03/07/2017
In the intricate machinery of the human body, blood plays an absolutely vital role, akin to the oil circulating through an engine – it delivers essential components and removes waste. Just as there are different types of lubricants for various engines, human blood isn't a singular entity. It’s categorised into distinct types, a fundamental classification system that ensures safety in medical procedures like transfusions and organ transplants. Understanding these classifications isn't merely academic; it’s a cornerstone of modern medicine, preventing potentially fatal reactions and safeguarding lives. This comprehensive guide will navigate the fascinating landscape of blood types, focusing on the eight most common variants and their profound implications.
- What Are Blood Types?
- How Are Blood Types Determined?
- The Importance of Blood Type Compatibility
- Inheriting Your Blood Type
- Rare Blood Types: The "Golden Blood"
- Why Should You Know Your Blood Type?
- How Can You Discover Your Blood Type?
- Frequently Asked Questions
- Q: Do blood types ever change over a person's lifetime?
- Q: Are some blood types more common than others globally?
- Q: What is the difference in compatibility for donating plasma versus whole blood?
- Q: Is blood type important for organ transplants as well as blood transfusions?
- Q: Can I donate blood if I don't know my blood type?
What Are Blood Types?
A blood type is essentially a classification system that allows healthcare professionals to determine whether one person's blood is compatible or incompatible with another's. This compatibility is paramount for safe blood transfusions and organ transplants. The determination of your blood type hinges on specific markers, known as antigens, found on the surface of your red blood cells, and the presence or absence of a particular protein called the Rh factor.
The ABO System: Antigens A, B, and O
When most people hear "blood types," their minds immediately go to A, B, AB, and O. This is known as the ABO blood group system, and it classifies blood based on the presence of two primary antigens: Antigen A and Antigen B. Your red blood cells either have Antigen A, Antigen B, both, or neither:
- Type A: Your red blood cells carry the A antigen.
- Type B: Your red blood cells carry the B antigen.
- Type AB: Your red blood cells possess both A and B antigens.
- Type O: Your red blood cells have neither A nor B antigens.
Crucially, your immune system produces antibodies against the antigens you *don't* have. For instance, a person with Type A blood will have anti-B antibodies, which would attack Type B blood. A person with Type O blood, having neither A nor B antigens, will produce both anti-A and anti-B antibodies, making them particularly sensitive to A or B blood types.
The Rh System: Positive or Negative
Beyond the ABO system, blood types are further refined by the presence or absence of another critical protein: the Rh factor, specifically the RhD antigen. This is why you hear of blood types being "positive" or "negative."
- Positive (+): If your red blood cells possess the RhD antigen, your blood type is classified as positive.
- Negative (-): If your red blood cells do not have the RhD antigen, your blood type is classified as negative.
The RhD antigen is highly significant, particularly in pregnancy, which we'll explore in more detail later. Approximately 85% of the global population is Rh positive.
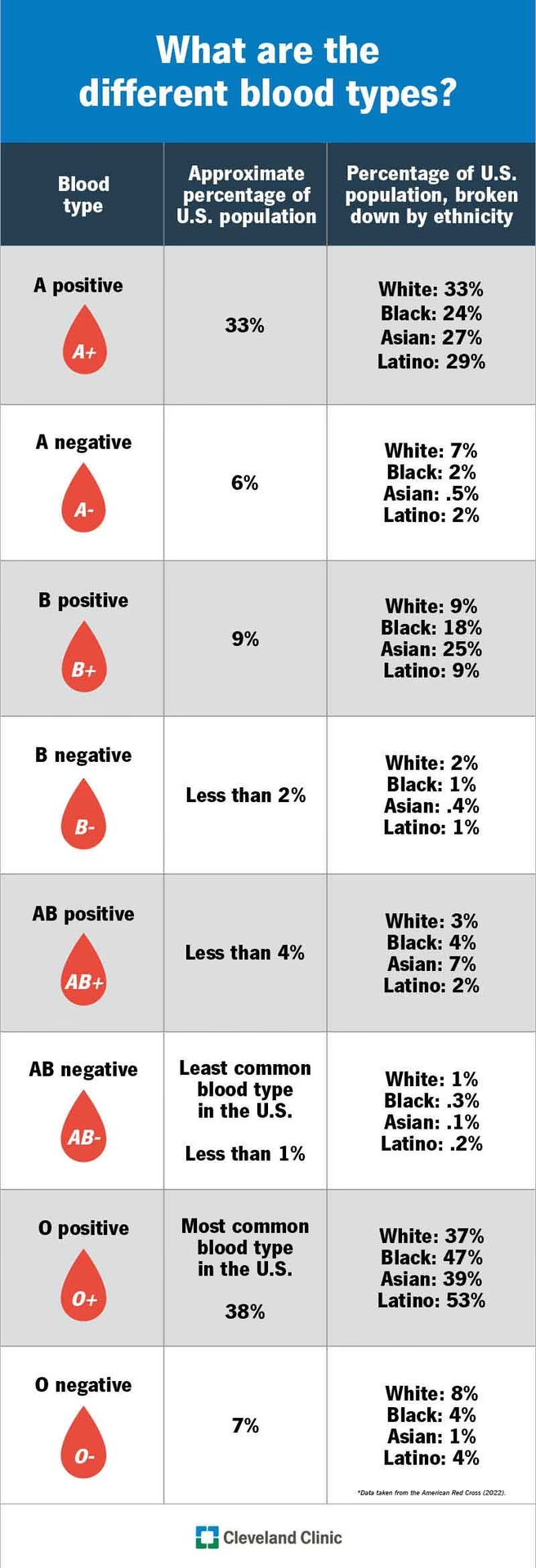
The Eight Common Blood Types
Combining the ABO and Rh systems yields the eight most common blood types that are routinely identified and categorised in healthcare settings:
- A positive (A+)
- A negative (A-)
- B positive (B+)
- B negative (B-)
- AB positive (AB+)
- AB negative (AB-)
- O positive (O+)
- O negative (O-)
While these are the most commonly recognised, it's important to note that the human blood system is far more complex. The International Society of Blood Transfusion has identified over 45 different blood group systems, encompassing hundreds of unique antigens beyond the ABO and RhD. However, for everyday medical practice, especially transfusions, the eight primary types are the critical focus due to their widespread clinical relevance.
How Are Blood Types Determined?
Determining a person's blood type is a precise laboratory procedure, typically performed by blood bank specialists. The process involves identifying the specific antigens present on the surface of your red blood cells. A small blood sample is taken, and then mixed with various reagents containing known antibodies.
For instance, to identify ABO type, your blood sample is mixed with anti-A antibodies and anti-B antibodies. If your blood agglutinates (clumps) when mixed with anti-A antibodies, it means your red blood cells have A antigens. If it clumps with anti-B, you have B antigens. If it clumps with both, you have AB. If it clumps with neither, you are Type O.
Similarly, to determine the Rh factor, your blood is mixed with anti-D antibodies. If clumping occurs, you are Rh positive. If no clumping occurs, you are Rh negative. This careful process ensures accurate typing, which is paramount for patient safety during transfusions.
The Importance of Blood Type Compatibility
The concept of blood compatibility is perhaps the most critical aspect of blood typing. If a patient receives blood from a donor whose blood cells contain antigens their immune system doesn't recognise, a severe immune response can be triggered. This is known as a haemolytic transfusion reaction, where the recipient's antibodies attack and destroy the transfused red blood cells. Such reactions can range from mild to life-threatening, causing fever, chills, kidney failure, and even death. Therefore, meticulous cross-matching is always performed before any transfusion.

Universal Donor and Universal Recipient
Within the spectrum of blood types, two stand out for their unique compatibility properties:
- O Negative (O-): The Universal Donor
Blood type O negative is often referred to as the universal donor because it lacks A, B, and RhD antigens. This means it carries no markers that would typically trigger an immune response in a recipient. In emergency situations, when there's no time to cross-match blood, O negative blood is often transfused because it has the lowest risk of causing an adverse reaction. However, O negative individuals can only receive O negative blood themselves, as their immune system would react to any A, B, or RhD antigens. - AB Positive (AB+): The Universal Recipient
Conversely, blood type AB positive is known as the universal recipient. Individuals with AB+ blood have both A and B antigens, as well as the RhD antigen, on their red blood cells. This means their immune system recognises all these common antigens as 'self' and will not produce antibodies against them. Consequently, AB+ individuals can safely receive blood from any other blood type, making them incredibly flexible recipients.
It's worth noting that while O negative is the universal red blood cell donor, the compatibility for plasma donation is different. Plasma is the liquid component of blood, and its compatibility is determined by the absence of antibodies. Type AB plasma is considered the universal plasma donor because it contains neither anti-A nor anti-B antibodies.
Blood Type Compatibility Chart
The following table illustrates the complex but vital rules of blood type compatibility for red blood cell transfusions:
| Your Blood Type | Compatible with Donor Blood Types (You can receive) | Blood Types You Can Donate To |
|---|---|---|
| A+ | A+, A-, O+, O- | A+, AB+ |
| A- | A-, O- | A-, A+, AB-, AB+ |
| B+ | B+, B-, O+, O- | B+, AB+ |
| B- | B-, O- | B-, B+, AB+, AB- |
| AB+ | All blood types (Universal Recipient) | AB+ |
| AB- | AB-, A-, B-, O- | AB-, AB+ |
| O+ | O+, O- | O+, A+, B+, AB+ |
| O- | O- | All blood types (Universal Donor) |
This table assumes compatibility across the less common non-ABO blood group antigen systems as well, which are also considered during detailed cross-matching procedures.
Inheriting Your Blood Type
Your blood type, much like your eye colour or hair texture, is a genetic trait inherited from your biological parents. Both the ABO genes and the Rh factors are passed down through specific genetic combinations. Each parent contributes one gene for the ABO system and one for the Rh factor, leading to a variety of possible outcomes for the child's blood type. Because of these many combinations, it's entirely possible for a child not to have the exact same blood type as either parent, though it will always be a genetically explainable combination of their parents' types.
Rare Blood Types: The "Golden Blood"
While the eight common blood types cover the vast majority of the population, there exist numerous other blood group systems involving over 600 different antigens that can attach to red blood cells. These variations lead to what are considered rare blood types. A general definition of a rare blood type is one that occurs in fewer than 1 per 1,000 people.
Some examples of these rarer blood group systems include the Duffy blood group, the K antigen (or Kell) group, the Lutheran blood group, and the Kidd blood group. The most common rare types in the UK and US include AB negative (around 0.6% of the population) and B negative (around 1.5%).
One of the world's rarest and most intriguing blood types is Rh-null, sometimes referred to as "golden blood." This incredibly rare blood type lacks all Rh antigens, not just the RhD antigen. Fewer than 50 people worldwide are known to possess this blood type, making it extraordinarily precious. While individuals with Rh-null blood can donate to almost anyone with an Rh deficiency (even those with other rare Rh types), they can only receive Rh-null blood themselves. This makes finding compatible blood for them a significant challenge, often requiring international collaboration and blood bank networks.
Why Should You Know Your Blood Type?
Knowing your blood type isn't just a piece of interesting personal information; it holds significant medical importance for several reasons.
Transfusions and Medical Procedures
The most immediate and critical reason to know your blood type is for safe blood transfusions. In emergencies, such as severe injury or during complex surgeries, rapid access to compatible blood can be life-saving. While hospitals always perform blood typing and cross-matching before a transfusion, knowing your type can provide crucial information quickly, especially if you carry your medical details. Beyond transfusions, organ transplants also demand strict blood type compatibility to prevent rejection, highlighting the pervasive role of blood typing in advanced medical interventions.
Pregnancy and Rh Incompatibility
For pregnant individuals, particularly those who are Rh negative, knowing their blood type is paramount. If an Rh negative pregnant person is carrying an Rh positive foetus (inherited from an Rh positive partner), a condition called Rh incompatibility can arise. This typically doesn't affect the first pregnancy, but during birth, foetal and maternal blood can mix, leading the Rh negative mother's immune system to develop antibodies against the RhD antigen. These antibodies can then cross the placenta in subsequent pregnancies and attack the red blood cells of an Rh positive foetus, leading to a serious condition known as haemolytic disease of the foetus and newborn (HDFN). HDFN can cause severe anaemia, jaundice, brain damage, or even stillbirth or neonatal death. Fortunately, this can be prevented by administering RhoGAM (a Rho(D) immune globulin) to the Rh negative mother at specific points during pregnancy and after delivery, which prevents the formation of these harmful antibodies.

Health Insights
Emerging research also suggests potential links between blood types and susceptibility to certain health conditions. For example, studies have indicated that people with certain blood types may have a slightly higher or lower risk of developing conditions like kidney stones, pre-eclampsia (high blood pressure during pregnancy), or specific bleeding disorders. Furthermore, some research during the COVID-19 pandemic suggested that individuals with blood group O might have a slightly lower likelihood of infection compared to those with blood group A, though more extensive research is ongoing in this area. While these associations are not definitive diagnostic tools, they contribute to a broader understanding of human health and genetics.
How Can You Discover Your Blood Type?
There are several straightforward ways to find out your blood type:
- Ask Your Doctor: Your general practitioner or healthcare provider may have your blood type on record from previous medical tests or procedures.
- Donate Blood: Volunteering to donate blood is an excellent way to learn your type, and it contributes to a vital public service. Blood donation centres routinely type all donated blood, and they will typically inform you of your blood type after your donation has been processed.
- At-Home Test Kits: Various at-home blood typing kits are available for purchase. These kits usually involve pricking your finger and placing blood drops on a special card treated with antibodies. While generally accurate if performed correctly, professional laboratory testing remains the most reliable method, especially for critical medical decisions.
It's important to remember that while your blood type is a lifelong characteristic and does not change, medical facilities will always perform a new blood type test and cross-match before any transfusion, regardless of your previously known type. This rigorous double-check is a critical safety measure.
Frequently Asked Questions
Q: Do blood types ever change over a person's lifetime?
A: No, your blood type is determined by the genes you inherit from your parents and remains constant throughout your life. It does not change due to diet, environment, or illness. The only rare exceptions might involve bone marrow transplants for certain medical conditions, where the recipient's blood type could potentially change to that of the donor.
Q: Are some blood types more common than others globally?
A: Yes, the prevalence of different blood types varies across populations and geographical regions. Globally, O positive is often the most common blood type, followed by A positive. AB negative is consistently among the rarest worldwide. For instance, in the United States, O positive accounts for about 37.4% of the population, while AB negative is only about 0.6%.
Q: What is the difference in compatibility for donating plasma versus whole blood?
A: When donating whole blood, the compatibility is primarily determined by the antigens on the red blood cells (ABO and Rh systems). For plasma donation, compatibility is based on the antibodies present in the plasma. Type AB plasma is considered the universal donor for plasma because it lacks both anti-A and anti-B antibodies, meaning it can be safely given to recipients of any ABO blood type.
Q: Is blood type important for organ transplants as well as blood transfusions?
A: Absolutely. Blood type compatibility is a crucial factor in organ transplantation. If the donor and recipient have incompatible blood types, the recipient's immune system will recognise the transplanted organ as foreign and launch a severe immune attack, leading to immediate organ rejection. This is why extensive testing, including blood typing and cross-matching, is performed rigorously before any organ transplant procedure.
Q: Can I donate blood if I don't know my blood type?
A: Yes, you can. Blood donation centres always perform blood typing on every unit of donated blood as part of their standard processing. So, even if you don't know your type beforehand, they will determine it for you, and you will typically be informed of your blood type after your donation.
In conclusion, the system of blood typing is far more than just a biological curiosity; it is a fundamental pillar of medical safety and preparedness. From ensuring safe blood transfusions in emergencies to preventing complications in pregnancy, understanding these eight common blood types is indispensable. Whether you're a potential donor, a recipient, or simply curious about the amazing complexities of the human body, knowing about blood types empowers you with vital knowledge that can, quite literally, make the difference between life and death. So, if you haven't already, consider finding out your blood type – it’s a small piece of information with immense significance.
If you want to read more articles similar to Understanding Your Blood: The Eight Key Types, you can visit the Automotive category.

