crohn's patients?
Absolutely. Smoking is one of the most significant risk factors for a more severe disease course in Crohn's, increasing the frequency of flare-ups, the need for surgery, and reducing the effectiveness of some treatments. Quitting smoking is one of the most impactful positive changes a Crohn's patient can make for their health.
What are the main goals of Crohn's disease treatment?
The primary goals of Crohn's treatment are to suppress inflammation, relieve debilitating symptoms (like pain and diarrhoea), correct any nutritional deficiencies, prevent complications such as strictures and fistulas, and ultimately, improve the patient's overall quality of life and achieve long-term remission.
What is Exclusive Enteral Nutrition (EEN)?
EEN is a dietary therapy where a patient consumes only specially formulated liquid nutritional drinks for a period (e.g., 6 weeks), avoiding all solid food. It's particularly effective in children for inducing remission and healing the gut lining, often used as an alternative to corticosteroids for acute flares.
Managing Crohn's disease is a lifelong journey that requires a comprehensive and adaptive approach. By combining targeted medical therapies, including the judicious use of antibiotics for specific complications, with tailored nutritional strategies and crucial lifestyle adjustments, individuals with Crohn's can significantly improve their symptoms, achieve periods of remission, and lead fulfilling lives. Ongoing communication with healthcare providers and engagement with patient support networks are key to navigating this complex condition effectively.
If you want to read more articles similar to Navigating Crohn's: Antibiotics & Beyond, you can visit the Automotive category.
