10/10/2013
Pregnancy brings about a myriad of changes within a woman's body, and while many are celebrated, others can be quite challenging. Among these, headaches are a surprisingly common occurrence. Approximately 15% of women report experiencing more intense headaches during their pregnancy, with these often being more prevalent in the early stages and tending to subside during the final six months. While the vast majority are harmless and a normal part of the physiological adjustments your body is making, understanding their causes, how to manage them, and crucially, when to seek medical advice, is paramount for your well-being and that of your baby.
It's natural to feel concerned when any new symptom arises during pregnancy, and headaches are no exception. This comprehensive guide aims to equip you with the knowledge to confidently navigate these aches, providing practical tips for prevention and relief, alongside vital information on when a headache might signal something more serious.
Understanding Pregnancy Headaches: Common Types You Might Encounter
Headaches during pregnancy can manifest in various forms, each with its own characteristics and typical triggers. Recognising the type of headache you are experiencing can help in managing it effectively and determining if further medical attention is required.
Tension Headaches
By far the most common type, accounting for roughly 26% of pregnancy headaches, tension headaches are often described as a dull, constant ache or pressure around the head, feeling like a tight band. They are typically mild to moderate in intensity and rarely debilitating. These headaches are frequently linked to daily stresses and fatigue, which are, let's be honest, often heightened during pregnancy.
Migraines
While some women experience migraines for the first time during pregnancy, it's more common for those who already suffer from them to continue doing so. Interestingly, about 70% of women with pre-existing migraines actually find their symptoms improve significantly during pregnancy, especially in the later trimesters. However, for others, they might persist or even worsen. Migraines are characterised by more intense, throbbing pain, often on one side of the head. They can be accompanied by nausea, vomiting, and heightened sensitivity to light (photophobia) and sound (phonophobia). In some cases, migraines may include an 'aura', which can involve visual disturbances like flashing lights or zigzag lines, or even tingling sensations in the arms and legs. Migraine attacks typically last for at least 24 hours.

Why Do They Happen? Unpacking the Causes
The pregnant body undergoes incredible transformations, and these changes are often at the root of headache development. Understanding the underlying causes can help you identify and avoid triggers.
- Hormonal Changes: The significant fluctuations in hormones, particularly oestrogen and progesterone, especially in the first trimester, are a primary culprit. These hormonal shifts can directly influence blood vessels and nerve pathways, leading to headaches.
- Increased Blood Circulation: Your body is working hard to support two lives, meaning an increase in blood volume and circulation. This physiological change can sometimes lead to an increase in pressure within the blood vessels in your head, contributing to headaches.
- Nasal Congestion: Pregnancy rhinitis, or a stuffy nose, is common due to increased blood flow to mucous membranes. This congestion can lead to sinus pressure, which often translates into frontal headaches.
- Stress and Fatigue: The physical demands of pregnancy, coupled with the emotional rollercoaster and often disrupted sleep, can lead to increased stress and profound fatigue. Both are well-known triggers for tension headaches.
- Hunger and Low Blood Sugar: Missing meals or going too long without food can cause your blood sugar levels to drop, leading to a headache. This is particularly relevant during pregnancy when your body's energy demands are higher.
- Dehydration: Especially if you are experiencing morning sickness with nausea and vomiting, dehydration can quickly set in. Even mild dehydration can trigger headaches.
- Caffeine Withdrawal: If you're used to a daily dose of caffeine and suddenly cut back or stop completely, withdrawal symptoms, including headaches, can occur.
Proactive Steps: Preventing Pregnancy Headaches
While not all headaches can be avoided, many can be prevented or their severity reduced through simple lifestyle adjustments. Prevention is always better than cure, especially when considering medication during pregnancy.
- Stay Hydrated: Drink plenty of water throughout the day. Keep a water bottle handy and sip regularly, especially if you're experiencing morning sickness.
- Prioritise Rest: Ensure you get an adequate number of hours of sleep each night. Listen to your body and allow yourself periods of rest during the day, even if it's just a short nap or lying down quietly.
- Manage Stress: Pregnancy can be stressful, but finding healthy ways to cope is crucial. Avoid overly stressful situations and try not to overload yourself with work or commitments. Practise relaxation techniques such as deep breathing exercises, gentle yoga, or calming massages.
- Identify and Avoid Triggers: Pay attention to what might be setting off your headaches. Common triggers can include coffee, tea, chocolate, stress, or bright lights. Certain foods are also known to trigger migraines in sensitive individuals, such as strong cheeses, cured meats, and those containing monosodium glutamate (MSG). Keeping a headache diary can help you pinpoint your personal triggers.
- Maintain Stable Blood Sugar: Eat balanced meals in smaller portions and incorporate healthy snacks throughout the day. This helps keep your blood sugar levels steady and prevents hunger-induced headaches.
- Gentle Physical Activity: Regular, moderate exercise, as advised by your healthcare provider, can improve circulation, reduce stress, and promote better sleep, all of which contribute to headache prevention.
Easing the Ache: Relief Strategies
When a headache strikes, there are several non-pharmacological and safe medication options to help alleviate the pain. Always prioritise non-drug methods first.
Non-Pharmacological Approaches
- Rest in a Conducive Environment: Retreat to a dark, quiet, and cool room. Lie down and close your eyes.
- Apply Compresses: Place warm or cool compresses on your forehead or the back of your neck. Experiment to see which provides more relief for you. A warm bath (ensure it's not too hot) can also be soothing.
- Scalp Massage: Gently massaging your scalp can help improve blood flow and relieve tension, offering a measure of relief.
Medication Guidance
When non-drug methods aren't enough, some medications are considered safe for use during pregnancy, while others should be strictly avoided.
- Paracetamol: This is generally considered the safest over-the-counter painkiller during pregnancy (e.g., Panadol, Calpol in the UK). Always adhere to the recommended dosage.
- Ibuprofen: It is crucial to avoid Ibuprofen (e.g., Advil, Nurofen in the UK) and other non-steroidal anti-inflammatory drugs (NSAIDs) during pregnancy. Their use has been associated with complications such as miscarriage and heart problems in the baby. It's important to note that Ibuprofen is generally considered safe during breastfeeding, but this is post-pregnancy.
- Other Medications: If you were prescribed medications for migraines before your pregnancy, or if you are considering any other headache relief medication, it is essential to speak to your pharmacist or healthcare provider first. They can advise on the safety and appropriateness of the medication during your pregnancy. Never self-medicate with unverified drugs.
When to Seek Medical Advice: Red Flags You Must Know
While most pregnancy headaches are benign, some can be a sign of a more serious underlying condition. It is vital to be aware of the warning signs and to contact your doctor or midwife immediately if you experience any of the following symptoms, especially if they appear after 20 weeks of pregnancy:
- Severe or Persistent Headaches: Headaches that are unusually severe, sudden in onset, or last for more than three days warrant immediate medical attention.
- Fever: A headache accompanied by a fever could indicate an infection.
- Stomach Pain or Pain Below the Ribs: This, especially when combined with a headache, can be a symptom of pre-eclampsia.
- Blurred Vision: Any changes in vision, such as blurriness, double vision, or seeing spots or flashing lights, are serious signs.
- Vomiting: Persistent or severe vomiting, particularly if it accompanies a severe headache and is not related to typical morning sickness.
- Sudden Swelling: Noticeable and sudden swelling of your face, hands, feet, or ankles can be a key indicator of pre-eclampsia.
- Drowsiness or General Deterioration: If you feel unusually sleepy, confused, or your general condition worsens.
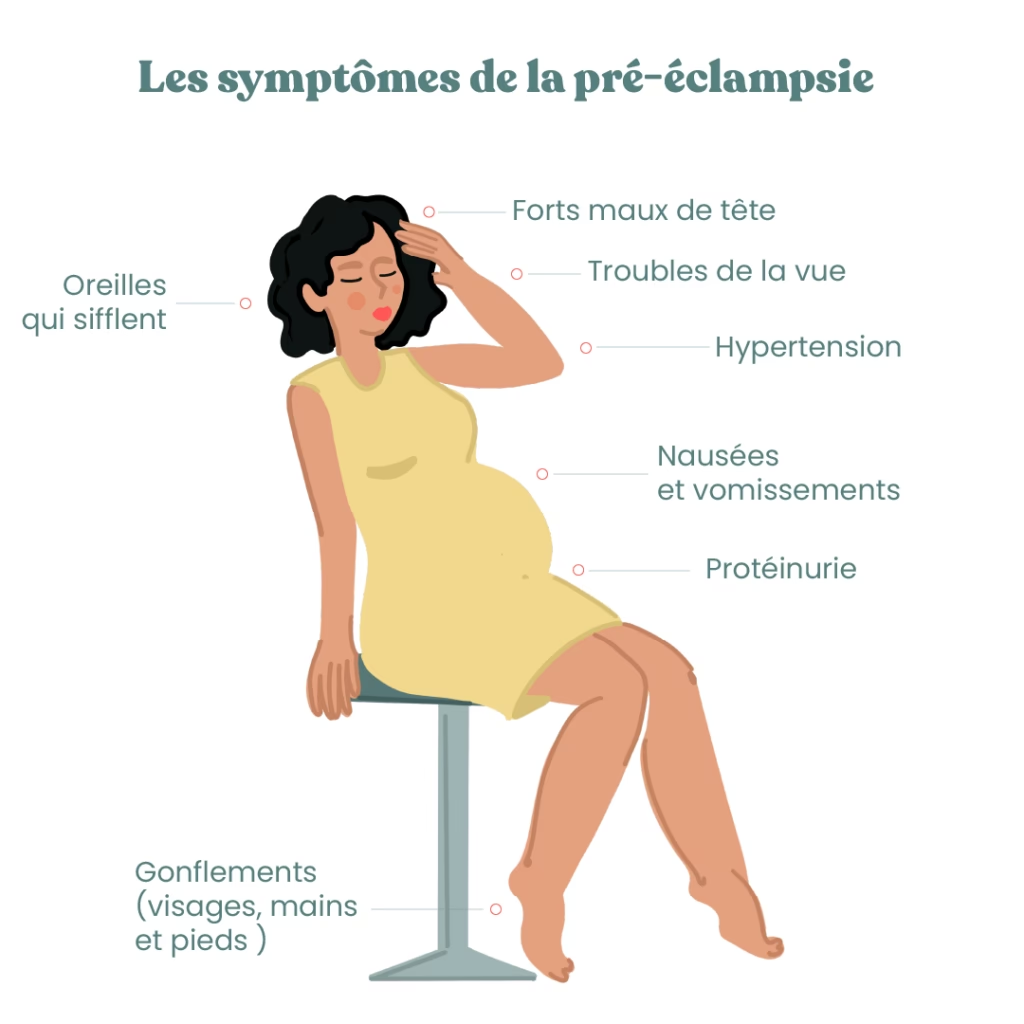
These symptoms, particularly after 20 weeks of gestation, could be indicative of pre-eclampsia. This is a serious pregnancy complication characterised by high blood pressure and protein in the urine, posing risks to both the mother and the baby. Other rare but serious neurological conditions like stroke, cerebral haemorrhage, or cerebral venous thrombosis can also present with severe headaches, sometimes accompanied by seizures or muscle weakness. Always err on the side of caution and seek prompt medical evaluation if you have any concerns.

Comparison Table: Headache Types & Key Characteristics
| Headache Type | Common Timing | Symptoms | Common Causes | When to Worry |
|---|---|---|---|---|
| Tension Headache | First Trimester, throughout | Mild-moderate, dull, band-like ache, pressure | Stress, fatigue, nasal congestion, dehydration | Rarely concerning on its own; if persistent/worsening |
| Migraine | Variable (often improve if pre-existing) | Severe, pulsating, unilateral, nausea, light/sound sensitivity, aura | Hormones, specific triggers, pre-existing condition | If new onset, significantly worse/different, or accompanied by red flags |
| Pre-eclampsia Related | Typically after 20 weeks | Severe, persistent, often with blurred vision, sudden swelling, stomach pain | High blood pressure, protein in urine (medical condition) | URGENT MEDICAL ATTENTION REQUIRED |
Frequently Asked Questions (FAQs)
Q: Why are headaches so common in early pregnancy?
A: Headaches are particularly common in the first trimester due to the rapid and significant hormonal changes your body undergoes. Increased blood volume, fatigue, and dehydration (often exacerbated by morning sickness) are also major contributors during this initial period of adjustment.
Q: Do all headaches during pregnancy mean something serious?
A: No, thankfully, the vast majority of headaches experienced during pregnancy are benign and are simply a normal part of your body adapting. However, it is crucial to be aware of the warning signs, such as severe pain, blurred vision, or sudden swelling, which warrant immediate medical review to rule out more serious conditions like pre-eclampsia.
Q: Can I take any painkillers for pregnancy headaches?
A: Paracetamol is generally considered the safest over-the-counter painkiller to take during pregnancy, when used according to dosage instructions. However, you should avoid Ibuprofen and other NSAIDs. Always consult your doctor or pharmacist before taking any medication, even those you used before pregnancy, to ensure it's safe for you and your baby.
Q: Will my migraines get worse during pregnancy?
A: Interestingly, for many women who suffer from migraines prior to pregnancy, their condition often improves. Approximately 70% of migraine sufferers experience a reduction in the frequency and intensity of their attacks during pregnancy. However, for a smaller percentage, migraines may worsen or appear for the first time.
Key Takeaways
- Headaches are a common symptom during pregnancy, particularly in the first trimester, and often decrease in severity later on.
- Most pregnancy headaches are benign tension headaches, but some women may experience migraines.
- Common causes include hormonal changes, increased blood flow, stress, fatigue, dehydration, and caffeine withdrawal.
- Lifestyle adjustments like staying hydrated, getting enough rest, managing stress, and identifying triggers can help prevent headaches.
- Paracetamol is generally safe for pain relief, but Ibuprofen should be strictly avoided. Always consult your healthcare provider before taking any medication.
- Seek urgent medical attention if you experience severe, persistent headaches, especially after 20 weeks, or if they are accompanied by symptoms like blurred vision, sudden swelling, stomach pain, or fever, as these could indicate serious conditions like pre-eclampsia.
If you want to read more articles similar to Navigating Headaches During Pregnancy: A UK Guide, you can visit the Automotive category.
