23/08/2008
Understanding your blood type is more than just a medical curiosity; it's a vital piece of information that plays a crucial role in blood transfusions and overall health. While we often hear about A, B, AB, and O, the reality of blood typing is far more complex and fascinating. This guide will delve into the intricacies of blood group systems, explore common and rare types, and explain the significance of this biological information.
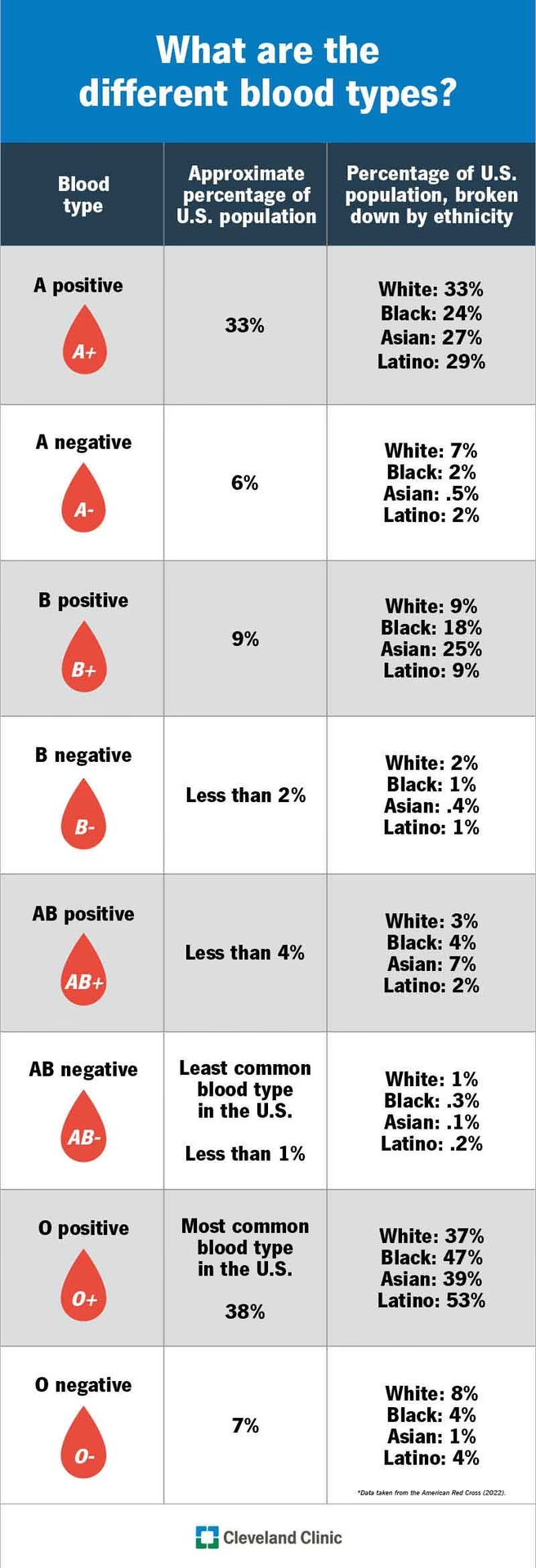
- The ABO Blood Group System: The Foundation of Compatibility
- The Rh System: Adding Another Layer of Complexity
- Common vs. Rare Blood Types: Who's Who?
- Beyond ABO and Rh: A World of Blood Types
- Why Knowing Your Blood Type Matters
- Finding Compatible Donors for Rare Blood Types
- Frequently Asked Questions (FAQs)
The ABO Blood Group System: The Foundation of Compatibility
The most significant and widely recognised blood-typing system is the ABO system. This system categorises blood based on the presence or absence of specific antigens on the surface of red blood cells. Antigens are like unique markers that can trigger an immune response if they are foreign to the body. The ABO system identifies four main blood groups:
- Type A: Has A antigens on red blood cells and anti-B antibodies in plasma.
- Type B: Has B antigens on red blood cells and anti-A antibodies in plasma.
- Type AB: Has both A and B antigens on red blood cells, but no anti-A or anti-B antibodies in plasma.
- Type O: Has neither A nor B antigens on red blood cells, but has both anti-A and anti-B antibodies in plasma.
The interaction between antigens on the donor's red blood cells and antibodies in the recipient's plasma is what determines compatibility. Introducing incompatible blood can lead to a severe and potentially fatal immune reaction, known as a transfusion reaction. This is why blood typing is a critical step before any transfusion.
The Rh System: Adding Another Layer of Complexity
Beyond the ABO system, the Rh system is the second most important in blood transfusions. This system is based on the presence or absence of the RhD antigen. If the RhD antigen is present, the blood type is considered Rh-positive (Rh+). If it's absent, the blood type is Rh-negative (Rh-).
Combining the ABO and Rh systems gives us the eight common blood types:
| ABO Group | Rh Factor | Commonality |
|---|---|---|
| O | + | Most Common |
| O | - | Common |
| A | + | Common |
| B | + | Less Common |
| A | - | Less Common |
| AB | + | Rare |
| B | - | Rare |
| AB | - | Rarest |
The Rh factor is particularly important during pregnancy. If an Rh-negative mother carries an Rh-positive baby, her immune system can develop antibodies against the baby's blood, potentially leading to haemolytic disease of the newborn in subsequent pregnancies. This is why Rh status is carefully monitored.
Common vs. Rare Blood Types: Who's Who?
While there are more than 33 recognised blood types and numerous other antigen systems, the ABO and Rh systems account for the vast majority of transfusable blood. Within these systems, there's a significant variation in prevalence across populations.
The Most Common Blood Type: O-Positive
Globally, O-positive (O+) is the most prevalent blood type, found in a significant portion of the world's population. Individuals with O+ blood can receive red blood cells from O+, O-, A+, A-, B+, B-, AB+, and AB-. This broad compatibility makes O+ a highly valuable blood type. However, O+ individuals can only donate to other Rh-positive recipients (A+, B+, AB+, O+).
The Universal Recipient: AB-Positive
Conversely, AB-positive (AB+) is often referred to as the "universal recipient." This is because individuals with AB+ blood have both A and B antigens and lack both anti-A and anti-B antibodies in their plasma. This means they can receive red blood cells from any ABO blood group, regardless of the Rh factor. However, AB+ individuals can only donate to other AB+ recipients.
The Universal Donor: O-Negative
On the other end of the spectrum is O-negative (O-). People with O- blood are considered the "universal red blood cell donors." They lack both A and B antigens, as well as the RhD antigen. This absence of common antigens means their red blood cells are less likely to trigger an immune response in recipients with different blood types. Therefore, O- blood can be transfused to individuals of any ABO and Rh group. However, O- individuals can only receive red blood cells from other O- donors, making them highly reliant on the generosity of others with the same rare type.
The Rarest Blood Type: AB-Negative
The rarest blood type among the commonly recognised groups is AB-negative (AB-). Constituting a tiny fraction of the global population (often cited as less than 1%), AB- individuals are universal recipients, meaning they can receive from all blood types. However, their rarity means they can only donate to other AB- individuals, highlighting the importance of their specific blood donations being available.
Beyond ABO and Rh: A World of Blood Types
While the ABO and Rh systems are paramount for transfusions, it's important to acknowledge that there are many other blood group systems. These include the Kell, Kidd, and Duffy systems, among others, each with its own set of antigens. While these systems are not as critical for routine transfusions, they can become significant in specific situations, such as for individuals requiring frequent transfusions or those with rare blood types who may develop antibodies to less common antigens.

The complexity of these additional systems means that compatibility can extend beyond the basic ABO and Rh factors. For example, someone with a rare antigen deficiency might only be able to receive blood from donors who also lack that specific antigen.
Why Knowing Your Blood Type Matters
Understanding your blood type is crucial for several reasons:
- Emergency Situations: In emergencies where immediate transfusion is necessary and there isn't time for full cross-matching, universal donor blood (O-) is used for red blood cell transfusions, and universal recipient plasma (AB) is used for plasma transfusions. Knowing your type can help medical professionals make quicker decisions.
- Pregnancy: As mentioned, Rh incompatibility can pose risks during pregnancy. Knowing your Rh status is vital for proper prenatal care.
- Organ Donation: Blood type compatibility is also a factor in organ transplantation, although tissue typing is more comprehensive.
- Personal Health: Some research suggests potential links between blood types and certain health conditions, although more studies are needed to establish definitive connections.
Finding Compatible Donors for Rare Blood Types
For individuals with rare blood types, finding compatible donors can indeed be a challenge. Fortunately, several avenues exist to facilitate this:
- National and International Donor Registries: Many countries maintain registries of blood donors, including those with rare blood types. These registries allow individuals to register their blood type and be contacted if a match is found.
- Directed Donation Programs: These programs allow individuals to donate blood specifically for a known recipient. This is particularly helpful for those with rare blood types who need a precise match.
- Cord Blood Banking: Cord blood, collected from the umbilical cord and placenta after birth, is rich in stem cells and can be stored in private or public banks. Cord blood is generally more compatible across different blood types than adult blood and can be a valuable resource.
- Awareness Campaigns: Raising awareness about the need for donations from individuals with rare blood types is crucial. Many organisations actively recruit donors with specific blood types to build a more comprehensive donor pool.
The global community of blood donors is a testament to human generosity. Even with the complexities of blood typing, the collective effort ensures that life-saving transfusions are available to those who need them.
Frequently Asked Questions (FAQs)
What is the most common blood type in the UK?
While O+ is the most common globally, specific prevalence can vary by region. Generally, O+ and A+ are the most common blood types in the UK.
Can I donate blood if I have a rare blood type?
Absolutely! Your donation is incredibly valuable, especially if you have a rare blood type. Registering with a blood donation service will allow them to contact you when a match is needed.
What is the difference between ABO and Rh systems?
The ABO system categorises blood based on A and B antigens, determining if you have anti-A or anti-B antibodies. The Rh system is based on the presence or absence of the RhD antigen, determining if your blood is positive or negative.
Why is O- blood called the universal donor?
O- blood is called the universal donor because it lacks the A, B, and RhD antigens on its red blood cells. This means it is less likely to be rejected by a recipient's immune system, making it compatible with all blood types in emergencies.
Can someone with AB- blood donate to anyone?
No, individuals with AB- blood are universal recipients, meaning they can receive blood from all types. However, they can only donate blood to other individuals with AB- blood, as they possess both A and B antigens and the RhD antigen.
How do I find out my blood type?
You can discover your blood type through a simple blood test administered by a healthcare professional. Many home blood typing kits are also available for purchase, offering a convenient way to learn your blood type.
If you want to read more articles similar to Understanding Blood Types: A Comprehensive Guide, you can visit the Automotive category.

