25/10/2023
Understanding and Managing Gastro-Oesophageal Reflux Disease (GORD)
Gastro-Oesophageal Reflux Disease, commonly known as GORD or acid reflux, is a condition where stomach acid or contents flow back up into the oesophagus (the gullet connecting the throat to the stomach). This backward flow can occur at any time, day or night, but it's particularly frequent after meals and when lying down. For many, the symptoms can be a persistent nuisance, impacting daily life. These can range from a persistent cough, a sore throat, and the classic burning sensation of heartburn or indigestion, to excessive mucus, post-nasal drip, an unpleasant taste in the mouth, or even a sensation of a lump in the throat. The good news is that with a few targeted changes, relief is often achievable. This guide aims to provide you with the knowledge and practical steps to help neutralise stomach acid, reduce its production, and prevent it from irritating your oesophagus and throat. Remember, healing takes time, so aim for at least four to six weeks of consistent effort to see noticeable improvements.
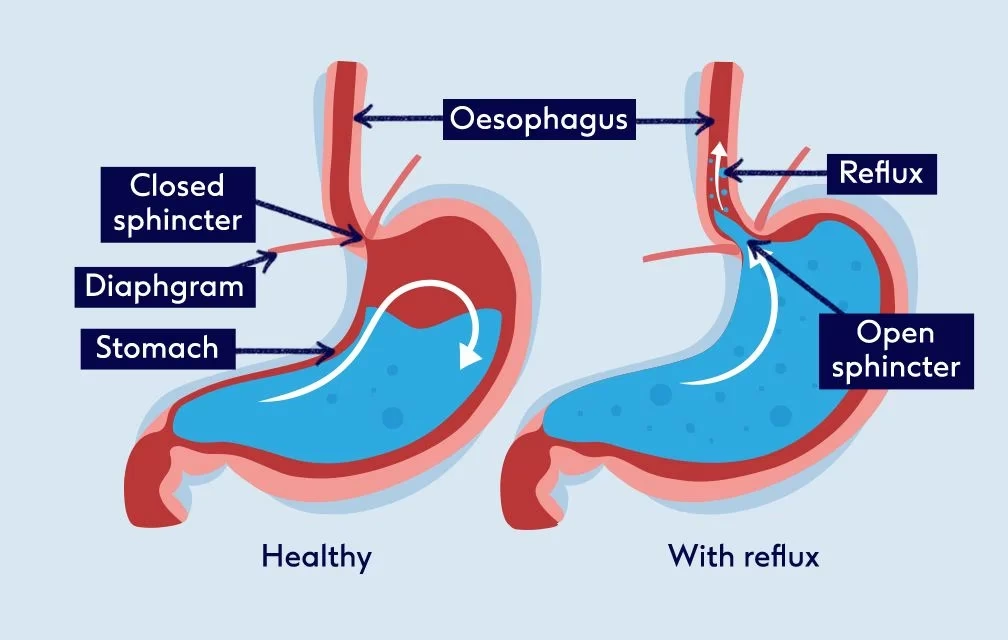
What Triggers Acid Reflux?
The causes of reflux are multifaceted, often stemming from a combination of factors related to our diet, our eating habits, our overall lifestyle, and even certain medications we might be taking. Understanding these triggers is the first step towards effectively managing the condition.
Dietary Adjustments for Reflux Relief
What you eat and drink plays a significant role in managing GORD. Making conscious choices about your food intake can make a substantial difference. Here are some key recommendations:
Eating Habits to Adopt:
- Smaller, More Frequent Meals: Instead of consuming large meals that can overwhelm your stomach, opt for smaller portions spread throughout the day. This aids digestion and reduces the likelihood of reflux.
- Evening Eating Habits: Limit your food intake in the evening. Aim to finish your last meal at least two hours before going to bed to allow your stomach adequate time to digest before you lie down.
- Avoid 'Eating on the Run': Take your time when eating. Rushing meals can lead to gulping air and inadequate chewing, both of which can exacerbate reflux.
- Maintain an Upright Posture: Sit upright while eating. Avoid eating while slumped in a low armchair with a tray on your lap, as this can impede digestion and encourage reflux.
- Stay Upright After Meals: Try to remain upright for at least an hour after eating. Avoid slumping or bending over, which can put pressure on your stomach and push acid upwards.
- Hydration is Key: Drink plenty of water throughout the day. Water helps to dilute stomach acid and aids in flushing food through the digestive system.
Foods to Approach with Caution:
Certain foods are known to irritate the oesophagus or increase stomach acid production. While individual triggers can vary, the following are commonly identified culprits:
| Food/Drink Category | Potential Impact |
|---|---|
| Spicy Foods, Tomato-Based Foods, Onions, Citrus Fruits, Vinegar | Can irritate the oesophagus and increase stomach acidity. |
| Fried, Fatty, or Greasy Foods | Slow down stomach emptying, increasing the chance of reflux. |
| Coffee (Caffeinated and Decaffeinated), Tea | Caffeine can relax the lower oesophageal sphincter (LES), allowing acid to escape. |
| Chocolate | Contains compounds that can relax the LES. |
| Carbonated (Fizzy) Drinks | Can cause bloating and increase pressure in the stomach. |
| Alcohol | Relaxes the LES and can irritate the oesophagus. |
| Very Salty, Crispy, or Crumbly Foods | May exacerbate existing irritation in the oesophagus. |
Lifestyle Modifications for Long-Term Relief
Beyond diet, several lifestyle adjustments can significantly contribute to managing GORD:
- Clothing: Avoid wearing tight clothing around your waist. Constrictive clothing can put pressure on your abdomen, pushing stomach contents upwards.
- Stress Management: Stress can often worsen digestive issues. Explore relaxation techniques such as joining relaxation classes, practicing yoga, or engaging in swimming to help manage stress levels.
- Smoking Cessation: If you smoke, quitting is one of the most impactful changes you can make. Smoking can weaken the LES. For support, consider calling the NHS Smoking Helpline on 0800 0224332.
- Elevate Your Bed: To prevent acid from flowing back when you sleep, raise the head end of your bed by placing blocks of 10 to 25 cm high under the bedposts. Simply using extra pillows is generally not effective as it can cause you to bend at the waist, potentially increasing pressure.
- Weight Management: If you are overweight, losing even a small amount of weight can significantly reduce the pressure on your stomach and lessen reflux symptoms. Consult your GP or a healthcare professional for advice on safe and effective weight loss strategies.
- Sleeping Position: Sleeping on your left side or on your stomach is often recommended. These positions can help gas to escape from the stomach more easily and reduce the likelihood of acid escaping into the oesophagus.
Medications and Acid Reflux
Certain medications can inadvertently contribute to or worsen acid reflux. If you suspect your medication might be a factor, it's crucial to discuss this with your doctor rather than stopping any prescribed treatment.
Medications That May Increase Reflux Risk:
- Some tranquillisers
- Steroids
- Certain asthma medications
- High doses of Vitamin C (1,000mg or more)
- Beta-blockers
- Tablets containing progesterone
- Aspirin
Important Note: Never stop taking prescribed medication without consulting your GP or pharmacist. If you believe your medication is contributing to your reflux symptoms, seek professional advice to explore alternative options or dosage adjustments.
Over-the-Counter Remedies for Symptom Relief
Several over-the-counter (OTC) medications can provide relief from the symptoms of acid reflux. It's important to use these as directed and be aware of potential interactions.
Antacids:
Antacids, such as Rennies, are readily available from your local pharmacist. They work by neutralising existing stomach acid. They can be taken just before bedtime initially, or if symptoms are persistent, 45 minutes after meals and every two hours between meals, as well as at bedtime. Be aware that antacids can interfere with the absorption of certain other drugs, so it's wise to inform your pharmacist about any other medications you are taking.
Gaviscon:
Gaviscon is not an antacid but rather a raft-forming alginate. It floats on top of the stomach acid, creating a physical barrier that prevents acid from reaching the oesophagus. Gaviscon is often found to be very helpful when taken regularly after meals and at bedtime. This can also be purchased over the counter.
When to Seek Further Advice
While lifestyle changes and OTC remedies can manage many cases of GORD, persistent or severe symptoms warrant professional medical attention. If your symptoms do not improve after six weeks of consistent self-care, or if you experience any of the following, consult your GP:
- Difficulty swallowing (dysphagia)
- Pain when swallowing (odynophagia)
- Unexplained weight loss
- Vomiting blood or material that looks like coffee grounds
- Black, tarry stools
- A persistent cough or hoarseness
- Chest pain (especially if it is severe or accompanied by shortness of breath)
Frequently Asked Questions about GORD
Q1: How long does it take to feel relief from GORD?
A1: With consistent application of dietary and lifestyle changes, you might start to feel some relief within a few weeks. However, significant healing of the irritated oesophagus and throat can take at least four to six weeks of careful treatment.
Q2: Can I still eat my favourite foods if I have reflux?
A2: It's often a process of identifying your personal triggers. While some foods are common culprits, you might find you can tolerate small amounts of certain foods without issue. Experiment cautiously and keep a food diary to track your reactions.
Q3: Is GORD the same as heartburn?
A3: Heartburn is a common symptom of GORD, but GORD is the underlying condition. Heartburn is the burning sensation caused by stomach acid backing up into the oesophagus. GORD encompasses this and other potential symptoms and complications.
Q4: Can stress really make my reflux worse?
A4: Yes, stress can significantly impact your digestive system. It can alter gut motility and increase sensitivity to pain, potentially exacerbating reflux symptoms. Managing stress is therefore an important part of managing GORD.
Q5: What's the difference between an antacid and Gaviscon?
A5: Antacids neutralise stomach acid, providing quick but often short-lived relief. Gaviscon forms a protective barrier over the stomach acid, preventing it from irritating the oesophagus, and is often more effective for longer-term symptom control, especially when taken regularly.
Further Information
For comprehensive online information and guidance on all aspects of health and healthcare, NHS Choices is an excellent resource. Making informed choices about your health is paramount, and understanding your condition is the first step towards effective management and a better quality of life.
If you want to read more articles similar to Beat Acid Reflux: Your Guide to Relief, you can visit the Automotive category.
