21/12/2018
Ocular hypertension, a condition characterised by elevated pressure within the eye, is a topic of significant interest for maintaining optimal vision. While often asymptomatic in its early stages, understanding its potential to progress to more severe conditions like glaucoma is crucial. This article delves into the intricacies of ocular hypertension, exploring its definition, the subtle ways it can manifest, and the critical importance of regular eye examinations in safeguarding your sight.
Understanding Ocular Hypertension
Ocular hypertension is medically defined as an increase in intraocular pressure (IOP) above the normal range, which is typically between 11 and 21 millimeters of mercury (mmHg). This pressure is maintained by a delicate balance between the production and drainage of aqueous humour, a clear fluid that nourishes the front of the eye. When the drainage system of the eye becomes inefficient, fluid can accumulate, leading to a rise in IOP. This elevated pressure, if sustained, can potentially exert damaging effects on the optic nerve, the vital conduit of visual information from the eye to the brain.
The Subtle Onset: Symptoms and Detection
One of the most concerning aspects of ocular hypertension is its often silent nature. Many individuals with this condition experience no noticeable symptoms, making it a stealthy precursor to more serious eye diseases. Unlike acute conditions, there are typically no immediate visual disturbances. This lack of early warning signs underscores the paramount importance of routine eye check-ups. An eye care specialist can accurately measure IOP during a comprehensive eye examination. A diagnosis of ocular hypertension is generally made when IOP consistently measures above 21 mmHg in one or both eyes over multiple visits. It's important to distinguish between bilateral ocular hypertension (affecting both eyes) and unilateral ocular hypertension (affecting only one eye), as management strategies may vary.
Ocular Hypertension vs. Glaucoma: A Critical Distinction
The relationship between ocular hypertension and glaucoma is a key area of concern. Ocular hypertension is considered a significant risk factor for developing glaucoma. Glaucoma is a group of eye diseases that cause progressive damage to the optic nerve, often associated with elevated IOP. While ocular hypertension means the pressure is high, glaucoma signifies that this high pressure has already begun to harm the optic nerve. Without timely intervention, untreated glaucoma can lead to irreversible vision loss, including blindness. Therefore, managing ocular hypertension is a proactive measure to prevent the onset or progression of glaucoma.

Risk Factors: Who is Most Vulnerable?
Several factors can increase an individual's susceptibility to ocular hypertension and, consequently, glaucoma. Some of these risk factors are unchangeable, such as:
| Risk Factor | Description |
|---|---|
| Age | The risk of ocular hypertension generally increases with age. |
| Ethnicity | Certain ethnic groups, such as individuals of African or Asian descent, may have a higher predisposition. |
| Family History | A personal or family history of glaucoma significantly elevates the risk. |
Additionally, specific medical conditions can contribute to ocular hypertension:
- Pigment Dispersion Syndrome: In this condition, pigment granules from the iris (the coloured part of the eye) can flake off and clog the eye's drainage channels, leading to increased IOP.
- Pseudoexfoliation Syndrome: This is a condition where flaky deposits of protein build up in various parts of the eye, including the drainage system, impeding fluid outflow.
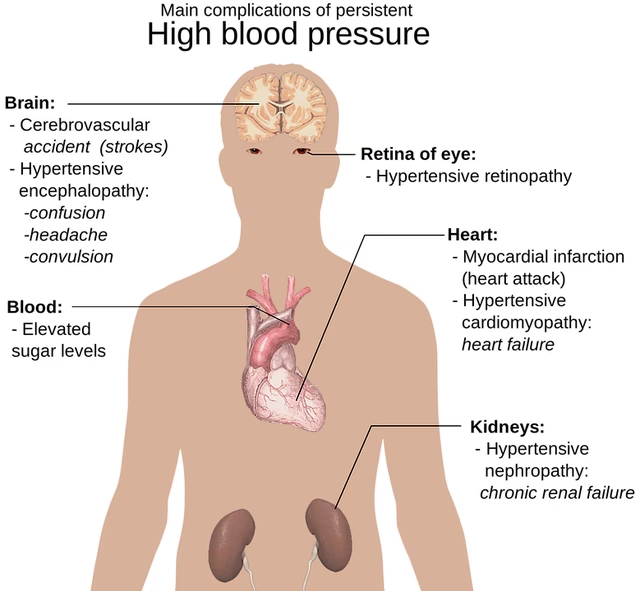
Other identifiable risk factors include a history of eye injury, long-term use of corticosteroid medications (especially eye drops), and certain systemic health conditions like diabetes and high blood pressure. High blood pressure itself can have a profound impact on eye health. The intricate network of tiny blood vessels within the eye is particularly sensitive to sustained high blood pressure. Over time, this can lead to damage to these delicate structures, potentially affecting vision. While the link between high blood pressure and blurred vision is well-documented, it's crucial to understand that elevated blood pressure can also indirectly contribute to ocular hypertension by affecting the overall health of the eye's vascular system.
The Importance of Early Detection and Management
Given the largely asymptomatic nature of ocular hypertension, early detection through regular comprehensive eye examinations is paramount. These examinations typically include:
- Tonometry: This is the standard test used to measure intraocular pressure. Various methods exist, such as the Goldmann applanation tonometry or non-contact tonometry (air puff test).
- Ophthalmoscopy: This allows the eye doctor to examine the optic nerve for any signs of damage or changes.
- Perimetry (Visual Field Testing): This test maps out the entire visual field of each eye, helping to detect any blind spots that might indicate optic nerve damage.
If ocular hypertension is diagnosed, your eye care professional will develop a personalised management plan. This plan may involve:
- Regular Monitoring: More frequent eye examinations to closely track IOP and monitor the optic nerve for any changes.
- Medicated Eye Drops: Prescription eye drops are often the first line of treatment to lower IOP by reducing fluid production or increasing fluid drainage. It is vital to use these drops exactly as prescribed.
- Laser Therapy: In some cases, laser treatment may be recommended to improve the drainage of aqueous humour.
- Surgery: Surgical procedures are typically reserved for cases where medication and laser therapy are insufficient to control IOP.
Frequently Asked Questions
Q1: Can ocular hypertension cause permanent vision loss?
While ocular hypertension itself, if unmanaged, can lead to glaucoma and subsequent vision loss, the condition as a precursor does not always result in permanent damage if detected and treated early. The damage occurs when glaucoma develops and progresses.
Q2: How often should I have my eyes checked if I have ocular hypertension?
The frequency of follow-up appointments will be determined by your eye care specialist based on your individual risk factors and the stability of your IOP. It could range from every few months to annually.

Q3: Are there lifestyle changes that can help with ocular hypertension?
While not a direct treatment, maintaining a healthy lifestyle, including a balanced diet, regular exercise, and managing conditions like high blood pressure and diabetes, can contribute to overall eye health and may indirectly support IOP management. Avoiding smoking is also beneficial.
Q4: Can high blood pressure directly cause blurred vision?
Yes, high blood pressure can cause blurred vision. The elevated pressure can affect the blood vessels in the retina, leading to swelling or bleeding, which can distort vision. Vision problems can sometimes be the first noticeable sign of uncontrolled high blood pressure.
In conclusion, ocular hypertension represents a critical juncture in eye health. By understanding its nature, recognising the risk factors, and committing to regular eye examinations, individuals can take proactive steps to protect their vision from the potentially devastating consequences of untreated high intraocular pressure.
If you want to read more articles similar to Ocular Hypertension: A Silent Threat to Your Vision, you can visit the Automotive category.
