20/10/2022
Understanding the intricate journey of sperm is fundamental to comprehending male fertility. For conception to occur, sperm must undertake a remarkable trek through the female reproductive tract, a feat that demands efficient and purposeful movement. This crucial ability is known as sperm motility, and it stands as one of the most significant factors influencing a couple's chances of achieving pregnancy. Without adequate motility, even a high sperm count may not be enough, as the sperm simply cannot reach their intended destination: the female partner’s egg, poised for fertilisation.
- Understanding Sperm Motility: The Foundation of Fertilisation
- Why Sperm Motility Matters for Conception
- Defining 'Normal': What Healthy Sperm Motility Looks Like
- Asthenozoospermia: When Sperm Motility is Low
- Unravelling the Causes of Impaired Sperm Motility
- Diagnosing Sperm Motility Issues: The Semen Analysis
- Strategies for Improving Sperm Motility and Fertility
- Frequently Asked Questions (FAQs)
- Conclusion
Understanding Sperm Motility: The Foundation of Fertilisation
Sperm motility refers to the capacity of sperm to move efficiently and effectively. It’s not merely about wiggling; it’s about directed, forward motion that propels the sperm towards the egg. This essential characteristic is meticulously assessed during a semen analysis, providing vital insights into a man's reproductive health. The journey of sperm from ejaculation through the cervix, uterus, and into the fallopian tube is arduous, requiring immense energy and precise navigation. Only the most robust and motile sperm are typically capable of completing this incredible odyssey.
The Two Primary Types of Sperm Motility
When assessing sperm movement, laboratory specialists primarily distinguish between two main types of motility, which describe how each individual sperm swims:
- Progressive Motility: This is the gold standard for sperm movement. It signifies that the sperm are swimming predominantly in a straight line or in large, purposeful circles, indicating effective forward progression. For sperm to successfully navigate the challenging environment of the female reproductive tract and eventually fertilise an egg, they must exhibit strong progressive motility. A minimum speed of at least 25 micrometres per second is considered essential for them to pass through the cervical mucus and continue their journey.
- Non-Progressive Motility: In contrast, non-progressive motility means that while sperm are indeed moving, their motion lacks forward direction. They might move their tails or oscillate, but they remain largely in the same spot, moving in irregular paths or tight, confined circles. While such sperm are technically 'motile', their inability to advance significantly hinders their capacity to reach the egg.
Why Sperm Motility Matters for Conception
The direct impact of sperm motility on fertility cannot be overstated. Simply put, if sperm are unable to swim effectively within the female reproductive tract, their chances of reaching and fertilising an ovum or egg become significantly diminished. The path to the egg is long and challenging, requiring sperm to travel from the cervix, through the uterus, and then into the fallopian tube. Sperm that lack good motility and fail to move rapidly may simply be unable to cover this distance in time, or at all.
It's fascinating to note how the female body also plays a supportive role in this process. During ovulation, the cervix softens and opens, the pH levels of the cervical mucus become less acidic, and the mucus itself becomes more slippery. These physiological changes create a more hospitable environment, allowing sperm to move more freely and efficiently towards their target. However, even with these favourable conditions, the inherent ability of the sperm to move remains paramount.
While sperm motility is a critical factor, it is important to understand that it is not the sole criterion considered when evaluating overall sperm health. Other vital parameters, such as the total number of sperm, their shape (morphology), and the sperm concentration, are also meticulously examined to provide a comprehensive picture of male fertility.
Defining 'Normal': What Healthy Sperm Motility Looks Like
For couples trying to conceive, understanding what constitutes 'normal' sperm motility is key. According to the World Health Organisation’s (WHO) Handbook for Semen Analysis, updated in 2021, specific benchmarks are used to evaluate sperm quality in healthy males:
- Approximately 42% or more of sperm should exhibit complete motility, meaning there is some form of movement, even if it's in small circles.
- Crucially, at least 30% or more of sperm must demonstrate progressive motility, indicating they are moving forward in a linear path or large circles.
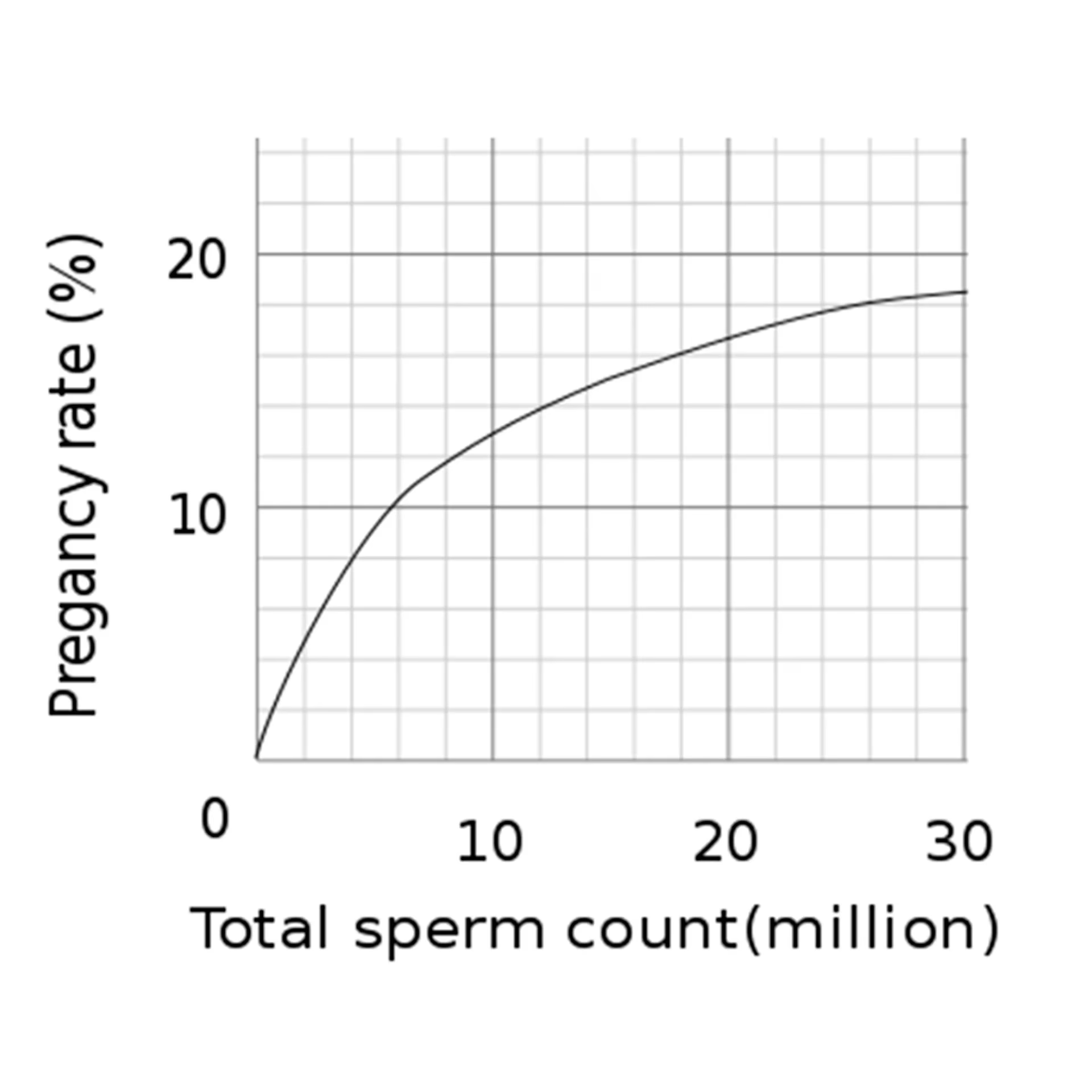
In terms of absolute numbers, a count of above twenty million motile sperm is generally regarded as normal. It's an interesting point to note that while a higher motile sperm count above twenty million is positive, it does not necessarily translate directly to a higher likelihood of achieving pregnancy. However, having fewer than twenty million motile sperm can significantly result in lower chances of conceiving naturally. For assisted reproductive techniques, such as in-vitro fertilisation (IVF) with or without intracytoplasmic sperm injection (ICSI) or for intrauterine insemination (IUI), a sperm count of five million and above can still be viable.
Normal Semen Analysis Report Values
A basic semen analysis is the diagnostic cornerstone for investigating the most significant indicators of sperm health. Here’s a summary of normal values often observed in a comprehensive report:
| Test | Normal Values |
|---|---|
| Sperm Count | 40 million or more |
| Volume | 2.0 mL or higher |
| Total Motility | 40% or higher |
| Sperm Concentration | 20 million or more per mL |
| Morphology (% of normal-appearing sperm) | 4% or more normal |
| Total Progressive Motility | 32% or higher |
The Motility Grading System
For a more detailed assessment, a thorough semen analysis classifies sperm motility into specific grades:
- Grade A: Fast Progressive Sperm – These are the most efficient swimmers, moving quickly and in a straightforward, linear direction. They are the most likely to reach and fertilise the egg.
- Grade B: Slow Progressive Sperm – While these sperm are moving forward, their progression is less direct or somewhat erratic. They still contribute to the motile count but are less efficient than Grade A sperm.
- Grade C: Non-Progressive Sperm – Sperm in this category can move their tails but are unable to move forward effectively. They may oscillate or move in tight circles, staying largely in one place.
- Grade D: Immotile Sperm – These sperm show no movement at all.
Grades C and D are generally considered indicators of poor sperm quality, suggesting that the testicles may not be functioning optimally in producing healthy, motile sperm.
Asthenozoospermia: When Sperm Motility is Low
The condition where less than 32% of sperm can move efficiently is medically termed asthenozoospermia, or more commonly, poor sperm motility. This means that a significant proportion of the sperm sample either moves too slowly or does not move in a forward direction, severely impeding their ability to reach the egg.
When sperm motility is low, it does not necessarily mean that fertilisation is impossible, but it undeniably complicates the process and can significantly affect male fertility. It is crucial to differentiate low sperm motility from a low sperm count (oligospermia), although these two conditions are often closely related and can even coincide. A man might have a sufficient number of sperm but poor motility, or a low count with good motility, or indeed a combination of both. In any scenario where fertility problems arise, it's imperative to conduct a comprehensive male fertility assessment, as sperm defects are estimated to be the primary cause in about 25% of couples experiencing difficulties conceiving.
As part of a fertility study, a semen analysis (seminogram) is the standard test to check sperm motility. This involves the man providing a semen sample, typically obtained by masturbation, which is then sent to a laboratory for detailed analysis. The laboratory assesses not only how sperm move and in what direction, but also other parameters like semen volume and pH, providing a holistic view of sperm health.
Unravelling the Causes of Impaired Sperm Motility
Several factors, ranging from biological predispositions to lifestyle choices and environmental exposures, can adversely affect sperm motility:
Biological & Medical Factors
- Genetic Predisposition: Some males may inherit genetic traits that lead to inherently lower sperm motility.
- Structural and Anatomical Issues: Conditions such as varicocele (enlarged veins in the scrotum), cryptorchidism (undescended testes), or testicular injury can impair sperm production and movement.
- Infections: Past or present infections within the reproductive tract can cause inflammation and damage to sperm-producing tissues, affecting motility.
- Malignancy or Surgery: Certain cancers or previous surgical procedures in the pelvic or scrotal area can have an impact.
- Hormonal Imbalances: Abnormal levels of hormones essential for sperm production, such as testosterone, can lead to poor motility.
- Anti-Sperm Antibodies: Though relatively rare, some men's immune systems produce antibodies that mistakenly attack and damage their own sperm, hindering their movement.
- Gluten Intolerance: Emerging research suggests a potential link between gluten intolerance and fertility issues, including impaired sperm motility, though more studies are needed.
Lifestyle & Environmental Influences
- Smoking: This is a particularly detrimental habit. Studies have consistently linked tobacco use to diminished sperm motility, with a notable impact observed in men who consume more than ten cigarettes daily. Beyond motility, smoking has also been associated with a range of DNA alterations within sperm, which can unfortunately lead to complications such as miscarriages and difficulties in conceiving.
- Alcohol and Drugs: Excessive alcohol consumption and recreational drug use can significantly impair sperm quality, including motility.
- Being Overweight or Obese: Excess body fat can disrupt hormonal balance, leading to reduced sperm quality and motility.
- Chronic Stress: Prolonged psychological stress has been shown to negatively impact reproductive hormones and sperm parameters.
- Exposure to Toxins: Environmental toxins, such as heavy metals (e.g., lead or cadmium), pesticides, and certain industrial chemicals, can be detrimental to sperm health.
- Excessive Heat: Testicles require a cooler temperature than the rest of the body for optimal sperm production. Exposure to excessive heat from sources like fevers, tight-fitting clothing, prolonged sitting (common for taxi drivers), working in very hot environments (e.g., kitchens, hairdressers), or frequent use of saunas and jacuzzis can negatively affect motility.
- Certain Medications: Some pharmaceuticals, notably anabolic steroids, can severely suppress natural sperm production and motility.
Diagnosing Sperm Motility Issues: The Semen Analysis
The definitive method for determining sperm motility and other vital sperm parameters is a standard semen analysis. For this diagnostic test, you will need to provide a sperm specimen. This is most commonly obtained by masturbation at a doctor's office or a dedicated testing centre to ensure the sample's integrity and timely delivery to the laboratory. Alternatively, a specimen can sometimes be collected using a special condom during intercourse or via the withdrawal method, though these methods are less common for initial diagnostic purposes.
Crucially, the collected sample must be kept at room temperature and submitted to the laboratory within 30 to 60 minutes to ensure the viability and accuracy of the sperm motility assessment. Once analysed, if the progressive sperm motility is found to be less than 32% (or total motility less than 40%), you would typically be diagnosed with low sperm motility.
Beyond motility, your doctor will also utilise the semen analysis to assess other critical indicators of male fertility, including sperm count (the total number of sperm per ejaculation) and sperm concentration (the number of sperm per millilitre of semen), among other factors.
Strategies for Improving Sperm Motility and Fertility
If you or your partner receive a diagnosis of low sperm motility, it is paramount to consult your doctor. This is because there could be an underlying medical condition, such as a varicocele or hormonal imbalances, that requires specific treatment. If an underlying medical condition is identified, treatment will be tailored accordingly.
However, irrespective of an underlying medical cause, several lifestyle modifications can significantly enhance overall sperm and reproductive health, often leading to improved motility:
Lifestyle and Dietary Modifications
- Regular Exercise and Healthy Weight: Maintaining a healthy body weight through consistent physical activity can positively influence hormonal balance and sperm quality.
- Limit Smartphone Exposure: While direct scientific evidence is still accumulating, some studies suggest that keeping smartphones away from the testicles (e.g., not in trouser pockets) may be beneficial due to potential electromagnetic radiation.
- Reduce Alcohol Consumption and Quit Smoking: As highlighted earlier, tobacco and excessive alcohol are significantly detrimental to sperm health. Quitting smoking and moderating alcohol intake can lead to notable improvements.
- Stress Management: Chronic stress can negatively impact fertility. Incorporating stress-reducing activities like meditation, yoga, or hobbies can be beneficial.
- Keep Testicles Cool: Opt for loose-fitting underwear (e.g., boxers) instead of briefs, and avoid prolonged hot baths, saunas, or very hot work environments to maintain optimal testicular temperature.
- Adopt a Healthy Diet: A balanced diet is crucial. Avoid highly processed meats (like salami or sausages) and trans fats (found in many industrial sweets and frozen pizzas), which have been linked to lower sperm counts and motility. Similarly, limit high-fat dairy products and excessive soy, which contains phytoestrogens. Instead, increase your intake of:
- Oily Fish: Rich in omega-3 fatty acids (e.g., tuna, mackerel, salmon, trout).
- Fresh Fruit and Vegetables: Packed with vitamins and antioxidants that protect cells from damage and boost sperm count and quality.
- Whole Grains and Nuts: Provide essential nutrients and fibre.
Supplements
Discuss with your doctor about specific nutritional supplements that may support sperm motility. Certain supplements, such as L-carnitine, coenzyme Q10, and vitamins A, E, C, or D, are often regarded as beneficial for improving sperm parameters due to their antioxidant properties and roles in cellular energy production.
Medical and Surgical Treatment
Even when lifestyle changes are insufficient or when the causes of impaired sperm motility are beyond individual control, advanced medical and surgical treatments offer hope:
- Addressing Underlying Conditions: If varicocele or low hormone levels are diagnosed, specific medical or surgical interventions can often correct these issues and subsequently improve sperm motility.
- Conjugal Artificial Insemination (IUI): This is often a first-line assisted reproductive technique for men with mild oligospermia and somewhat decreased motility. IUI involves depositing sperm directly into the woman’s uterus, significantly shortening the distance the sperm need to travel and bypassing the cervical mucus barrier. It is a relatively simple and painless procedure.
- In Vitro Fertilisation (IVF) using the Partner’s Sperm: IVF is highly recommended when semen analysis parameters are significantly impaired. It offers the highest success rates among assisted reproductive technologies. In IVF, eggs are retrieved from the woman and fertilised with the partner's sperm outside the body in a laboratory setting. Once healthy embryos develop, they are then implanted into the woman's uterus. IVF, particularly when combined with Intracytoplasmic Sperm Injection (ICSI), where a single sperm is injected directly into an egg, can overcome even severe motility issues.
Frequently Asked Questions (FAQs)
Q: What is the minimum sperm motility for pregnancy?
A: According to WHO guidelines, for natural conception, at least 30% of sperm should exhibit progressive motility (forward movement). Additionally, sperm must move at a minimum speed of approximately 25 micrometres per second to effectively pass through cervical mucus.
Q: Can I improve my sperm motility naturally?
A: Yes, many lifestyle modifications can significantly help. These include adopting a healthy diet rich in fruits, vegetables, and omega-3s, engaging in regular exercise, maintaining a healthy weight, avoiding smoking and excessive alcohol, managing stress, and wearing loose underwear to keep the testicles cool. Discussing beneficial supplements with your doctor can also be helpful.
Q: Does low sperm motility mean I can't have children?
A: Not necessarily. While low sperm motility (asthenozoospermia) can make natural conception more challenging, it does not mean you cannot father children. Assisted reproductive technologies (ARTs) like Intrauterine Insemination (IUI) or In Vitro Fertilisation (IVF), especially with ICSI, can significantly increase your chances of conception by bypassing the need for extensive sperm movement.
Q: How soon can sperm motility improve after lifestyle changes?
A: The entire process of sperm production (spermatogenesis) takes approximately 72 days. Therefore, you should typically expect to see significant improvements in sperm quality and motility after consistently implementing lifestyle changes for at least 2 to 3 months.
Conclusion
Male fertility is a complex interplay of various factors, with sperm motility standing out as a critically important aspect. While the ability of sperm to move efficiently is paramount for natural conception, it's reassuring to know that even with limited sperm motility, pregnancy can still occur, particularly with the aid of modern reproductive technologies. These advancements, such as IVF or IUI, effectively circumvent the requirement for sperm to move extensively on their own, thereby enhancing the likelihood of conception for many couples.
If you and your partner have been trying to conceive for 12 months or more without success, it is always advisable to consult your doctor. A healthcare professional can conduct thorough tests on both you and your partner to identify any underlying fertility-related health issues. Based on the findings, your doctor will be able to guide you on the most appropriate next steps and tailored treatment options to help you achieve your dream of starting a family.
If you want to read more articles similar to Sperm Motility: Your Guide to Male Fertility, you can visit the Automotive category.
