22/06/2002
Chimeric Antigen Receptor (CAR)-T cell therapy has emerged as a groundbreaking advancement in cancer treatment, offering hope to patients with previously intractable malignancies. By harnessing the body's own immune system, CAR-T cells are engineered to recognise and destroy cancer cells with remarkable precision. However, this powerful therapy is not without its unique challenges, most notably the risk of severe side effects such as Cytokine Release Syndrome (CRS). Amidst this revolutionary landscape, a crucial drug, Tocilizumab, has established itself as an indispensable tool, effectively mitigating these toxicities and allowing patients to fully benefit from their life-saving treatment.
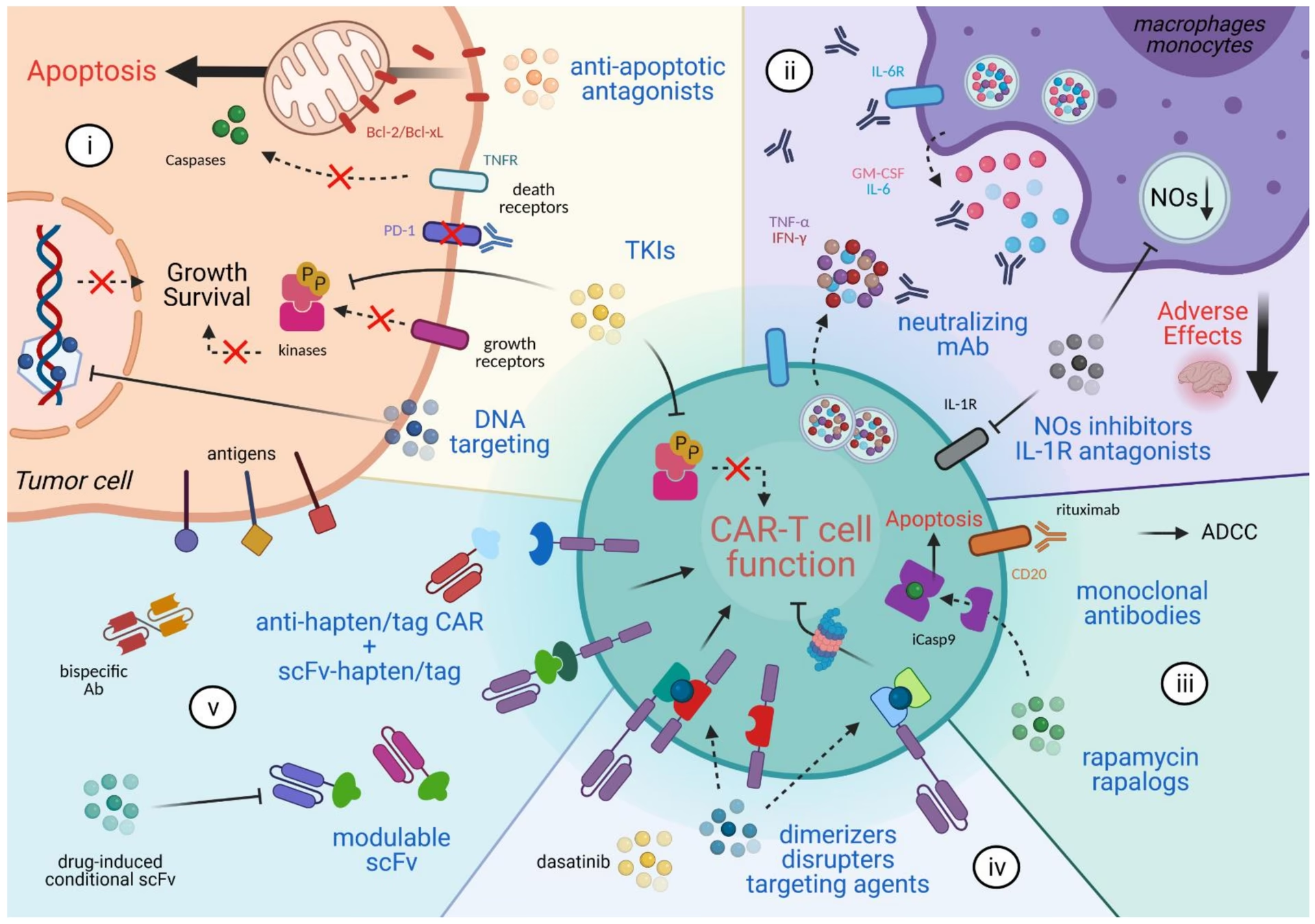
- What is CAR-T Cell Therapy?
- Understanding Cytokine Release Syndrome (CRS)
- Tocilizumab: The Mechanism of Action
- Clinical Efficacy in CAR-T Associated CRS
- Tocilizumab as a Prophylactic Treatment for CAR-T Cells
- Advantages and Limitations of Using Tocilizumab
- Safety and Adverse Events
- Management of Severe CRS with Tocilizumab
- Tocilizumab for Acute Obstructive Sclerosis (AOSD)
- Tocilizumab Biosimilars and Local Care Pathways
- Frequently Asked Questions (FAQs)
- Conclusion
What is CAR-T Cell Therapy?
CAR-T cell therapy represents a paradigm shift in oncology, moving beyond traditional chemotherapy to a highly personalised form of immunotherapy. It involves extracting a patient's own T-cells, a type of white blood cell crucial for immune response, and genetically modifying them in a laboratory. These modifications equip the T-cells with Chimeric Antigen Receptors (CARs), synthetic molecules designed to recognise specific proteins found on the surface of cancer cells. Once infused back into the patient, these engineered CAR-T cells proliferate and actively seek out and destroy tumour cells. The NHS has significant experience in developing and introducing such novel and potent anti-cancer treatments, recognising the critical need to concentrate and develop expertise in this complex field.
Understanding Cytokine Release Syndrome (CRS)
While CAR-T cell therapy is incredibly effective, its potent immune activation can lead to a severe systemic inflammatory response known as Cytokine Release Syndrome (CRS). CRS occurs as a result of non-antigen specific immune activation, where the activated CAR-T cells release a cascade of inflammatory cytokines into the bloodstream. Clinically and biologically, CRS often mimics conditions like Macrophage Activation Syndrome (MAS) or Hemophagocytic Lymphohistiocytosis (HLH). Key cytokines involved in driving this host immune dysregulation include interleukin-6 (IL-6), interferon-gamma (IFN-γ), and IL-10. Patients experiencing CRS can develop a range of symptoms, from fever and fatigue to more severe manifestations like profound hypotension requiring vasopressors, respiratory distress necessitating mechanical ventilation, and even multi-organ dysfunction. The severity of CRS can vary significantly, from mild to life-threatening, making its timely and effective management paramount to patient safety and treatment success.
Tocilizumab: The Mechanism of Action
Tocilizumab is a humanised monoclonal antibody of the IgG1κ class that specifically targets the human interleukin-6 receptor (IL-6R). IL-6 is a pleiotropic soluble mediator with profound effects on inflammation, immune response, and haematopoiesis. It plays a critical role in promoting T-cell differentiation, activating B-cells, and driving acute inflammatory responses. IL-6R exists in two forms: membrane-bound and soluble. When IL-6 binds to either form, it initiates a signalling cascade through a co-receptor called gp130, leading to the activation of the Jak/Stat pathway and subsequent cellular responses. Tocilizumab works by blocking IL-6-mediated signal transduction, effectively inhibiting IL-6 from binding to its receptor. This blockade disrupts both classical IL-6 signalling (where IL-6 binds to membrane-bound IL-6R) and trans-IL-6 signalling (where IL-6 binds to soluble IL-6R). By interrupting these pathways, Tocilizumab dampens the excessive inflammatory response characteristic of CRS. Originally approved for various rheumatologic diseases such as rheumatoid arthritis, Tocilizumab's efficacy in rapidly resolving severe CRS symptoms led to its FDA approval for CAR-T-associated CRS in 2017, following impressive clinical outcomes.
Clinical Efficacy in CAR-T Associated CRS
The clinical evidence supporting Tocilizumab's efficacy in managing CAR-T associated CRS is robust and spans various CAR constructs.
Tisagenlecleucel Trials
In the Phase 1/2a CTL019 study, where children and young adults with relapsed/refractory B-cell acute lymphoblastic leukaemia (B-ALL) received tisagenlecleucel, CRS occurred in all 30 patients. Eight of these patients developed severe CRS, requiring intensive care and vasopressor support. All patients with severe CRS received Tocilizumab, which resulted in rapid defervescence (reduction of fever) and stabilisation of blood pressure, with significant improvement typically observed within 1 to 3 days. Some patients required second doses or short courses of glucocorticoids. Crucially, all patients requiring Tocilizumab and/or steroids recovered from severe CRS and achieved disease remission. Similar positive outcomes were observed in the ELIANA trial, a Phase 2 global study, where 77% of patients experienced CRS. Twenty-eight patients received Tocilizumab for severe CRS, and all cases were reversible. Importantly, the use of Tocilizumab in both trials did not appear to compromise the clinical efficacy of CAR-T cells; patients achieved complete remission, demonstrated robust CAR-T cell proliferation, and maintained their persistence.

Axicabtagene Ciloleucel Trial
In the Phase 2 ZUMA-1 trial involving adults with refractory aggressive non-Hodgkin lymphoma receiving axicabtagene ciloleucel, CRS developed in 93% of patients, with 13% experiencing severe CRS. Tocilizumab was administered to 43% of all patients, regardless of CRS severity, and 27% received glucocorticoids. All CRS events were reversible, and immunosuppression for CRS did not negatively affect the overall response among patients in this study. Retrospective analysis showed a median time from CRS onset to the first Tocilizumab dose of 3 days, with many patients responding after a single dose.
Other CAR Constructs and T-Cell-Engaging Therapies
Tocilizumab's effectiveness extends beyond tisagenlecleucel and axicabtagene to other CAR constructs and T-cell-engaging therapies. In the Phase 1 CTL119 study, three patients with severe CRS experienced complete reversal of symptoms after receiving Tocilizumab. Similarly, in a Phase 1 trial using CD22-CAR-T cells, Tocilizumab, sometimes combined with corticosteroids, effectively reversed CRS symptoms in affected patients. Even with therapies like blinatumomab (a CD19/CD3 BiTE antibody) and flotetuzumab (a CD123/CD3 bispecific antibody), where CRS incidence might differ, Tocilizumab has been successfully used to resolve symptoms without impacting the anti-leukaemic activity of these agents.
Tocilizumab as a Prophylactic Treatment for CAR-T Cells
While Tocilizumab has proven highly effective in treating established CRS, the optimal timing of its administration remains a subject of ongoing research. One particularly promising area is the exploration of Tocilizumab as a prophylactic treatment strategy for CAR-T cell associated CRS. The hypothesis is that preemptive immunomodulation could significantly decrease the rates of severe CRS, particularly in patients with high disease burden, without negatively affecting the engraftment and persistence of CAR-T cells. There is an ongoing clinical trial (NCT02906371) specifically evaluating the efficacy of early Tocilizumab intervention in paediatric patients deemed at high risk for severe CRS due to their disease burden. This trial aims to determine if administering Tocilizumab before the onset of severe symptoms can prevent or minimise the most dangerous manifestations of CRS, thereby improving patient safety and outcomes. If successful, this prophylactic approach could revolutionise the management of CAR-T therapy toxicities, allowing for a smoother and safer treatment journey for patients.
Advantages and Limitations of Using Tocilizumab
Tocilizumab offers distinct advantages in the management of CAR-T-associated toxicities, but also has specific limitations.
Advantages
A significant advantage of Tocilizumab over other immunosuppressive agents, such as corticosteroids, is its apparent ability to control CRS symptoms without suppressing T-cell function or inducing T-cell apoptosis. This is critical because the primary goal of CAR-T cell therapy is to leverage the patient's own T-cells to fight cancer. Studies consistently show that patients who receive Tocilizumab for CRS treatment maintain robust CAR-T cell proliferation, expansion, and long-term persistence, ensuring the anti-cancer efficacy of the therapy is not compromised. Durable responses have been observed in patients treated with Tocilizumab, reinforcing its role as a safe and effective intervention.

Limitations
Despite its broad utility, Tocilizumab has not been shown to be effective for either the prevention or treatment of Immune Effector Cell-Associated Neurotoxicity Syndrome (ICANS), another significant CAR-T cell therapy associated toxicity. ICANS can manifest with symptoms ranging from headache and delirium to seizures and cerebral oedema. The ineffectiveness of Tocilizumab against ICANS is likely due to its inefficient distribution into the central nervous system (CNS), or the involvement of other cytokines beyond IL-6 in the pathophysiology of neurotoxicity. Therefore, Tocilizumab is not an approved treatment for neurotoxicity associated with CAR-T cell therapy. For ICANS, alternative therapies such as anakinra, an IL-1R antagonist, have shown promise in preclinical studies by potentially preventing neurotoxicity.
Safety and Adverse Events
In general, Tocilizumab is considered a very well-tolerated drug with a favourable safety profile. Despite its potent immunosuppressive effects, the risk of serious infections attributed to Tocilizumab monotherapy is comparable to other biologic disease-modifying antirheumatic drugs (DMARDs). However, it is important to note that a 'black box warning' in Tocilizumab's label describes an increased risk of serious infections. Common adverse events (AEs) include headache, diarrhoea, and neutropenia (a reduction in a type of white blood cell). In the context of CAR-T cell therapy, no serious adverse events have been directly attributed to Tocilizumab administration. While some patient deaths occurred in trials within 30 days of Tocilizumab, none were thought to be caused by the drug itself, further underscoring its safety when used appropriately.
Management of Severe CRS with Tocilizumab
Given the potentially life-threatening nature of CAR-T therapy-associated CRS, significant research has focused on identifying risk factors for severe CRS and determining the optimal timing for Tocilizumab administration. Key risk factors include a high disease burden before CAR-T infusion, which can lead to higher levels of T-cell activation, and higher infusion doses of CAR-T cell products. Early elevation of inflammatory markers like IL-6 and IFN-γ can also predict CRS severity and may guide pre-emptive anti-cytokine treatment. While specific guidelines vary slightly between different CAR-T products, there is a general consensus that Tocilizumab should be administered at the time of moderate-to-severe signs of CRS to minimise life-threatening complications without compromising CAR-T cell efficacy.
Tisagenlecleucel Guidelines: For patients receiving tisagenlecleucel, Tocilizumab is considered when CRS symptoms require moderate-to-aggressive intervention, such as haemodynamic instability despite fluid and vasopressor support, worsening respiratory distress, or rapid clinical deterioration. Doses can be repeated every 8 hours, up to a maximum of four doses. If no clinical improvement is seen after the first dose, concurrent administration of methylprednisolone should be considered.
Axicabtagene Ciloleucel Guidelines: For axicabtagene ciloleucel, the threshold for Tocilizumab administration is somewhat lower. Patients with moderate CRS symptoms, such as oxygen requirements less than 40% FiO2 or hypotension responsive to fluids or low-dose vasopressors, may receive Tocilizumab. Doses can also be repeated every 8 hours for a maximum of four total doses, with corticosteroids considered if no clinical improvement within 24 hours.

It is vital to recognise that these algorithms serve as guidelines, and the decision for optimal timing heavily relies on the clinical judgement of the treating institution and a multidisciplinary approach involving critical care teams. In rare circumstances, CRS may be refractory to Tocilizumab and additional immunosuppression is needed. Mechanisms for this failure are unclear but may involve inadequate Tocilizumab dosing, alternative cytokines driving the hypercytokinaemia, or compensatory feedback in IL-6 signalling. Investigations into alternative therapies for Tocilizumab and corticosteroid-refractory CRS are ongoing, including siltuximab (an IL-6 antagonist), dasatinib (a multityrosine kinase inhibitor), ruxolitinib (a Janus kinase inhibitor), anakinra (an IL-1 receptor antagonist), and Cytosorb cartridge columns. While anecdotal success has been reported, prospective clinical trials are needed to confirm their efficacy.
Tocilizumab for Acute Obstructive Sclerosis (AOSD)
Beyond its crucial role in CAR-T cell therapy, Tocilizumab has also been suggested as a treatment option for patients suffering from Adult-Onset Still's Disease (AOSD) who experience chronic arthritis unresponsive to conventional disease-modifying antirheumatic drugs (DMARDs) like methotrexate. AOSD is a rare inflammatory condition characterised by high fevers, rash, joint pain, and elevated inflammatory markers. As a monoclonal antibody, Tocilizumab's ability to block IL-6 signalling helps to dampen the systemic inflammation characteristic of AOSD, offering a targeted approach for those whose condition remains refractory to other treatments.
Tocilizumab Biosimilars and Local Care Pathways
The introduction of biosimilar medicines, such as Tyenne, a licensed Tocilizumab biosimilar, offers significant opportunities for the NHS to deliver better value in treating various conditions. For pharmacy teams and healthcare professionals planning to incorporate Tocilizumab biosimilars into local care pathways, thorough preparation is essential. This involves ensuring familiarity with national guidelines, commissioning policies, and the Summary of Medicinal Product Characteristics (SmPC) for the biosimilar. Understanding the background to biological and biosimilar medicines, as well as the specific licence and supporting evidence for Tocilizumab biosimilar, is crucial.
Developing an implementation plan requires collaborative work across integrated care systems, involving pharmacy, prescribing clinicians, specialist nurses, business managers, finance, contracting teams, and homecare providers. Key steps include:
- Patient Identification: Clinicians need to identify patients currently receiving Tocilizumab and then determine who is suitable for switching to the biosimilar, as well as those for whom it would be clinically inappropriate.
- Staff Familiarity: Ensuring all staff involved are comfortable with the evidence supporting biosimilars and addressing any clinician concerns.
- Service Capacity: Assessing and potentially increasing capacity to manage the additional workload associated with the introduction, considering impacts on clinic visits, infusions, injections, and pharmacy operations.
- Processes: Establishing clear processes for involving homecare leads early (as much subcutaneous Tocilizumab is delivered via homecare), ensuring shared decision-making with patients supported by written materials and education, and creating workable procedures for reviewing, switching, and discontinuing treatments in line with national recommendations.
- Savings Utilisation: Ensuring that the cost savings generated by biosimilar adoption are effectively used to offset costs, incentivise change, and ultimately improve patient care.
Frequently Asked Questions (FAQs)
Is Tocilizumab a chemotherapy drug?
No, Tocilizumab is not a chemotherapy drug. It is a monoclonal antibody that targets a specific part of the immune system (the IL-6 receptor) to reduce inflammation. Chemotherapy drugs work by directly killing rapidly dividing cancer cells.
Can Tocilizumab be used for conditions other than CAR-T cell CRS?
Yes, Tocilizumab was originally approved for various rheumatologic diseases like rheumatoid arthritis, systemic and polyarticular juvenile idiopathic arthritis, and giant cell arteritis. It has also been explored for use in Adult-Onset Still's Disease (AOSD) and, more recently, in severe COVID-19 associated cytokine storm.

Does Tocilizumab weaken the CAR-T cells?
Current clinical evidence suggests that Tocilizumab does not impair the function, expansion, or persistence of CAR-T cells. This is a significant advantage, as it allows for effective management of CRS without compromising the anti-cancer efficacy of the therapy.
Why is Tocilizumab not effective for neurotoxicity (ICANS)?
Tocilizumab is generally not effective for ICANS because it does not efficiently cross the blood-brain barrier to reach the central nervous system. Additionally, ICANS pathophysiology may involve other cytokines or mechanisms that Tocilizumab does not target.
What happens if CRS does not respond to Tocilizumab?
In cases where CRS is refractory to Tocilizumab, alternative immunosuppressive therapies may be considered. These include corticosteroids, other anti-cytokine agents like siltuximab (another IL-6 antagonist) or anakinra (an IL-1 receptor antagonist), or other investigational drugs like dasatinib or ruxolitinib. A multidisciplinary team approach is crucial in such complex situations.
Conclusion
CAR-T cell therapy has truly revolutionised the cancer treatment landscape, offering unprecedented opportunities for patients with difficult-to-treat malignancies. However, the success of this innovative therapy is intrinsically linked to the effective management of its associated toxicities, particularly Cytokine Release Syndrome. Tocilizumab stands as a cornerstone in this critical aspect of care, demonstrating impressive efficacy in dampening the severe inflammatory response of CRS without compromising the vital anti-cancer function of CAR-T cells. Its minimal toxicity profile further solidifies its indispensable role. While ongoing research continues to refine the optimal timing of intervention, especially concerning its potential prophylactic use in high-risk patients, and explores alternative agents for refractory cases, Tocilizumab remains a beacon of hope, ensuring that the transformative power of CAR-T cell therapy can be delivered safely and effectively to those who need it most. Furthermore, the integration of Tocilizumab biosimilars into local care pathways promises to enhance accessibility and cost-effectiveness, broadening the reach of this life-saving treatment.
If you want to read more articles similar to Tocilizumab: Revolutionising CAR-T Cell Therapy Care, you can visit the Automotive category.
