08/10/2024
The human mouth is a complex ecosystem, teeming with a diverse array of microorganisms. While many of these bacteria are commensal, playing a neutral or even beneficial role, others can pose a significant threat to our health. Among these potentially pathogenic bacteria, Staphylococcus aureus has long been recognised for its ability to cause a wide range of infections, from superficial skin ailments to life-threatening systemic conditions. However, its presence and role within the oral cavity and the surrounding perioral region have been a subject of ongoing debate and investigation. This article delves into a comprehensive 10-year retrospective analysis of laboratory data, exploring the frequency of S. aureus isolation from oral and perioral clinical specimens, shedding light on its potential implications for both oral health and broader cross-infection pathways.
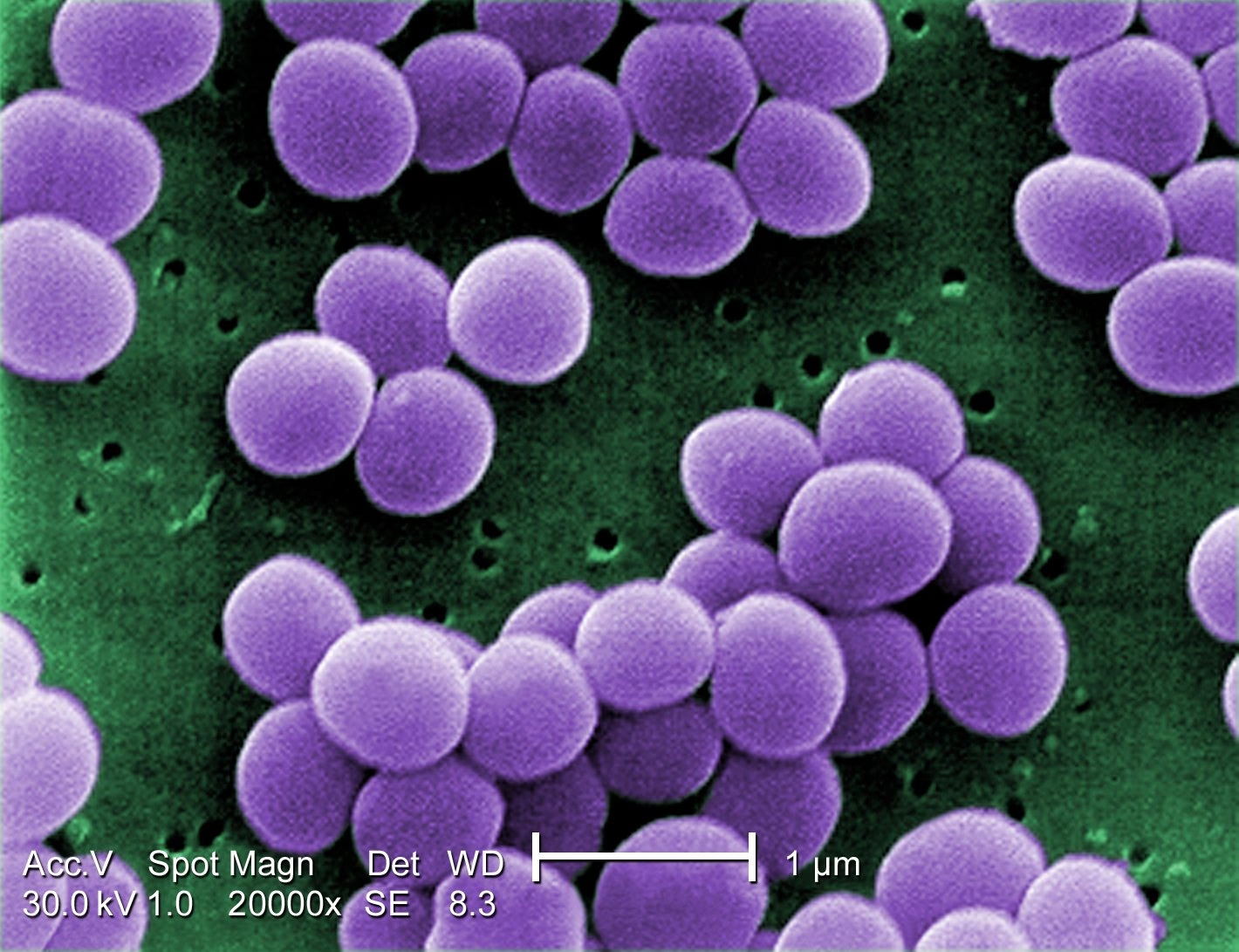
For years, the scientific community has pondered the significance of Staphylococcus aureus residing within the mouth. Is it merely a bystander, or does it actively contribute to disease processes? Furthermore, could the oral cavity serve as a reservoir for transmitting this formidable bacterium to other parts of the body, or even to other individuals? These questions are crucial for understanding the full spectrum of S. aureus infections and for developing effective strategies for prevention and treatment. This study, conducted at the Oral Microbiology Laboratory of Glasgow Dental Hospital, aimed to provide empirical data to address these very uncertainties.
- The Scope of the Study: A Decade of Data
- Key Findings: A Significant Presence
- Specimen Types: Where is it Found Most?
- The Dominance of Specific MRSA Lineages
- Implications for Oral Health and Beyond
- Understanding the Mechanisms: Colonization and Virulence
- Diagnostic Considerations and Clinical Practice
- Future Research Directions
- Conclusion: A Re-evaluation of the Oral Microbiome
The Scope of the Study: A Decade of Data
The research encompassed a substantial period, reviewing laboratory records from January 1998 to December 2007. During these ten years, a total of 11,312 specimens were submitted for microbiological analysis. These specimens originated from various oral and perioral sites, reflecting a broad spectrum of clinical presentations and patient demographics. The meticulous collation and analysis of this extensive dataset were key to drawing robust conclusions about the prevalence of S. aureus in this specific anatomical niche.
Key Findings: A Significant Presence
The results of the analysis were quite striking. Staphylococcus aureus was identified in a significant proportion of the submitted specimens – specifically, in 1,986 cases, which translates to an impressive 18% of the total. This figure immediately suggests that S. aureus is far from an infrequent visitor to the oral environment. The sheer volume of isolation underscores the importance of considering this bacterium when evaluating oral health concerns.
Delving deeper into the types of S. aureus identified, the study revealed a clear distinction between methicillin-sensitive S. aureus (MSSA) and methicillin-resistant S. aureus (MRSA). Of the 1,986 isolates, a vast majority, 1,782 (90%), were MSSA. This is the more common form of the bacteria, generally more susceptible to a wider range of antibiotics. However, the remaining 204 isolates (10%) were MRSA. The emergence and persistence of MRSA are of particular concern due to its inherent resistance to many commonly used antibiotics, making infections more challenging to treat.
Specimen Types: Where is it Found Most?
The study also provided valuable insights into the specific sites within the oral cavity and perioral region where S. aureus was most frequently detected. For MSSA, the most common specimen type yielding positive results was the oral rinse. This suggests that MSSA can be present in the general oral environment, potentially residing in saliva or on mucosal surfaces throughout the mouth. Oral rinses are often used to sample a broad area, indicating a widespread presence.
In contrast, for MRSA, the tongue swab emerged as the most frequent source of isolation. This finding is particularly noteworthy. The tongue, with its textured surface, can harbour bacteria and may represent a more specific niche for MRSA colonization. The fact that MRSA was more concentrated on tongue swabs, compared to the more general oral rinse for MSSA, could imply different colonization patterns or preferences between the two strains.
The Dominance of Specific MRSA Lineages
Further analysis of the MRSA isolates revealed that the majority belonged to specific lineages: EMRSA-15 or EMRSA-16. These designations refer to particular strains of MRSA that have been identified and tracked due to their prevalence and potential for community and hospital-acquired infections. The identification of these specific lineages in oral specimens highlights the potential for the oral cavity to be a reservoir for strains that are already known to be problematic in other healthcare settings. This has significant implications for understanding the transmission dynamics of MRSA.
Implications for Oral Health and Beyond
The conclusions drawn from this extensive study are significant and far-reaching. Firstly, the findings strongly suggest that Staphylococcus aureus remains a frequent isolate within the oral cavity and the surrounding perioral tissues. This challenges any notion that the oral environment is merely a passive recipient of this bacterium. Instead, it points towards the oral cavity as an active site for S. aureus colonization and potentially, replication.
Secondly, the study posits that the oral cavity should be considered a potential source of S. aureus in the context of cross-infection. This means that individuals carrying S. aureus in their mouths could inadvertently transmit the bacteria to others through various means, such as respiratory droplets or direct contact. Furthermore, it raises the possibility of the oral cavity acting as a source for autoinfection, where the bacteria spread from the mouth to other parts of the body, leading to infections elsewhere.
The presence of MRSA, in particular, within oral samples is a serious consideration. Given that MRSA is often associated with more severe and difficult-to-treat infections, its identification in the mouth warrants careful attention. It raises questions about whether oral colonization with MRSA could predispose individuals to systemic MRSA infections or contribute to the spread of MRSA within healthcare settings and the community.
Thirdly, the study encourages a re-evaluation of the role of S. aureus in the pathogenesis of certain oral diseases. While often associated with skin and soft tissue infections, the possibility of S. aureus contributing to conditions affecting the mouth itself cannot be overlooked. This could include exacerbating existing oral inflammatory conditions, playing a role in periodontal disease, or contributing to the development of specific oral lesions. Therefore, clinicians should consider S. aureus as part of a differential diagnosis when faced with unusual or persistent oral pathologies.
Understanding the Mechanisms: Colonization and Virulence
The ability of S. aureus to colonize the oral cavity and persist there is likely due to a complex interplay of factors. The oral environment offers a rich source of nutrients and various surfaces for bacterial adhesion. S. aureus possesses a repertoire of adhesins and surface proteins that facilitate its attachment to oral tissues, including epithelial cells and the tongue's surface. Once attached, it can form biofilms, which are communities of bacteria encased in a protective matrix, further enhancing its resilience against host defences and antimicrobial agents.
The virulence factors produced by S. aureus also play a crucial role. These include a variety of toxins, enzymes, and surface proteins that can damage host tissues, evade the immune system, and promote bacterial invasion. For example, coagulase, a key virulence factor, helps the bacteria to evade phagocytosis by immune cells. Toxins like alpha-hemolysin can cause direct damage to host cells, and superantigens can trigger exaggerated immune responses, leading to tissue damage.
The specific preference for tongue swabs observed for MRSA might be related to differences in adhesion mechanisms or the microenvironment of the tongue's surface compared to other oral sites. Further research could explore the specific molecular interactions between MRSA strains and tongue epithelial cells.
Diagnostic Considerations and Clinical Practice
The findings of this study have direct implications for clinical practice. Dentists, oral surgeons, and other healthcare professionals who deal with the oral cavity should be aware of the significant prevalence of S. aureus. This awareness should translate into appropriate diagnostic considerations:
- Differential Diagnosis: When a patient presents with oral lesions, infections, or persistent inflammation, S. aureus should be included in the differential diagnosis, especially if conventional treatments are not proving effective. Microbiological sampling and testing may be warranted.
- Infection Control: For healthcare professionals, understanding the oral cavity as a potential reservoir for S. aureus reinforces the importance of rigorous infection control measures. This includes proper hand hygiene, the use of personal protective equipment, and the disinfection of dental instruments and equipment.
- Patient Screening: In certain high-risk settings, such as intensive care units or during specific surgical procedures, screening patients for S. aureus colonization, including in the oral cavity, might be considered, particularly if they have a history of MRSA infections or are at high risk of developing them.
- Antibiotic Stewardship: The presence of MRSA in oral samples highlights the need for judicious antibiotic use. Prescribing antibiotics for oral conditions should be based on accurate diagnosis and susceptibility testing, avoiding broad-spectrum agents when a more targeted approach is possible.
Future Research Directions
While this study provides a valuable snapshot of S. aureus prevalence, several avenues for future research remain open:
- Longitudinal Studies: More extensive longitudinal studies could track the carriage of S. aureus in individuals over time to understand the dynamics of colonization and potential fluctuations in shedding.
- Mechanistic Studies: Investigating the specific molecular mechanisms by which S. aureus colonizes different oral sites, adheres to tissues, and interacts with the host immune system would provide deeper insights.
- Association with Oral Diseases: Research specifically designed to correlate the presence and load of S. aureus with the incidence and severity of various oral diseases, such as periodontal disease, oral candidiasis, or lichen planus, is needed.
- Treatment Strategies: Exploring novel therapeutic strategies for managing S. aureus colonization in the oral cavity, potentially including antimicrobial mouthwashes or probiotics, could be beneficial.
- Transmission Pathways: Further studies focusing on the specific transmission pathways of oral S. aureus, both within individuals and between individuals, would help in designing targeted public health interventions.
Conclusion: A Re-evaluation of the Oral Microbiome
In conclusion, the decade-long analysis from Glasgow Dental Hospital unequivocally demonstrates that Staphylococcus aureus is a frequently isolated bacterium from the oral cavity and perioral region. The data underscore the importance of viewing the mouth not just as a site for food processing and speech, but as a dynamic microbial environment that can harbour significant pathogens like S. aureus. The identification of MSSA and particularly MRSA, including specific problematic lineages, highlights the potential for the oral cavity to serve as a reservoir for cross-infection and to contribute to the burden of staphylococcal disease. Clinicians should remain vigilant, considering S. aureus in their diagnostic workup for oral conditions and adhering to stringent infection control practices. This research serves as a crucial reminder of the complex interplay between oral health and systemic well-being, urging a continued exploration into the multifaceted roles of microorganisms within our bodies.
If you want to read more articles similar to Staph Aureus in the Mouth: A Hidden Threat?, you can visit the Automotive category.
