03/01/2025
In the United Kingdom, a significant number of people rely on beta-blocker medications to manage various health conditions. With over 50 million prescriptions issued annually, understanding these drugs is crucial for many. Beta-blockers, or beta-adrenoceptor blocking agents as they are formally known, primarily target the beta-adrenoceptors found in vital areas of the body, including the heart, peripheral blood vessels, bronchi, pancreas, and liver. While a wide array of beta-blockers are available, they are generally considered equally effective in their primary functions.
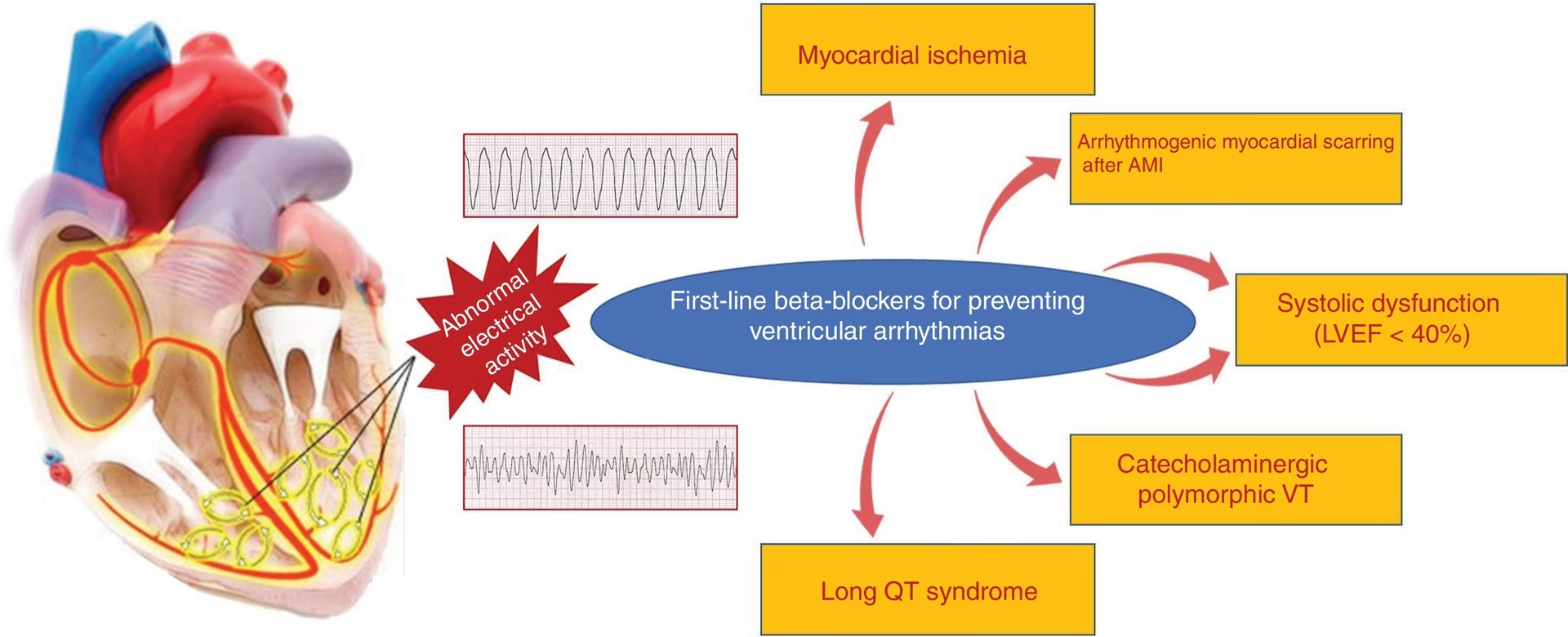
- What Are Beta-Blockers Used For?
- How Do Beta-Blockers Work?
- Why Would I Be Prescribed a Beta-Blocker?
- Types of Beta-Blockers: Selective vs. Non-Selective
- Are Beta-Blockers Safe for Everyone?
- Potential Side Effects of Beta-Blockers
- What If I Miss a Dose?
- Alternatives to Beta-Blockers
- Important Considerations
- Common Beta-Blockers in the UK:
What Are Beta-Blockers Used For?
The most common applications for beta-blockers lie in the management of heart and circulatory conditions. They are frequently prescribed to address:
- Irregular Heart Rhythms (Arrhythmias): Beta-blockers help to regulate the heart's rhythm, preventing it from beating too fast or erratically.
- Angina: By slowing the heart rate, beta-blockers reduce the heart's oxygen demand, thereby decreasing the frequency and severity of angina episodes.
- High Blood Pressure (Hypertension): While not always a first-line treatment, they are used when other medications are insufficient or for specific patient profiles.
Furthermore, individuals with conditions such as heart valve disease, heart failure, or those who have experienced a heart attack may also be prescribed beta-blockers as part of their treatment plan. Beyond cardiovascular health, doctors sometimes utilise beta-blockers for non-heart-related issues, notably anxiety, where they can help mitigate the physical symptoms of stress.
How Do Beta-Blockers Work?
Beta-blockers exert their effects by counteracting the action of stress hormones, namely adrenaline and noradrenaline. These hormones can stimulate the heart to beat faster and with greater force. By blocking the receptors that these hormones bind to, beta-blockers achieve the following:
- Slowing Heart Rate: This directly reduces the workload on the heart.
- Reducing Pumping Force: Less forceful contractions also contribute to a lower workload.
- Relaxing Blood Vessels: Some beta-blockers also have the effect of widening blood vessels, which can further help in lowering blood pressure.
- Kidney Influence: Certain beta-blockers can inhibit the production of angiotensin II by the kidneys, a hormone that constricts blood vessels and raises blood pressure.
A normal resting heart rate for adults is typically between 60 and 100 beats per minute (bpm), with a healthy blood pressure range of 90/60 mmHg to 120/80 mmHg. For individuals over 80, these parameters may be slightly higher due to natural age-related stiffening of arteries.
Why Would I Be Prescribed a Beta-Blocker?
The decision to prescribe a beta-blocker is based on a thorough assessment of a patient's medical history and current condition. Here are some key reasons:
Angina
Clinical guidelines strongly recommend beta-blockers as a primary treatment for angina. They are often used alone or in conjunction with calcium channel blockers. By reducing the heart's oxygen requirement, they effectively minimise angina attacks.
Heart Failure
For a specific type of heart failure, known as 'heart failure with reduced ejection fraction' (HFrEF), beta-blockers are proven to improve life expectancy. They are recommended for all patients with HFrEF, irrespective of symptom severity, and are typically prescribed alongside an ACE inhibitor.

Heart Valve Disease
If you have been diagnosed with heart valve disease, your doctor will likely include a beta-blocker in your treatment regimen.
Irregular Heart Rhythm (Arrhythmia)
Beta-blockers are effective in controlling irregular heart rhythms, such as atrial fibrillation, by helping to restore a normal heart rate and reducing symptoms like palpitations and fatigue.
Heart Attacks
Following a heart attack, patients are typically prescribed beta-blockers before hospital discharge to significantly reduce the risk of a subsequent event. This treatment is often lifelong.
High Blood Pressure
Beta-blockers are considered for individuals with high blood pressure that is resistant to other treatments, often as part of a multi-drug therapy plan.

Anxiety
The beta-blocker propranolol is particularly useful for short-term management of anxiety. It works by blocking the physical effects of adrenaline and noradrenaline, such as sweating, trembling, and rapid heart rate, which are triggered by the body's 'fight or flight' response.
Types of Beta-Blockers: Selective vs. Non-Selective
Beta-blockers can be broadly categorised into two main types:
| Type | Examples | Primary Action & Use | Potential Side Effects |
|---|---|---|---|
| Selective | Atenolol, Bisoprolol, Nebivolol | Primarily block beta-receptors in the heart, leading to fewer effects on other body parts. Commonly used for heart conditions. | Generally fewer side effects compared to non-selective types. |
| Non-Selective | Propranolol, Nadolol | Block beta-receptors in both the heart and other areas of the body. Often used for non-heart conditions like anxiety. | Can cause side effects such as cold extremities and may trigger asthma attacks in susceptible individuals. |
Are Beta-Blockers Safe for Everyone?
Beta-blockers are not suitable for all individuals. They are generally not recommended for those with:
- Uncontrolled heart failure
- Very low blood pressure (hypotension)
- Certain heart rhythm disorders
- Bradycardia (a very slow heartbeat)
Individuals with respiratory conditions like asthma or COPD may also not be prescribed beta-blockers due to the risk of precipitating severe asthma attacks. A doctor will carefully weigh the potential benefits against these risks.
Potential Side Effects of Beta-Blockers
While many people tolerate beta-blockers well with minimal or no side effects, some common reactions can occur:
- Cold hands and feet
- Unusual or vivid dreams
- Fatigue, potentially due to an excessively slow heart rate
- Erectile dysfunction in some men
- Dizziness
- Tiredness
- Blurred vision
- Diarrhoea
- Nausea
It is crucial to consult your doctor if you experience side effects, as stopping beta-blockers abruptly can lead to serious complications, including heart palpitations, a return of angina, or a dangerous rise in blood pressure. Your doctor may adjust the dosage or switch you to a different, perhaps more selective, beta-blocker.
What If I Miss a Dose?
If you forget to take your beta-blocker dose, it's important to consult the patient information leaflet that accompanies your medication for specific advice. Never take a double dose to compensate for a missed one. If you accidentally take more than prescribed, seek immediate advice from your pharmacist or GP practice, or call 111.

Alternatives to Beta-Blockers
If beta-blockers are not tolerated or are contraindicated, several alternative medications exist. For conditions like angina or atrial fibrillation, drugs such as diltiazem or verapamil can help slow the heart rate. Ivabradine is another option for angina that specifically targets heart rate reduction.
Important Considerations
- Diabetes: Beta-blockers can mask the symptoms of low blood sugar (hypoglycaemia) in individuals with diabetes. More frequent blood sugar monitoring may be necessary.
- Drug Interactions: Beta-blockers can interact with other medications, including anti-arrhythmics, antihypertensives, and certain antipsychotics. Always inform your doctor and pharmacist about all medications you are taking.
- Pregnancy and Breastfeeding: Consult your GP for advice on suitable medications during pregnancy or breastfeeding.
- Driving and Operating Machinery: Avoid these activities if you experience dizziness, tiredness, or visual disturbances after taking beta-blockers.
Reporting Side Effects: If you suspect you are experiencing side effects from your medication, you can report them through the Yellow Card Scheme, managed by the Medicines and Healthcare products Regulatory Agency (MHRA).
Common Beta-Blockers in the UK:
Some of the commonly prescribed beta-blockers in the UK include:
- Atenolol (e.g., Tenormin)
- Bisoprolol (e.g., Cardicor, Congescor)
- Carvedilol
- Metoprolol (e.g., Betaloc, Lopresor)
- Nebivolol (e.g., Nebilet)
- Propranolol (e.g., Inderal)
Always take your beta-blocker exactly as prescribed by your doctor. It may take several weeks or even months to feel the full benefits, and initial symptom worsening is possible. Patience and adherence to your treatment plan are key to long-term health improvement.
If you want to read more articles similar to Understanding Beta-Blockers: Your Guide, you can visit the Automotive category.
