15/06/2011
- Navigating the Discomfort: Understanding and Relieving Pregnancy Constipation
- What is Constipation?
- Common Culprits Behind Constipation
- When to Seek Medical Advice
- Recognising the Signs: Symptoms of Constipation
- Tailoring Treatment: Strategies for Pregnancy Constipation
- Understanding Dyssynergic Defecation
- Managing Severe or Chronic Constipation
- Prognosis for Constipation During Pregnancy
- Frequently Asked Questions (FAQs)
Pregnancy is a time of immense joy and significant bodily changes. While many embrace the transformation, some women find themselves grappling with an unwelcome companion: constipation. This common ailment can add an extra layer of discomfort to an already sensitive period. But what exactly is constipation, and more importantly, what can be done about it, especially when you're expecting? This article delves into the causes, symptoms, and, most crucially, the best strategies for managing constipation during pregnancy, offering practical advice and actionable steps for expectant mothers.
What is Constipation?
Constipation is generally defined as difficulty passing stools, a reduced frequency of bowel movements compared to your normal routine, or the passage of hard, dry stools. It's a widespread issue that can affect anyone, but it's particularly prevalent during pregnancy due to a confluence of hormonal and physical factors. Understanding its fundamental nature is the first step towards effective management.
Common Culprits Behind Constipation
Several factors contribute to the onset of constipation, and during pregnancy, these are often amplified:
- Low-Fibre Diet: A diet lacking in dietary fibre can significantly slow down the digestive process, leading to harder, more difficult-to-pass stools.
- Inadequate Fluid Intake: Water is essential for softening stools and facilitating their passage. Not drinking enough fluids can exacerbate constipation.
- Reduced Physical Activity: While it might be tempting to rest more during pregnancy, a lack of regular exercise can slow down bowel function.
- Underlying Digestive Issues: Some individuals may have a naturally slower digestive system.
- Medications: Certain medications, including some commonly prescribed during pregnancy like iron supplements, can have constipation as a side effect.
- Underlying Medical Conditions: In rarer cases, persistent constipation can be a symptom of more serious health issues.
When to Seek Medical Advice
While occasional constipation is common and often manageable at home, certain symptoms warrant a consultation with your doctor. It's crucial to be aware of these red flags:
- Rectal Bleeding: While often caused by haemorrhoids or anal fissures (a small tear), blood in the stool can sometimes indicate a more serious condition.
- Sudden, Unexplained Weight Loss: This is a general health concern that should always be investigated by a medical professional.
- Sudden Onset of Constipation: A new, abrupt change in bowel habits can be a cause for concern.
- Sensation of Blockage: Feeling like something is physically obstructing the passage of stool requires medical evaluation.
- Rectal Prolapse: This is a condition where part of the rectum protrudes from the anus.
- Persistent Narrowing of Stool: A consistent change in the diameter of your stools could indicate a narrowing in the lower bowel.
Additionally, if you are over 50 years old and experience constipation, it's advisable to consult a doctor, even outside of pregnancy. If your constipation persists for more than two weeks without improvement despite home care, medical advice is recommended. Your doctor can usually diagnose constipation through a discussion of your symptoms and a physical examination. Further investigations may be conducted to rule out any underlying serious conditions.
Recognising the Signs: Symptoms of Constipation
Beyond the fundamental difficulty in passing stools, several other symptoms can accompany constipation:
- Less frequent bowel movements than usual.
- Painful or difficult bowel movements.
- Hard, lumpy, or pellet-like stools.
- A feeling of incomplete bowel emptying.
- Abdominal pain or cramping.
- Bloating and discomfort.
- General fatigue.
Tailoring Treatment: Strategies for Pregnancy Constipation
The approach to managing constipation during pregnancy often focuses on lifestyle adjustments and, if necessary, safe medical interventions. The goal is to find a balance that promotes regular, comfortable bowel movements.
Dietary Adjustments: The Power of Fibre and Fluids
This is arguably the most important aspect of managing constipation during pregnancy. Increasing your intake of fibre and fluids can make a significant difference:
Fibre-Rich Foods: Fibre adds bulk to your stool and softens it, making it easier to pass. Aim to incorporate a variety of these into your diet:
| Food Group | Examples |
|---|---|
| Fruits | Berries, apples (with skin), pears, prunes, figs, dates |
| Vegetables | Root vegetables (carrots, potatoes), broccoli, Brussels sprouts, leafy greens |
| Whole Grains | Oatmeal, wholemeal bread, wholewheat pasta, brown rice, bran cereals |
| Legumes | Beans, lentils, peas |
| Nuts and Seeds | Almonds, walnuts, chia seeds, flaxseeds |
Hydration is Key: Drink plenty of water throughout the day. Starting your day with a large glass of water can be particularly beneficial. Other fluids like herbal teas (check for pregnancy safety) and diluted fruit juices can also contribute to your daily fluid intake.
Lifestyle Modifications: Gentle Movement and Routine
In addition to diet, these lifestyle changes can support healthy bowel function:
- Regular Exercise: Aim for at least 30 minutes of moderate exercise most days of the week. Walking, swimming, and prenatal yoga are excellent options. Even short, regular walks can stimulate bowel activity.
- Establish a Routine: Try to go to the toilet at the same time each day, ideally after a meal, as this can help train your body's natural bowel reflexes. Don't ignore the urge to go.
When Lifestyle Changes Aren't Enough: Safe Over-the-Counter Options
If dietary and lifestyle changes don't provide sufficient relief, your doctor or pharmacist may recommend safe over-the-counter (OTC) options. It's crucial to discuss any medication or supplement with your healthcare provider during pregnancy.
- Bulk-Forming Laxatives: These work by absorbing water in the gut to create softer, bulkier stools. Examples include psyllium (like bran or linseeds) and methylcellulose. They are generally considered safe and effective.
- Stool Softeners: These medications, such as docusate sodium, help to draw water into the stool, making it softer and easier to pass. They are often recommended for those with hard stools.
- Osmotic Laxatives: Lactulose is a common example. It works by drawing water into the bowel, which softens the stool and stimulates bowel movements. It's generally considered safe for pregnant women.
Important Note on Iron Supplements: If you are taking iron supplements and experiencing constipation, speak to your doctor. They may be able to switch you to a different type of iron supplement that is less likely to cause this side effect, or suggest ways to manage it.
Prunes: Often referred to as a natural laxative, prunes are high in fibre and sorbitol, a natural sugar that can help stimulate bowel movements. Enjoying a few prunes daily can be an effective remedy.
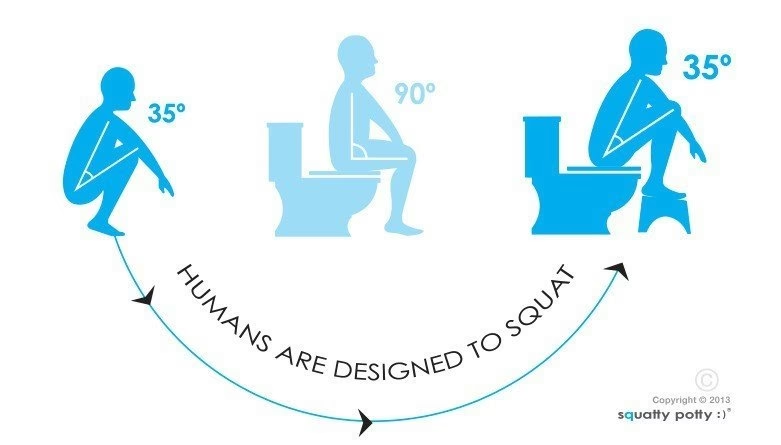
Understanding Dyssynergic Defecation
In some cases, constipation can be linked to a condition called dyssynergic defecation. This occurs when the muscles involved in bowel movements, particularly the pelvic floor muscles and those surrounding the anus, do not coordinate properly. This can lead to difficulty in expelling stools. If dyssynergic defecation is suspected, a treatment called biofeedback therapy may be recommended. This therapy aims to improve your control over these specific muscles, and many individuals experience significant improvement with it.
Managing Severe or Chronic Constipation
For individuals with severe, chronic constipation that does not respond to conventional treatments, surgery might be considered. However, this is typically a last resort and is most commonly used for rare congenital conditions affecting the bowel.
Prognosis for Constipation During Pregnancy
The prognosis for constipation during pregnancy is generally good. With appropriate dietary adjustments, increased fluid intake, regular physical activity, and, if necessary, safe medical interventions, most women can effectively manage and overcome constipation. The key is to be proactive, listen to your body, and seek professional advice when needed. By adopting these strategies, expectant mothers can significantly improve their comfort and well-being throughout their pregnancy journey.
Frequently Asked Questions (FAQs)
Q1: Is constipation common during pregnancy?
Yes, constipation is very common during pregnancy, affecting a large percentage of expectant mothers.
Q2: What is the best natural remedy for pregnancy constipation?
Increasing fibre intake through fruits, vegetables, and whole grains, along with drinking plenty of water and incorporating gentle exercise like walking, are considered the best natural remedies.
Q3: Can I take laxatives during pregnancy?
Some laxatives are considered safe during pregnancy, but it is essential to consult your doctor or pharmacist before taking any medication, including over-the-counter laxatives.
Q4: How much water should I drink to help with constipation?
General recommendations suggest aiming for at least 8-10 glasses (around 2-2.5 litres) of water per day, but individual needs may vary. Listen to your body and drink when you are thirsty.
Q5: When should I see a doctor about my constipation?
You should see a doctor if your constipation is severe, persists for more than two weeks despite home care, or if you experience any of the red flag symptoms mentioned earlier, such as rectal bleeding or unexplained weight loss.
If you want to read more articles similar to Pregnancy Constipation Relief, you can visit the Automotive category.
