28/01/2002
Embarking on the journey of In Vitro Fertilisation (IVF) is a significant step for many couples hoping to conceive. While much focus is often placed on the female partner's reproductive health, the male factor, specifically sperm quality and quantity, plays an equally crucial role in the success of these advanced reproductive technologies. Understanding the nuances of sperm parameters, such as Total Motile Count (TMC) and Total Progressive Motility Count (TPMC), can empower couples to make informed decisions and optimise their path to parenthood.
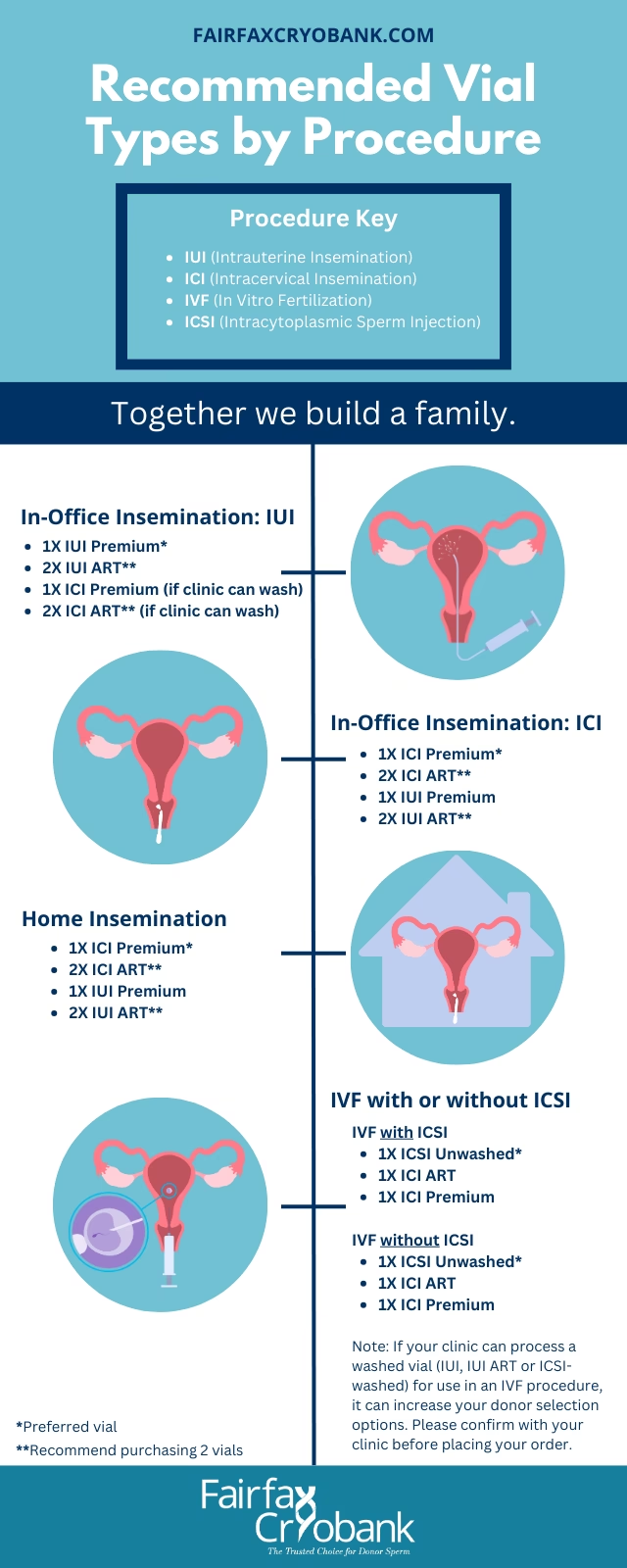
- Sperm Requirements for IVF and ICSI
- Understanding Total Motile Count (TMC) and Total Progressive Motility Count (TPMC)
- The Clinical Impact of Sperm Quality on Fertility Outcomes
- Frequently Asked Questions About Sperm Count and IVF
- Q1: How many sperm cells are truly needed for IVF?
- Q2: Does the total motile sperm count (TMC) affect IVF success?
- Q3: What's the difference between MOT20, MOT10, and MOT2 straws?
- Q4: Can I calculate my TMC or TPMC from my semen analysis report?
- Q5: Is it better to focus on TMC or TPMC?
- Q6: Does sperm quality matter if we're doing ICSI?
- Conclusion
Sperm Requirements for IVF and ICSI
When undergoing IVF, the aim is for your eggs to be fertilised in a laboratory setting within a Petri dish. For this process, a surprisingly modest number of high-quality sperm are often sufficient. Specifically, for standard IVF, straws labelled MOT10+, containing at least 5 million motile sperm cells, are generally considered adequate to achieve successful fertilisation. These figures are based on the concentration of actively swimming sperm.
It's important to clarify what 'MOT' signifies. MOT stands for Motile Total and indicates the amount of forward-moving sperm cells per millilitre (mio/ml) at the time of cryopreservation. All reputable sperm donors adhere to World Health Organisation (WHO) guidelines for normal sperm quality. Therefore, a MOT10 or MOT2 straw does not imply lower sperm quality; rather, the concentration of sperm has been specifically diluted to fit these categories, making them suitable for different treatment types:
- MOT20: At least 20 million motile sperm per ml. This is typically the highest concentration available and is often recommended for Intrauterine Insemination (IUI).
- MOT10: At least 10 million motile sperm per ml. This concentration is versatile and suitable for both IUI and IVF procedures.
- MOT2: At least 2 million motile sperm per ml. This lower concentration is specifically designed for Intracytoplasmic Sperm Injection (ICSI), where a single sperm is injected directly into each egg.
If you are uncertain about the specific type of fertility treatment you will undergo, opting for MOT20+ straws is often a safe bet, as this concentration is generally suitable for all forms of treatment, providing maximum flexibility.
Understanding Total Motile Count (TMC) and Total Progressive Motility Count (TPMC)
Beyond simply having a certain number of sperm, the overall quality and movement of sperm are paramount. This is where concepts like Total Motile Count (TMC) and Total Progressive Motility Count (TPMC) become critical. These metrics provide a more comprehensive assessment of male fertility potential compared to just looking at sperm density or motility in isolation.
What is Total Motile Count (TMC)?
The TMC addresses the variability in ejaculate volumes by combining sperm density, overall motility, and ejaculate volume to provide the total number of swimming sperm present in the entire ejaculate. Different laboratories may use slightly different terms like “total motile sperm” or “motile sperm count,” but the key identifier is the unit of measure, which should be in millions (e.g., “__ million” or “__ × 106”), as opposed to “__ million per cc” for sperm density.
If your semen analysis report doesn't explicitly state TMC, you can easily calculate it using the following formula:
(Sperm Density × Ejaculate Volume × Total Motility) ÷ 100
For example, if an analysis shows an ejaculate volume of 2.0 cc, a sperm density of 30 × 106/cc, and a total motility of 50 percent, the TMC would be (2.0 × 30 × 50) ÷ 100 = 30 million sperm.
It's crucial to differentiate TMC from "total count," which includes both motile and non-motile sperm and is a less useful indicator of fertility potential.
What is Total Progressive Motility Count (TPMC)?
The male fertility community often introduces another layer of specificity with TPMC. This metric focuses solely on the total number of sperm that are moving forward progressively – those actively swimming in a straight line or large circles. This makes intuitive sense, as these are the sperm most likely to reach and fertilise an egg. The calculation is similar to TMC, but uses progressive motility instead of total motility:
(Sperm Density × Ejaculate Volume × Progressive Motility) ÷ 100
Progressive motility is sometimes listed directly on the report, or it may need to be calculated by adding the percentages of Grade 2/Grade B (slow progressive) and Grade 3/Grade A (rapid progressive) motility.
Normal Ranges for TMC and TPMC
Defining "normal" ranges for TMC and TPMC is complex and can vary depending on the context of conception (natural, IUI, or IVF/ICSI). For natural intercourse or IUI, higher numbers of swimming sperm are generally better. A TMC of 25 million sperm or above is often considered indicative of good fertility potential, with some studies suggesting up to 75 million sperm may offer additional benefit for natural conception. For TPMC, a range of 20 million sperm or above is often cited as "normal," although pregnancies can occur with much lower counts.
A critical consideration for TMC is the average motility grade. A TMC is only considered "normal" if the average motility grade is 2 or higher, or if progressive motility is 30% or greater. This ensures that the counted sperm are not just moving, but moving effectively.

The Clinical Impact of Sperm Quality on Fertility Outcomes
While sperm density and overall motility are foundational, relying solely on isolated WHO criteria can be misleading. TMC and TPMC offer a more accurate prognostic assessment of a couple's chances of success across various conception methods.
Natural Intercourse
It's logical that more and better-swimming sperm improve the chances of natural conception. Studies have shown a strong correlation between increased TMCs and TPMCs and higher chances of natural pregnancy. For instance, a TPMC of <5 million sperm significantly lowers the chance of natural pregnancy compared to 5 million or above. Remarkably, even men with extremely low TPMC (<1 million) have been able to achieve natural pregnancies, albeit at a lower rate (around 25% over a three-year period). A TMC of 25 million sperm or above has been linked to a six-fold higher chance of natural conception compared to counts below this level.
Conclusion for Natural Intercourse: While natural conception is possible even with very low sperm counts, higher TMCs/TPMCs correlate with increased success. If natural conception hasn't occurred after a year and TPMC/TMC is <20-25 million, considering IUI or IVF might be advisable.
Intrauterine Insemination (IUI)
IUI success rates also intuitively increase with a higher presence of motile sperm. Research has explored various cut-off points for TMC and TPMC to determine when IUI becomes less effective and IVF should be considered. It's important to distinguish between pre-wash and post-wash sperm counts in IUI, as semen is processed to concentrate and select higher-quality sperm before insemination.
Pre-Wash Total Motile Count (TMC) for IUI
Some studies suggest a pre-wash TMC cut-off of 5 million sperm or above for IUI. For example, a study of 353 couples found a clinical pregnancy rate of 28.5% when TMC was less than 5 million, compared to 44.3% when it was 5 million or above. Other studies point to a higher recommended TMC of 10 million sperm for better success rates. One study even reported no successful pregnancies with IUI when TMC was less than 5 million, rising to 9.5% for 5-10 million and 17.4% for above 10 million.
Pre-Wash Total Progressive Motility Count (TPMC) for IUI
Early studies suggested a pre-wash TPMC of 1 million or above could increase IUI success. More recent research indicates that higher TPMC correlates with better outcomes. For instance, a 2011 study showed pregnancy rates increasing from 5.1% (TPMC < 5 million) to 15.1% (TPMC between 5 and 10 million).
Post-Wash Total Motile Counts (PWTMC) for IUI
While pre-wash numbers are useful for initial counselling, post-wash counts, obtained after semen processing, can provide additional predictive information for subsequent IUI cycles. A meta-analysis of 55 studies suggested a PWTMC of 1 million sperm as a cut-off for increased IUI success. However, other studies indicate that pregnancy rates are significantly higher with PWTMC of 5 million or above. A large 2021 study of 90,000 IUI cycles demonstrated improved outcomes with higher post-wash TMCs, though pregnancies were still established at lower counts:
| Post-Wash TMC (millions) | Clinical Pregnancy Rate (%) |
|---|---|
| 1.0 - 1.99 | 7.45 |
| 2.0 - 3.99 | 10.13 |
| 4.0 - 4.99 | 11.63 |
| 5.0 - 5.99 | 12.87 |
| 6.0 - 6.99 | 13.93 |
| 7.0 - 8.99 | 14.33 |
| 9+ | 16.70 |
Conclusion for IUI: Both pre-wash and post-wash motile sperm counts correlate with IUI outcomes. While pre-wash numbers guide initial decisions, post-wash evaluations can inform future cycles. Controversy exists regarding definitive cut-offs, but generally, pre-wash TMCs of 5-10 million (ideally ≥20 million) and post-wash TPMC of 1-5 million (ideally >5 million) are associated with better success.
IVF/ICSI Success
For IVF and especially ICSI, the number of sperm required is far fewer than for natural conception or IUI. In ICSI, theoretically, only one viable sperm is needed per egg retrieved (typically 5-15 eggs). In the early days of ICSI, it was often believed that sperm quality became irrelevant due to the direct injection process, compensating for any defects as long as enough viable sperm were present. However, contemporary research has strongly contradicted this notion.
Many studies now demonstrate that lower sperm quality can indeed negatively impact IVF/ICSI outcomes. Elevated levels of sperm DNA Fragmentation Index (DFI), for instance, have been shown to adversely affect IVF/ICSI success rates. Moreover, a man's total motile sperm count has been found to correlate with IVF/ICSI success.

A 2016 study, examining 518 couples undergoing ICSI, compared outcomes for men with a TPMC of <1 million sperm versus those with >20 million sperm. The group with higher TPMC (>20 million) exhibited a significantly higher fertilisation rate (84.9% vs. 72.5%) and a lower miscarriage rate (17.9% vs. 33.3%). Higher TPMC also predicted a greater chance of producing high-quality embryos and a higher number of embryos reaching the blastocyst stage.
This evidence underscores that optimising sperm quality is beneficial even before engaging in advanced reproductive treatments like IVF/ICSI. While these technologies can overcome certain male factor infertility issues, better sperm quality consistently leads to more favourable outcomes, highlighting the importance of a thorough male fertility evaluation.
Frequently Asked Questions About Sperm Count and IVF
Q1: How many sperm cells are truly needed for IVF?
For standard IVF, where sperm and eggs are combined in a dish, MOT10+ straws (containing at least 5 million motile sperm cells) are typically sufficient. For ICSI, where a single sperm is injected into each egg, significantly fewer are needed, often as low as MOT2+ straws (at least 2 million motile sperm per ml) suffice, as only one viable sperm per egg is technically required.
Q2: Does the total motile sperm count (TMC) affect IVF success?
Yes, contrary to earlier beliefs, a man's TMC and TPMC do affect IVF/ICSI success. Studies indicate that higher motile sperm counts are associated with better fertilisation rates, lower miscarriage rates, and a higher likelihood of developing high-quality embryos to the blastocyst stage. While IVF/ICSI can overcome severe male factor issues, optimising sperm quality remains beneficial for overall success.
Q3: What's the difference between MOT20, MOT10, and MOT2 straws?
These designations refer to the concentration of motile sperm cells per millilitre (mio/ml) at the time of cryopreservation. MOT20 has at least 20 million motile sperm/ml, MOT10 has at least 10 million motile sperm/ml, and MOT2 has at least 2 million motile sperm/ml. They all contain high-quality sperm but are diluted to different concentrations to suit various treatments: MOT20 for IUI (highest concentration), MOT10 for IUI and IVF, and MOT2 for ICSI.
Q4: Can I calculate my TMC or TPMC from my semen analysis report?
Yes, if your report doesn't explicitly state TMC or TPMC, you can calculate it. For TMC, use the formula: (Sperm Density × Ejaculate Volume × Total Motility) ÷ 100. For TPMC, use: (Sperm Density × Ejaculate Volume × Progressive Motility) ÷ 100. Ensure you use the correct units and percentages.
Q5: Is it better to focus on TMC or TPMC?
Both TMC and TPMC provide valuable information. TPMC specifically measures sperm capable of progressive forward movement, which is highly relevant for reaching and fertilising an egg. TMC, when considering the average motility grade, also offers important insights. Often, clinicians use whichever calculation is feasible based on the data provided in the semen analysis report. It's crucial to understand which metric is being discussed, as their "normal" cut-offs differ.
Q6: Does sperm quality matter if we're doing ICSI?
Yes, while ICSI bypasses some natural barriers by injecting a single sperm directly into an egg, the overall quality of that sperm still matters. Studies show that factors like sperm DNA fragmentation and overall motile count can still influence fertilisation rates, embryo quality, and miscarriage rates even with ICSI. Optimising sperm health before ICSI is therefore recommended.
Conclusion
The journey to conception, especially through advanced methods like IVF and ICSI, is multifaceted, with male factor fertility playing a crucial and often underestimated role. Understanding concepts like Total Motile Count (TMC) and Total Progressive Motility Count (TPMC) goes beyond simple sperm numbers, offering a more nuanced and predictive insight into a man's fertility potential. While IVF and ICSI can overcome many challenges, the growing body of evidence suggests that better sperm quality, as indicated by these comprehensive metrics, consistently leads to more favourable outcomes, including higher fertilisation rates, better embryo development, and reduced miscarriage risks. Therefore, a thorough evaluation of male fertility and, where possible, efforts to optimise sperm health, should be an integral part of any couple's fertility treatment plan, empowering them with the best possible chances of success.
If you want to read more articles similar to Sperm Count & IVF: Decoding Fertility Success, you can visit the Automotive category.
