07/12/2012
- What Exactly Are Beta-Blockers?
- Indications: Why Are Beta-Blockers Prescribed?
- How Do Beta-Blockers Work?
- Potential Side Effects of Beta-Blockers
- Drug Interactions: What to Watch Out For
- Special Populations
- When to Seek Medical Advice for Side Effects
- Important Considerations and Precautions
- Economic Impact
What Exactly Are Beta-Blockers?
Beta-blockers, also known as beta-adrenergic blocking agents, are a class of medications that play a crucial role in managing a variety of cardiovascular conditions. They work by blocking the effects of stress hormones like adrenaline (epinephrine) and noradrenaline (norepinephrine) on the body's beta receptors. These receptors are found throughout the body, including in the heart, blood vessels, and lungs. By blocking these receptors, beta-blockers essentially 'calm' the heart and reduce the impact of stress on the cardiovascular system.
The primary mechanism of action involves slowing down the heart rate, reducing the force of the heart's contractions, and lowering blood pressure. This makes them invaluable in treating conditions such as hypertension (high blood pressure), angina (chest pain), heart failure, and certain heart rhythm disturbances (arrhythmias). Beyond their cardiac benefits, beta-blockers also find utility in managing conditions like glaucoma, migraines, essential tremors, and even symptoms associated with anxiety and hyperthyroidism.
Indications: Why Are Beta-Blockers Prescribed?
The versatility of beta-blockers means they are prescribed for a wide array of medical conditions. Here are the primary indications:
- Hypertension: By reducing heart rate and contractility, beta-blockers effectively lower blood pressure.
- Angina Pectoris: They reduce the heart's workload and oxygen demand, thereby preventing or relieving chest pain caused by insufficient blood flow to the heart muscle.
- Heart Failure: Certain beta-blockers can improve the function of the heart over the long term in patients with chronic heart failure.
- Post-Myocardial Infarction (Heart Attack): They are vital in secondary prevention, reducing the risk of future heart attacks and improving survival rates after a heart attack.
- Arrhythmias: Beta-blockers help to control irregular heart rhythms by slowing down electrical conduction in the heart.
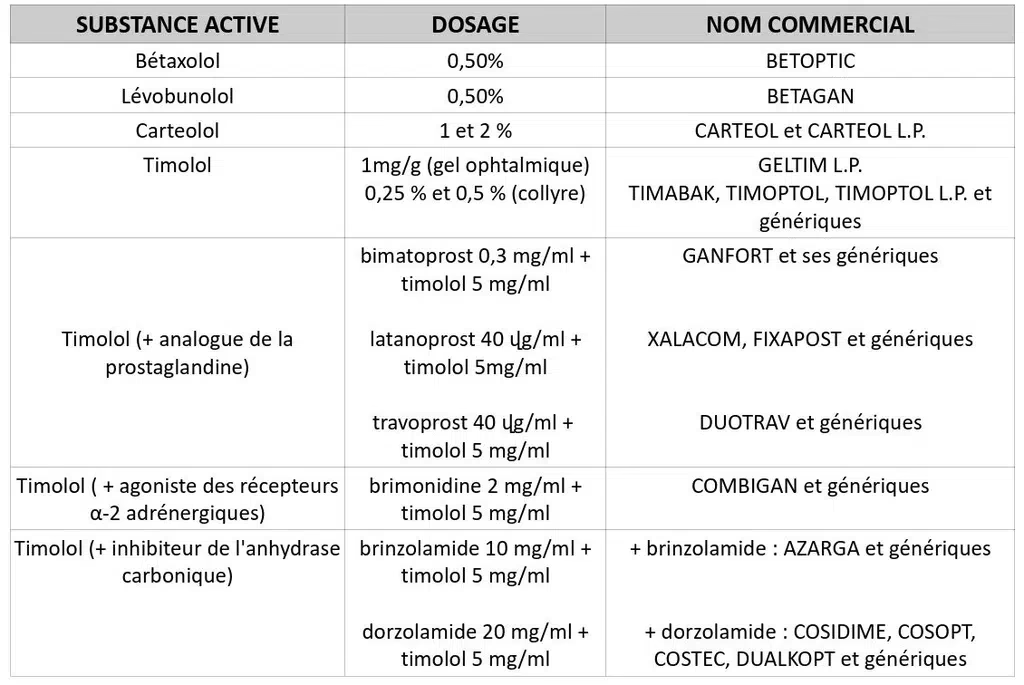
- Glaucoma: When administered as eye drops, they reduce the production of fluid within the eye, lowering intraocular pressure.
- Migraine Prevention: They can reduce the frequency and severity of migraine headaches.
- Essential Tremors: Beta-blockers are effective in reducing the involuntary shaking associated with essential tremor.
- Anxiety and Stress: They can help manage the physical symptoms of anxiety, such as rapid heart rate, palpitations, and trembling.
- Hyperthyroidism: They can control cardiovascular symptoms like rapid heart rate and palpitations associated with an overactive thyroid gland.
How Do Beta-Blockers Work?
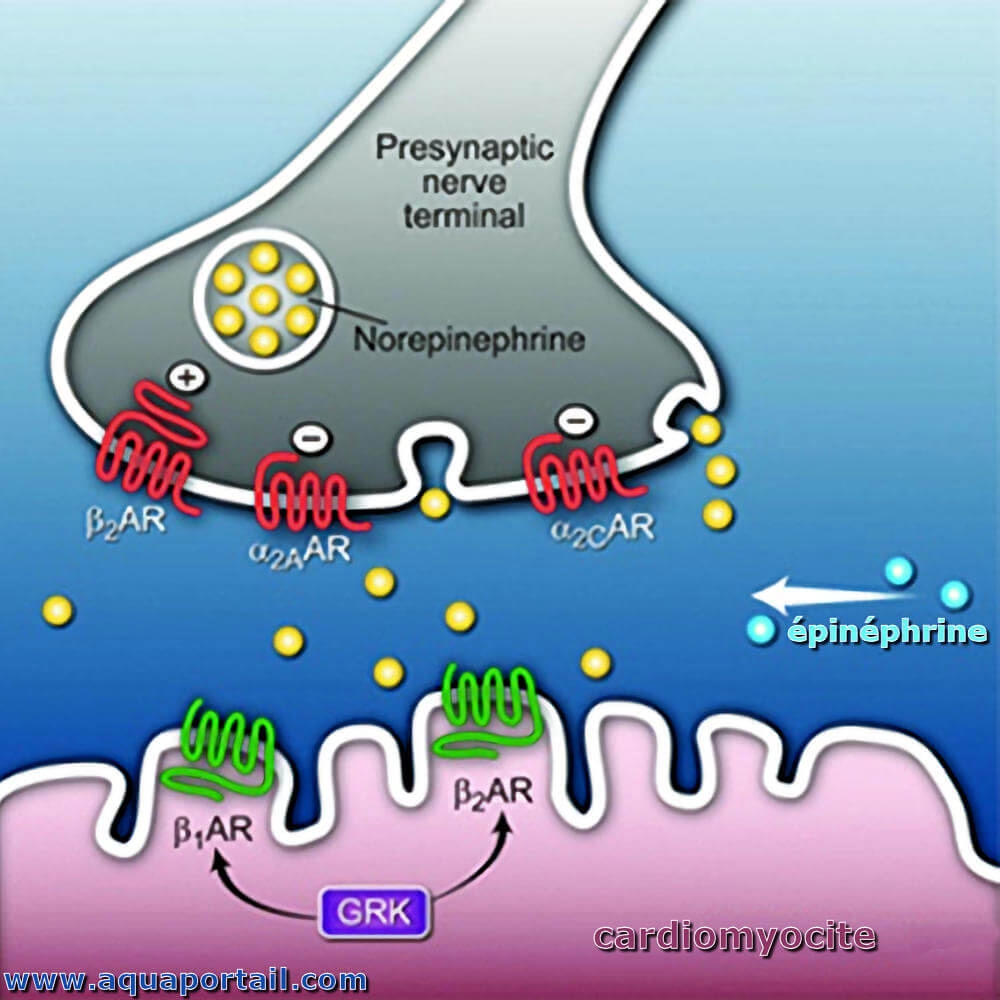
Beta-blockers exert their effects by selectively or non-selectively blocking beta-adrenergic receptors. There are two main types of beta receptors:
- Beta-1 (β1) receptors: Primarily found in the heart. Blocking these receptors slows the heart rate and reduces the force of contraction.
- Beta-2 (β2) receptors: Found in the lungs, blood vessels, and other tissues. Blocking these can lead to bronchoconstriction (narrowing of the airways) and affect blood vessel dilation.
Beta-blockers can be classified based on their selectivity:
Cardioselective (Beta-1 Selective) Beta-Blockers
These primarily target β1 receptors in the heart. They are generally preferred for patients with respiratory conditions like asthma or COPD because they have a lower risk of causing bronchospasm. Examples include:
- Metoprolol (e.g., Seloken®)
- Bisoprolol (e.g., Cardensiel®)
- Atenolol (e.g., Tenormin®)
- Nebivolol (e.g., Nebilox®)
Non-Cardioselective (Non-Selective) Beta-Blockers
These block both β1 and β2 receptors. While effective for many cardiovascular conditions, they carry a higher risk of side effects, particularly in patients with respiratory issues. Examples include:
- Propranolol (e.g., Avlocardyl®)
- Nadolol (e.g., Corgard®)
- Timolol (e.g., Timacor®)
Beta-Blockers with Additional Properties
Some beta-blockers have additional actions that can be beneficial:
- Intrinsic Sympathomimetic Activity (ISA): Medications like Acebutolol (Sectral®) and Pindolol (Visken®) have a mild stimulating effect on beta receptors, which may result in less bradycardia.
- Alpha- and Beta-Blocking Activity: Carvedilol (Kredex®) and Labetalol (Trandate®) block both alpha and beta receptors, leading to vasodilation and further blood pressure reduction.
- Membrane Stabilising Activity: Sotalol (Sotalex®) also has antiarrhythmic properties.
Potential Side Effects of Beta-Blockers
While highly effective, beta-blockers can cause side effects. The likelihood and severity of these effects often depend on the specific drug, dosage, and individual patient factors. It's crucial to report any persistent or bothersome side effects to your doctor.
Common Side Effects:
- Bradycardia: A slow heart rate, which can manifest as dizziness, fatigue, or fainting.
- Hypotension: Low blood pressure, also leading to dizziness or lightheadedness.
- Fatigue and Weakness: A general feeling of tiredness.
- Cold Extremities: Cold hands and feet due to reduced blood flow.
- Dizziness or Lightheadedness: Often related to blood pressure changes.
- Gastrointestinal Issues: Nausea, vomiting, or diarrhoea.
- Sleep Disturbances: Insomnia or nightmares.
Less Common but More Serious Side Effects:
- Bronchospasm: Particularly with non-selective beta-blockers in individuals with asthma or COPD.
- Masking of Hypoglycemia: Beta-blockers can hide the warning signs of low blood sugar (like rapid heart rate) in diabetic patients.
- Depression: Some individuals may experience mood changes or depression.
- Sexual Dysfunction: Erectile dysfunction in men can occur.
- Heart Failure Exacerbation: In rare cases, they can worsen heart failure if not managed correctly.
- Raynaud's Phenomenon: Aggravation of poor circulation in the extremities.
Drug Interactions: What to Watch Out For
Beta-blockers can interact with other medications, potentially altering their effectiveness or increasing the risk of side effects. It is vital to inform your doctor and pharmacist about all medications, supplements, and herbal remedies you are taking.
Key Interactions to Consider:
Pharmacokinetic Interactions (Affecting Drug Metabolism):
Many beta-blockers are metabolised by liver enzymes, particularly CYP2D6 and CYP3A4. Medications that inhibit or induce these enzymes can affect beta-blocker levels:
- CYP2D6 Inhibitors (e.g., Paroxetine, Fluoxetine, Quinidine): Can increase beta-blocker levels, potentially leading to enhanced effects or side effects.
- CYP2D6 Inducers (e.g., Rifampicin, Carbamazepine, Phenytoin): Can decrease beta-blocker levels, reducing their effectiveness.
- CYP3A4 Inhibitors (e.g., Certain Antifungals, Grapefruit Juice): Can increase beta-blocker levels.
- CYP3A4 Inducers (e.g., St. John's Wort): Can decrease beta-blocker levels.
These interactions are not usually contraindications but require careful monitoring and potential dosage adjustments when starting, stopping, or changing doses of interacting medications.
Pharmacodynamic Interactions (Affecting Drug Action):
- Other Blood Pressure-Lowering Medications: Combining beta-blockers with other antihypertensives (e.g., calcium channel blockers, diuretics, ACE inhibitors) can increase the risk of hypotension.
- Calcium Channel Blockers (e.g., Verapamil, Diltiazem): Can potentiate the effects on heart rate and conduction, increasing the risk of bradycardia and heart block.
- Antiarrhythmics: Certain antiarrhythmic drugs can increase the risk of bradycardia and conduction disturbances.
- Digoxin: May increase the risk of bradycardia.
- Insulin and Oral Hypoglycemics: Beta-blockers can mask the symptoms of hypoglycemia in diabetic patients.
- MAO Inhibitors: Can lead to a hypertensive crisis.
- NSAIDs (Non-Steroidal Anti-Inflammatory Drugs): May reduce the blood pressure-lowering effect of beta-blockers.
Special Populations
Pregnancy and Breastfeeding:
The use of beta-blockers during pregnancy and breastfeeding requires careful consideration. Certain beta-blockers, like Labetalol and Propranolol, are often preferred. Close monitoring of both the mother and the baby is essential.
| Indication | Preferred Beta-Blockers |
|---|---|
| Cardiology (Hypertension, Arrhythmia, Angina, Heart Failure) | Pregnancy: Labetalol (1st line), Metoprolol, Atenolol, Propranolol (2nd line). Breastfeeding: Propranolol, Labetalol. |
| Migraine Prevention | Pregnancy/Breastfeeding: Metoprolol, Propranolol. |
| Glaucoma | Pregnancy/Breastfeeding: Timolol (gel/LP formulations preferred to minimise systemic absorption). |
Elderly Patients:
Elderly individuals may be more sensitive to the effects of beta-blockers and often require lower starting doses, with slower titration to avoid side effects like dizziness and bradycardia. Close monitoring of heart rate and blood pressure is crucial.
Patients with Renal or Hepatic Impairment:
Dosage adjustments may be necessary for patients with kidney or liver disease, as these organs are involved in the elimination of many beta-blockers. Your doctor will determine the appropriate dose based on your individual condition.
When to Seek Medical Advice for Side Effects
While some side effects are mild, others warrant prompt medical attention:
- Severe Dizziness or Fainting: Especially if it leads to falls or persists.
- Significantly Slow Heart Rate: Below 40 beats per minute, or accompanied by symptoms like extreme fatigue or lightheadedness.
- Unexplained Fatigue: If it significantly impacts daily activities for over two weeks.
- Shortness of Breath or Chest Pain: These could indicate serious cardiac or pulmonary issues.
- Worsening Asthma Symptoms: Increased wheezing or difficulty breathing.
- Significant Coldness in Hands or Feet: Particularly if accompanied by pain or colour changes.
- Persistent Digestive Upset or Signs of Depression: Nausea, vomiting, or low mood that doesn't resolve.
Important Considerations and Precautions
Taking Your Medication:
Beta-blockers should be taken daily at the same time each day, with or without food, as prescribed by your doctor. Never stop taking beta-blockers abruptly without consulting your doctor, as this can lead to dangerous rebound effects, such as a sudden increase in heart rate or blood pressure.

Choosing the Right Beta-Blocker:
There isn't a single 'best' beta-blocker; the most suitable choice depends on the specific medical condition, the patient's overall health, presence of other conditions (like asthma or diabetes), and potential drug interactions. Your doctor will make this decision based on your individual profile. Common choices include Metoprolol, Bisoprolol, Carvedilol, Nebivolol, and Propranolol, each with its own characteristics.
Who Prescribes Beta-Blockers?
Beta-blockers are prescribed by various specialists, including:
- Cardiologists: For heart-related conditions.
- General Practitioners (GPs): For common issues like hypertension.
- Neurologists: For migraines and tremors.
- Endocrinologists: For hyperthyroidism symptoms.
- Ophthalmologists: For glaucoma (as eye drops).
A thorough medical evaluation is always necessary before starting beta-blocker therapy.
Economic Impact
In France, the expenditure on beta-blockers for health insurance was estimated at €221.3 million in 2022. This figure represents a decrease from previous years, partly due to the increased use of alternative antihypertensive medications and the expiry of patents on many original 'princeps' drugs, allowing for lower-cost generic versions.
In summary, beta-blockers are a cornerstone in the management of numerous cardiovascular and other health conditions. Understanding their mechanism, indications, potential side effects, and interactions is key to their safe and effective use. Always consult with your healthcare provider for personalised advice and treatment plans.
If you want to read more articles similar to Understanding Beta-Blockers: Uses and Side Effects, you can visit the Automotive category.
