05/09/2023
In the intricate world of healthcare, the financial pulse of an institution is often measured by its operating margin. This vital metric offers a clear snapshot of a hospital’s financial health, indicating how efficiently it manages its core operations. While specific figures for UK hospital operating margins in 2022 are not readily available in the detailed data provided, the fundamental principles, challenges, and importance of this metric remain universally relevant across the healthcare sector, including the National Health Service (NHS) and private hospitals in the UK.
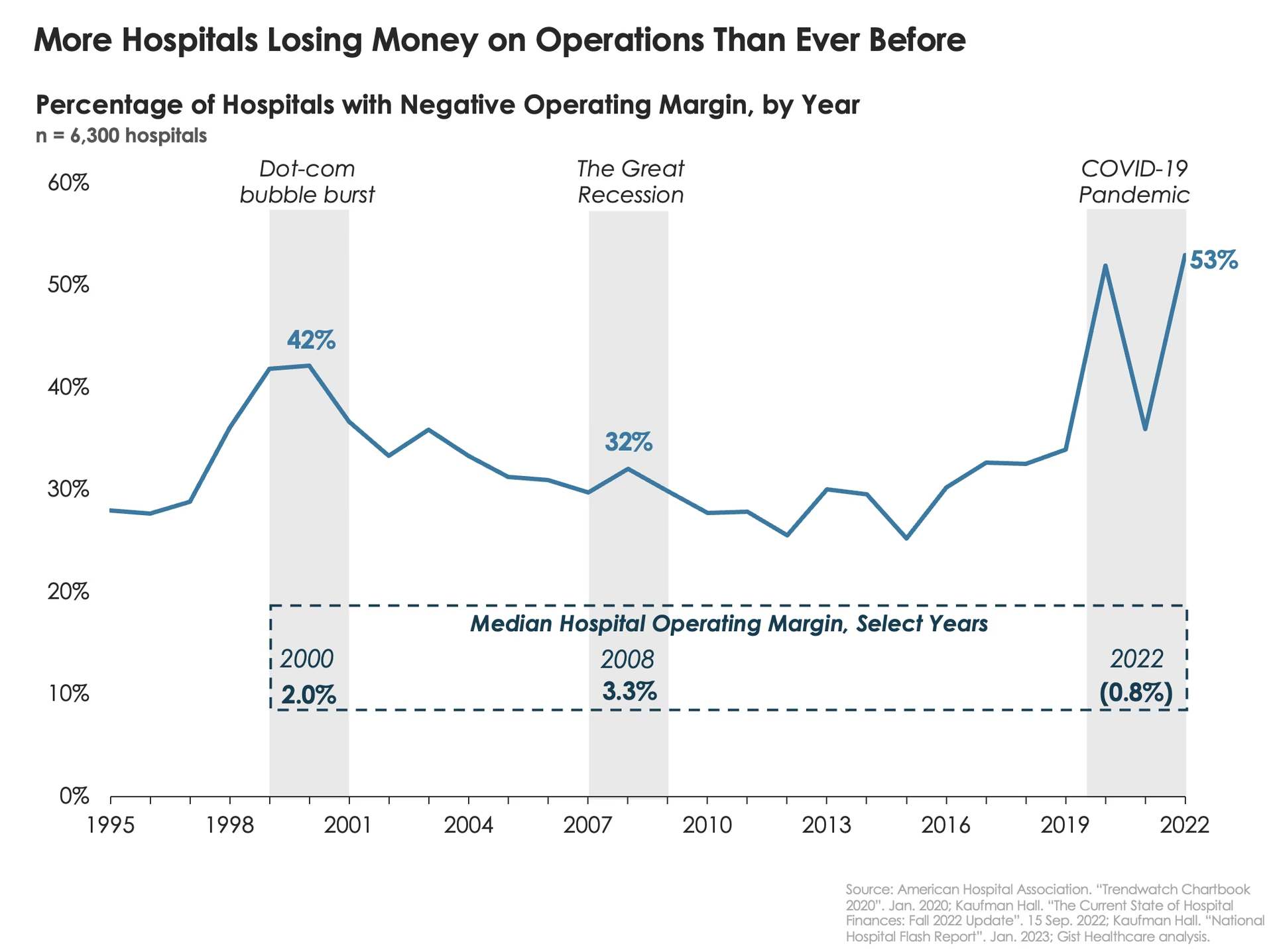
Understanding the operating margin is more than just an accounting exercise; it's about comprehending the capacity of a hospital to invest in new technologies, maintain quality care, attract skilled staff, and ultimately, serve its community effectively. The healthcare landscape is dynamic, fraught with rising costs, evolving patient needs, and shifting economic pressures, making the management of operating margins a perpetual high-wire act for hospital leaders.
- Understanding the Hospital Operating Margin
- The Critical Role of Operating Margin for Hospitals
- Key Factors Influencing Hospital Operating Margins
- Navigating Financial Headwinds: The Hospital Financial Performance Gap
- The Landscape of Healthcare Profitability: An Illustrative Overview
- Strategies for Margin Improvement in Hospitals
- Balancing Financial Health and Quality Healthcare Services
- Frequently Asked Questions (FAQs)
- Conclusion
Understanding the Hospital Operating Margin
At its core, the operating margin represents the percentage of revenue left after deducting operating expenses. It is calculated by dividing a hospital's operating income by its total operating revenue. Operating income includes revenue generated from patient care, such as medical procedures, consultations, and hospital stays, minus the direct costs associated with providing those services, including staff salaries, medical supplies, utilities, and administrative overheads.
Unlike net profit margin, which includes non-operating income and expenses (like investment income or one-off sales of assets), the operating margin focuses purely on the profitability of a hospital's primary activities. A robust operating margin suggests that a hospital is efficiently delivering its core services, generating enough income to cover its day-to-day running costs and ideally, have a surplus for reinvestment.
The Critical Role of Operating Margin for Hospitals
For any hospital, whether publicly funded like those within the NHS or privately owned, a healthy operating margin is paramount for long-term sustainability and the continuous provision of high-quality care. Here’s why it’s so critical:
- Sustainability and Resilience: A positive operating margin ensures that a hospital can cover its bills, pay its staff, and avoid debt. Without it, institutions face the risk of financial distress, potentially leading to service cuts or even closure.
- Investment in Infrastructure and Technology: Modern healthcare relies heavily on cutting-edge equipment, advanced IT systems, and up-to-date facilities. Surplus funds from a strong operating margin allow hospitals to invest in these crucial areas, improving diagnostic capabilities, treatment options, and patient experience.
- Staffing and Training: Attracting and retaining top medical talent requires competitive salaries, continuous professional development, and a supportive working environment. A healthy margin enables investment in human capital, which directly translates to better patient care.
- Quality of Care: Ultimately, financial stability underpins the ability to deliver high-quality patient care. It allows for appropriate staffing levels, access to necessary supplies, and the implementation of best practices, all of which contribute to improved patient outcomes and safety.
Key Factors Influencing Hospital Operating Margins
Hospitals operate within a complex financial ecosystem, and their operating margins are influenced by a multitude of factors. While the specific context of the UK’s NHS differs from a predominantly insurance-based system, many underlying pressures are universal:
Payer Mix and Funding Models
In the UK, NHS hospitals are primarily funded through general taxation, with budgets allocated by the government. While this provides a degree of stability, it also means hospitals are heavily reliant on government policy and funding decisions. Shifts in government-sponsored insurance or funding models can significantly impact the revenue streams available to NHS trusts. Private hospitals, on the other hand, deal with a mix of private insurance payments and self-paying patients, and their margins can be affected by changes in insurance reimbursement rates or patient willingness to pay out-of-pocket.

Rising Operating Costs
Healthcare is an incredibly cost-intensive industry. Hospitals face ever-increasing expenses across several categories:
- Staffing Costs: Wages and benefits for doctors, nurses, and support staff represent a significant portion of a hospital's budget. Shortages of skilled personnel can drive up costs due to reliance on agency staff or overtime.
- Medical Supplies and Equipment: The cost of pharmaceuticals, disposables, and highly specialised medical equipment continues to rise.
- Technology and Innovation: Investing in new medical technologies, from advanced imaging machines to electronic health record systems, is essential but expensive.
- Utilities and Maintenance: Running large facilities requires substantial expenditure on energy, water, and building maintenance.
Demographic and Site-of-Care Utilisation Shifts
Population ageing and the increasing prevalence of chronic conditions mean that hospitals are often dealing with patients presenting with greater medical complexity. These cases typically require more resources, longer stays, and more intensive care, driving up the cost per patient. Furthermore, shifts towards more care being delivered outside of traditional hospital settings (e.g., in community clinics or at home) can alter the case mix for hospitals, potentially leaving them with the most complex and expensive cases.
Reliance on Non-Operating Revenue Sources
While operating margin focuses on core activities, some hospitals may rely on non-operating revenues, such as investment income, charitable donations, or supplemental payments. While these can provide a financial cushion, their unpredictable nature means they cannot be relied upon for sustainable operational stability. For NHS trusts, charitable donations often play a crucial role in funding enhancements beyond core services.
Across the global healthcare sector, there’s a consistent narrative of a widening financial performance gap. Many organisations find themselves in a challenging position, even if they achieve periods of operating margin stability. Structural pressures are constantly looming, making long-term financial health a significant concern. These include the aforementioned shifts in payer mix, the ongoing operation within hybrid payment environments (combining fixed budgets with activity-based funding), and the increasing medical complexity of patients.
The sentiment among healthcare leaders, as evidenced by recent surveys, highlights that addressing immediate financial challenges and improving operating efficiency are top priorities. This universal response underscores that despite any temporary improvements in average margins, hospitals and health systems remain supremely challenged in the long term. The emphasis has shifted from simply growing in size or revenue to achieving sustainable growth through margin improvement and differentiated service paths. Leaders are focusing on becoming stronger and more resilient overall, rather than just bigger.

The Landscape of Healthcare Profitability: An Illustrative Overview
It's important to note that the 'average' profit margin in healthcare can vary wildly depending on the type of provider and the specific market. For instance, a large NHS teaching hospital will have a vastly different financial structure and objective compared to a small private cosmetic surgery clinic.
While specific UK hospital operating margins for 2022 are not provided, the following table, based on US industry data, offers an illustrative comparison of typical profit margins across different healthcare sub-sectors. This demonstrates the diversity of financial performance within the broader healthcare industry and highlights that hospitals, particularly large public ones, often operate on much tighter margins than some specialised private clinics.
Illustrative Profit Margins Across Healthcare Sub-sectors (Based on US Data)
| Industry Name | Gross Margin | Net Margin | Pre-tax, Pre-stock Operating Margin |
|---|---|---|---|
| Healthcare Products (e.g., supplement shops) | 57.74% | 7.00% | 17.41% |
| Healthcare Support Services | 14.72% | 2.01% | 4.35% |
| Healthcare Facilities (including hospitals) | 35.63% | 5.31% | 12.24% |
| Urgent Care Centres (Private, US Average) | N/A | 15% (Successful Average) | N/A |
| Dental Clinics (Private, US Average) | N/A | 30-40% | N/A |
Note: This table is based on US industry averages and is illustrative. 'Net Margin' can be misleading for owner-operated clinics as owner compensation is an expense. 'Pre-tax, pre-stock operating margin' often provides a more relevant picture for small private businesses. Large public hospitals, like those in the NHS, do not typically aim for 'profit' in the same way as private enterprises, but rather for financial sustainability and efficiency to meet public health needs.
Strategies for Margin Improvement in Hospitals
Maintaining a healthy operating margin is a continuous challenge, but hospitals can employ several strategies to improve their financial standing:
- Cost Reduction and Efficiency: This is often the primary focus. It involves negotiating better prices with suppliers, optimising staff scheduling to reduce overtime, streamlining administrative processes through technology, and identifying areas of waste.
- Revenue Enhancement (where applicable): For private hospitals, this might involve expanding service lines, attracting new patient populations, or optimising billing and collection processes. For NHS trusts, it often means ensuring full utilisation of capacity and efficient patient flow to meet activity targets and secure funding.
- Technology Adoption: Implementing new technologies like telehealth can reduce operating costs by enabling remote consultations and monitoring, potentially reducing the need for expensive in-person visits. Advanced analytics can also help identify inefficiencies and opportunities for improvement.
- Strategic Partnerships: Collaborating with other healthcare providers or organisations can lead to shared resources, economies of scale, and improved service delivery, ultimately positively impacting margins.
Balancing Financial Health and Quality Healthcare Services
The inherent tension in healthcare lies in balancing the need for financial viability with the imperative to provide high-quality, accessible care. For NHS trusts, this means operating within allocated budgets while striving to meet ever-increasing demand and clinical standards. For private hospitals, it means generating sufficient surplus to reinvest while remaining competitive on price and quality.
Hospital leaders must make difficult decisions that balance fiscal responsibility with patient needs. This requires a deep understanding of their organisation's strengths and capabilities, allowing them to prioritise investments and navigate a tumultuous future. The goal is not just to survive but to thrive, ensuring that communities have access to the essential healthcare services they need.

Frequently Asked Questions (FAQs)
Q1: What is the primary difference between operating margin and net profit margin for a hospital?
The operating margin focuses solely on the profitability of a hospital's core healthcare services, calculated from operating revenue minus operating expenses. The net profit margin, conversely, includes all revenues and expenses, both operating and non-operating (e.g., investment income, taxes, interest), providing a broader, 'bottom-line' view of overall profitability.
Q2: Why do hospital operating margins fluctuate so much?
Hospital operating margins are highly susceptible to fluctuations due to several factors. These include changes in patient volume and case mix, unexpected surges in demand (like pandemics), shifts in funding or reimbursement policies, rising costs of medical supplies and labour, and the unpredictable nature of non-operating income sources.
Q3: How does a low operating margin impact patient care?
A consistently low or negative operating margin can severely impact patient care. It limits a hospital's ability to invest in new medical equipment, recruit and retain skilled staff, upgrade facilities, and fund vital training programmes. This can lead to longer waiting lists, reduced access to advanced treatments, and potential compromises in the overall quality and safety of care provided.
Conclusion
The operating margin is a cornerstone of hospital financial management, reflecting the efficiency and sustainability of its core services. While specific data for UK hospital operating margins in 2022 remains elusive in the provided information, the underlying challenges and strategic imperatives are clear. Hospitals, whether part of the NHS or private entities, face a constant battle against rising costs, evolving patient needs, and structural financial pressures. The ability to effectively manage and improve operating margins is not merely a financial objective; it is fundamental to a hospital's capacity to deliver high-quality patient care, innovate, and remain a vital pillar of the community's health infrastructure. Adaptability, strategic cost management, and a keen understanding of both internal capabilities and external market forces are crucial for navigating the complex financial landscape of modern healthcare.
If you want to read more articles similar to Navigating Hospital Operating Margins in the UK, you can visit the Automotive category.
