10/09/2020
For many men, the gradual onset of symptoms like persistent fatigue, a diminished sex drive, erectile dysfunction, and changes in mood or body composition can be deeply unsettling. These often vague yet impactful issues, frequently appearing in the late 40s or early 50s, can significantly interfere with daily life and overall happiness. While often attributed to lifestyle factors or the natural ageing process, these symptoms can sometimes be indicative of a more specific medical condition: testosterone deficiency. Understanding this condition and the pathways to effective treatment in the UK is crucial for those seeking to reclaim their vitality and well-being.
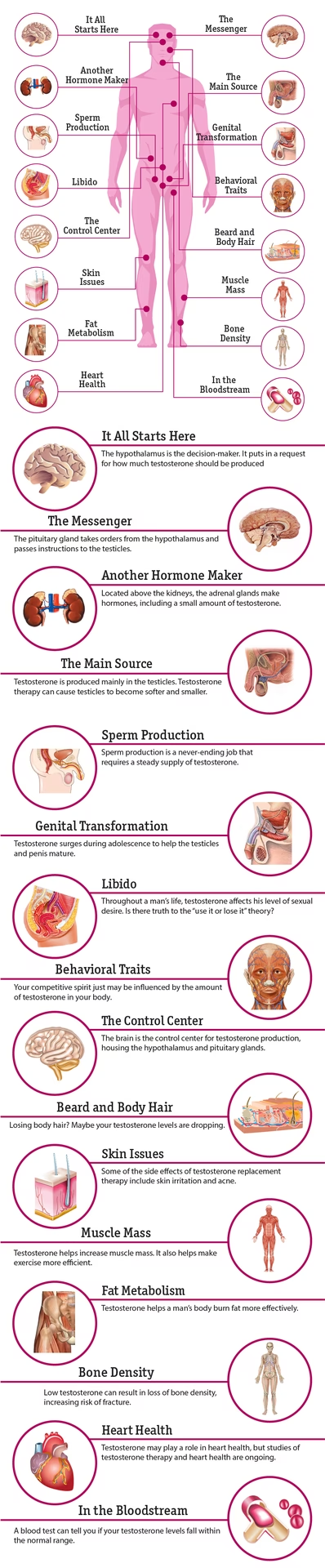
Testosterone, a vital hormone primarily produced in the testes, plays a pivotal role in numerous bodily functions, from maintaining bone density and muscle mass to regulating mood and sexual function. When levels dip below optimal, the impact can be profound, leading to a cascade of physical and psychological symptoms. Recognised as a legitimate medical condition, Testosterone Deficiency (TD) requires careful diagnosis and, in many cases, appropriate intervention through Testosterone Replacement Therapy (TRT).
- Understanding Testosterone Deficiency and Its Symptoms
- Why Consider Testosterone Replacement?
- Navigating TRT in the UK: NHS vs. Private Clinics
- The Dangers of Unregulated TRT
- Choosing the Best TRT Clinic in the UK
- Side Effects of Testosterone Replacement Therapy
- Frequently Asked Questions (FAQs)
- Conclusion
Understanding Testosterone Deficiency and Its Symptoms
The term 'male menopause' or 'andropause' is often used to describe the symptoms men experience in middle age, but it's largely a misleading label. Unlike the female menopause, which involves a sudden and significant drop in hormone levels, men's testosterone levels decline steadily by about 1% a year from around age 30 to 40. This gradual reduction typically doesn't cause significant problems on its own. However, a more pronounced deficiency, known as late-onset hypogonadism, can indeed be responsible for a range of disruptive symptoms. This specific medical condition is not a normal part of ageing but can particularly affect men who are obese or have type 2 diabetes.
Common symptoms associated with low testosterone include:
- Mood swings and increased irritability
- Persistent tiredness and lack of energy
- Brain fog and poor concentration
- Reduced libido and erectile dysfunction
- Loss of muscle mass and reduced exercise capacity
- Redistribution of fat, leading to increased belly fat or gynecomastia (enlarged male breasts)
- Difficulty sleeping or increased tiredness
- Low self-esteem or general lack of enthusiasm
It's important to note that many of these symptoms can also stem from lifestyle factors or psychological issues such as stress, depression, anxiety, a poor diet, lack of sleep, excessive alcohol consumption, or smoking. A thorough diagnostic process is essential to differentiate between these causes and confirm a testosterone deficiency.
Why Consider Testosterone Replacement?
When symptoms are persistent and significantly impact quality of life, and blood tests confirm low testosterone levels, TRT becomes a viable consideration. Before a general practitioner (GP) even considers investigations for testosterone replacement, they may need to manage other underlying health issues. These could include obstructive sleep apnoea, poorly controlled heart failure, severe lower urinary tract infections, pre-existing prostate issues, or polycythaemia (a high red blood cell count). Addressing these conditions first ensures that TRT, if prescribed, is administered safely and effectively, without exacerbating other health concerns.

TRT aims to restore testosterone levels to a healthy range, thereby alleviating symptoms and improving overall well-being. For many men, this can mean a significant improvement in energy levels, mood stability, cognitive function, libido, and physical performance.
Accessing Testosterone Replacement Therapy in the UK can be a complex journey, with distinct pathways through the National Health Service (NHS) and private clinics. Both routes have their advantages and disadvantages, and understanding these can help individuals make an informed decision.
TRT Through the NHS
While the NHS does provide TRT, the process is often characterised by stringent criteria, lengthy waiting times, and limited treatment options:
- Initial Consultation: The journey typically begins with a GP visit. If the GP recognises the symptoms of low testosterone, they may order an initial blood test to assess levels.
- Stringent Criteria: For a GP to consider prescribing testosterone, BSSM (British Society for Sexual Medicine) guidelines suggest levels should be 12 nmol/L or lower, alongside negative symptoms. However, many GPs are not confident in prescribing TRT and often defer to specialists. The NHS often uses a lower threshold for diagnosis than many private clinics, meaning many symptomatic individuals with levels above this cut-off are denied treatment.
- Referral to an Endocrinologist: If a patient qualifies based on these strict criteria, they are typically referred to an Endocrinologist, a hormone specialist. This referral process can take several months, leaving symptoms untreated and potentially worsening. Endocrinologists may also utilise local pathology reference ranges, which can vary and may not always reflect optimal health.
- Limited Treatment Options: Even when treatment is prescribed, the options available on the NHS may not always be tailored to individual patient needs, potentially leading to fluctuations in hormone levels and suboptimal results.
- Inconsistent Monitoring: NHS monitoring protocols may not always align with best practices for TRT optimisation, increasing the risk of side effects and inadequate symptom relief.
For many men, these barriers, particularly the long waiting times and restrictive criteria, lead them to seek alternative routes for TRT.
Private TRT in the UK
Private TRT clinics offer a more patient-centred and often faster approach to treatment:
- Specialist Expertise: Private clinics often focus exclusively on hormone therapy, ensuring patients receive care from experienced professionals who specialise in this field.
- Comprehensive Assessment: A thorough evaluation is standard, including an in-depth medical history, detailed symptom review, and extensive blood tests. This holistic approach ensures a more tailored and effective treatment plan.
- Personalised Treatment Plans: One of the key advantages of private care is the ability to adapt TRT to the individual. Personalised Treatment Plans consider lifestyle preferences, symptom severity, and how the patient responds to treatment, allowing for greater optimisation.
- Continuous Monitoring and Support: Regular follow-ups and adjustments are a cornerstone of private TRT, ensuring optimal effectiveness while minimising potential side effects. Patients often receive more consistent and proactive support.
- Faster Access: Shorter waiting times mean patients can receive diagnosis and begin treatment promptly, avoiding the long NHS delays.
The choice between NHS and private pathways often comes down to individual priorities regarding speed, personalisation, and the level of specialist care desired.

Comparison of NHS and Private TRT Pathways
To further illustrate the differences, consider the following comparison:
| Feature | NHS Pathway | Private Pathway |
|---|---|---|
| Initial Access | GP consultation, often requiring multiple visits. | Direct consultation with hormone specialist. |
| Diagnostic Criteria | Often stricter, lower testosterone thresholds. | More comprehensive, considering symptoms alongside levels. |
| Waiting Times | Can be months for specialist referral and treatment initiation. | Generally much shorter, often weeks or days. |
| Treatment Options | May be limited to standard formulations. | Wider range of tailored options (injections, gels, creams). |
| Monitoring & Follow-up | Can be inconsistent; less frequent. | Regular, comprehensive monitoring and adjustments. |
| Personalisation | Less individualised, often protocol-driven. | Highly personalised, considering lifestyle and response. |
| Specialist Expertise | Referral to a general endocrinologist. | Specialised clinics focused purely on hormone therapy. |
The Dangers of Unregulated TRT
While the allure of quick fixes or cheaper alternatives might lead some to consider self-prescribed TRT or unregulated online sources, this practice is highly discouraged and carries significant risks. Obtaining testosterone without a valid prescription is illegal in the UK. More importantly, it poses serious health dangers, including cardiovascular complications, severe hormone imbalances, and liver toxicity. Proper medical supervision is absolutely essential to ensure safe and effective treatment, with regular blood tests and clinical oversight to monitor progress and mitigate risks.
Choosing the Best TRT Clinic in the UK
Selecting a reputable TRT provider is paramount for a safe and effective treatment journey. A high-quality clinic should demonstrate several key characteristics:
- Experienced and Qualified Medical Professionals: Ensure the clinic employs doctors and specialists with extensive experience in hormone therapy and men's health.
- Care Quality Commission (CQC) Registration: Look for CQC registration, which indicates that the clinic meets national standards of quality and safety in health and social care.
- A Thorough Diagnostic Process: The clinic should conduct comprehensive evaluations, including in-depth medical history reviews, symptom assessments, and detailed blood tests, to ensure an accurate diagnosis.
- A Treatment Option That Best Meets Individual Needs: The clinic should offer a range of treatment options and work with you to find the most suitable method for your lifestyle and response.
- Continued Access to Medication to Ensure Safe Practice: Ensure the clinic provides clear pathways for prescription refills and ongoing medication management.
- Regular Monitoring and Follow-up Care: Optimal TRT requires consistent monitoring of hormone levels and overall health. The clinic should have robust protocols for regular check-ups and adjustments.
- Transparent Communication and Patient Education: A good clinic will ensure you are fully informed about your condition, treatment options, potential side effects, and what to expect throughout your therapy.
A clinic’s leadership can also be a key indicator of quality, often reflecting a passion for optimising men’s health and adherence to best practices in hormone therapy, ensuring patient safety, efficacy, and long-term well-being.
Side Effects of Testosterone Replacement Therapy
For most patients, Testosterone Replacement Therapy is well-tolerated with few side effects. However, like any medical treatment, there are potential risks that need to be monitored by a healthcare professional. The most significant side effect requiring careful monitoring is polycythaemia (an abnormally high red blood cell count). If left untreated, polycythaemia can increase the risk of serious complications, including strokes. For this reason, all patients on Testosterone Replacement Therapy require regular blood count measurements to ensure their levels remain stable and within a healthy range. Other potential, though less common, side effects can include fluid retention, acne, sleep apnoea exacerbation, and prostate enlargement, underscoring the importance of ongoing medical supervision.
Frequently Asked Questions (FAQs)
What are the main symptoms of low testosterone?
Common symptoms include chronic fatigue, low mood, irritability, reduced sex drive, erectile dysfunction, difficulty concentrating, loss of muscle mass, increased body fat, and disrupted sleep patterns.

Is 'male menopause' a real condition?
The term 'male menopause' is misleading. While testosterone levels do decline with age, this is usually gradual. A significant drop in testosterone causing symptoms is a specific medical condition called late-onset hypogonadism, which is not a normal part of ageing.
How is low testosterone diagnosed?
Diagnosis involves a review of your symptoms combined with specific blood tests to measure your testosterone levels. Typically, multiple blood tests might be required to confirm consistently low levels.
Can I get TRT on the NHS?
Yes, TRT is available through the NHS, but access can be challenging due to stringent diagnostic criteria, long waiting lists for specialist referrals (usually to an endocrinologist), and potentially limited treatment options.
What are the benefits of private TRT?
Private clinics generally offer faster access to specialists, more comprehensive assessments, highly personalised treatment plans, continuous monitoring, and a wider range of treatment options tailored to individual needs.

Are there any risks to TRT?
Most patients tolerate TRT well. However, potential risks include polycythaemia (high red blood cell count, which increases stroke risk), fluid retention, acne, and potential exacerbation of pre-existing prostate issues. Regular monitoring by a doctor is crucial to manage these risks.
Why might a GP delay TRT consideration?
GPs may need to first address other underlying health conditions such as obstructive sleep apnoea, uncontrolled heart failure, severe urinary tract issues, prostate problems, or polycythaemia, as these can affect the safety and effectiveness of TRT.
Conclusion
For men seeking to address the pervasive symptoms of low testosterone, navigating the available treatment options in the UK can feel daunting. While NHS treatment is an option, the restrictive eligibility criteria, differing diagnostic thresholds, and extended waiting times often make private care a more viable and efficient solution for many. Private TRT clinics offer specialist expertise, comprehensive assessments, personalised treatment plans, and ongoing support, ensuring patients receive the highest standard of care tailored to their unique needs.
Regardless of the pathway chosen, prioritising experienced and qualified medical professionals, regulatory compliance (such as CQC registration for private clinics), and patient-focused care is essential for ensuring the safest and most effective treatment journey. Ultimately, managing hormonal health effectively involves not just medical intervention but also a holistic approach that embraces the four crucial pillars of well-being: lifestyle, nutrition, exercise, and mindset. By taking an informed and proactive approach, men can successfully address testosterone deficiency and significantly improve their quality of life.
If you want to read more articles similar to Navigating Testosterone Replacement Therapy in the UK, you can visit the Automotive category.
