09/08/2018
Hand, Foot & Mouth Disease (HFMD) is a surprisingly common viral infection, often striking children under the age of five, though it can affect older children and even adults. While typically a mild and self-limiting illness, it can cause significant discomfort for those affected. Many parents wonder about its nature, how to manage it, and, crucially, whether their little ones can contract it more than once. The short answer to that common query is yes, it's entirely possible to experience HFMD multiple times throughout life. This comprehensive guide will delve into everything you need to know about HFMD, from its causes and symptoms to effective home care and prevention strategies, all tailored for a UK audience.
- Understanding Hand, Foot & Mouth Disease (HFMD)
- Recognising the Symptoms of HFMD
- Contagion and Spread: How HFMD Travels
- Managing HFMD Symptoms: Comfort is Key
- Hand, Foot & Mouth and School/Nursery Attendance
- Duration and Rare Complications of HFMD
- HFMD and Pregnancy: What You Need to Know
- Frequently Asked Questions About HFMD
Understanding Hand, Foot & Mouth Disease (HFMD)
Hand, Foot & Mouth Disease is an infection primarily caused by the Coxsackie A16 virus, a member of the enterovirus family. Less commonly, other related viruses, such as enterovirus 71 or other strains of Coxsackievirus, can be responsible. Unlike bacterial infections, HFMD is viral, meaning antibiotics are entirely ineffective as a treatment. The illness typically runs its course, with symptoms resolving on their own within 7 to 10 days.
It’s important to distinguish HFMD from Foot and Mouth Disease, which affects farm animals and is caused by a completely different virus. There is no link between the two, and humans cannot catch the animal disease. HFMD in humans is generally mild, but understanding its origins and how it manifests is the first step towards effective management.
What Causes HFMD?
As mentioned, the primary culprits are viruses from the enterovirus genus. The most frequent cause is Coxsackievirus A16, but Enterovirus 71 is also a known cause and can, in rare instances, lead to more severe complications. These viruses are highly contagious and spread easily, particularly in environments where young children gather, such as nurseries and schools. Understanding the viral nature of HFMD helps explain why specific treatments are limited and why hygiene plays such a crucial role in prevention.
Recognising the Symptoms of HFMD
The onset of Hand, Foot & Mouth Disease often mimics other common childhood illnesses, starting with general malaise before the more distinctive signs appear. Recognising these symptoms early can help in managing the child's comfort and preventing further spread.
Initial symptoms commonly include:
- A high temperature (fever)
- A sore throat
- Reduced appetite
- A general feeling of being unwell or irritable
After this initial phase, which typically lasts a day or so, the more characteristic signs of HFMD begin to emerge. A sore throat often becomes more pronounced, quickly followed by the development of small spots inside the mouth. These spots rapidly progress into painful mouth ulcers, which can make eating and drinking quite challenging for children.
The Distinctive HFMD Rash
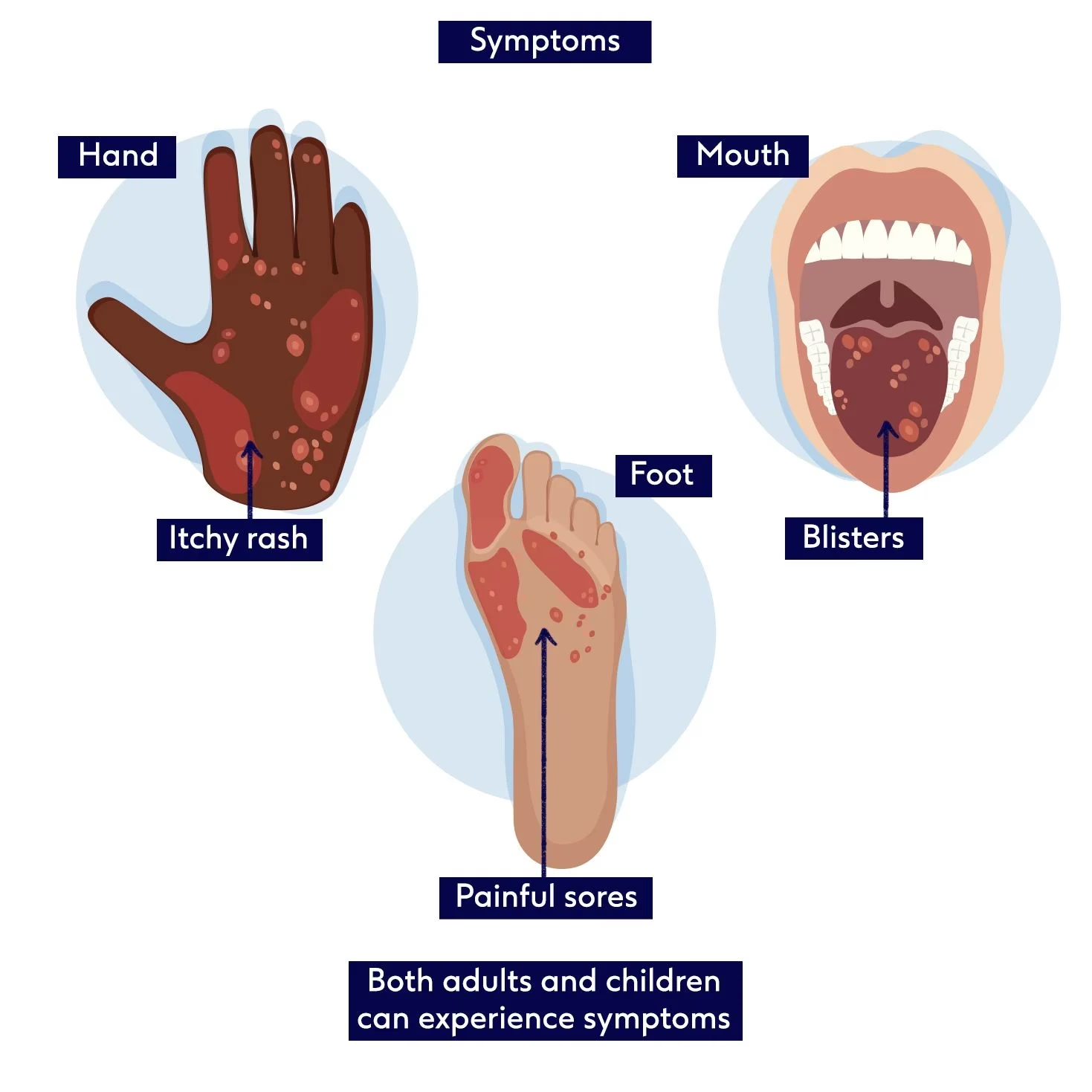
Approximately a day after the mouth ulcers appear, a rash usually develops on the skin. This rash is a key indicator of HFMD. The spots are small, typically a few millimetres in diameter, and appear as small lumps. They are most commonly found on the palms of the hands and the soles of the feet. However, it's not unusual for the spots to also appear on the buttocks, legs, and even the genital area. Rarely, they may develop on other parts of the body.
While the rash can resemble chickenpox, there are a few key differences. HFMD spots are generally smaller than chickenpox lesions. Crucially, unlike chickenpox, they are not usually itchy, though they can sometimes be a little bit sore to the touch. The presence of mouth ulcers combined with this specific rash pattern on the hands and feet is highly indicative of HFMD.
| Symptom | Description | Typical Onset |
|---|---|---|
| High Temperature (Fever) | Often one of the first signs, indicating the body's fight against infection. | Initial 1-2 days |
| Sore Throat | Can make swallowing difficult, often precedes mouth sores. | Shortly after fever |
| Reduced Appetite | Due to general malaise and sore throat/mouth. | Initial 1-2 days |
| Mouth Sores/Ulcers | Small spots develop inside the mouth, progressing to painful ulcers. Can also appear on lips. | Quickly after sore throat |
| Skin Rash | Small, non-itchy (but sometimes sore) red spots, typically on palms and soles. Can also be on buttocks, legs, genitals. | About a day after mouth ulcers |
| General Malaise | Feeling unwell, tired, irritable. | Initial 1-2 days |
Contagion and Spread: How HFMD Travels
Hand, Foot & Mouth Disease is highly contagious, and understanding its transmission routes is vital for preventing its spread, especially within family units and communal settings like nurseries. The incubation period for HFMD is typically 3 to 5 days, meaning it can take several days for symptoms to appear after a person has been infected.

The virus spreads primarily through:
- Respiratory Droplets: Coughs and sneezes can release virus particles into the air, which can then be inhaled by others.
- Direct Contact: Touching the fluid from the blisters or mouth ulcers of an infected person can transmit the virus.
- Faecal-Oral Route: The virus can be passed in stools (faeces). If an infected person doesn't wash their hands thoroughly after using the toilet, they can easily pass the virus onto surfaces or other people.
Individuals are mainly infectious until the spots and mouth ulcers have completely gone. However, it's crucial to note that the virus can still be shed in faeces for several weeks after the symptoms have resolved. This extended period of mild infectiousness underscores the importance of continued good hygiene practices long after recovery.
Preventing the Spread of HFMD
Given its highly contagious nature, robust hygiene practices are the cornerstone of preventing HFMD from spreading. While there's no vaccine available in the UK, these simple measures can significantly reduce the risk:
- Thorough Handwashing: Ensure children (and adults) wash their hands frequently and thoroughly with soap and water for at least 20 seconds, especially after using the toilet, changing nappies, and before eating. Adults should take particular care when handling soiled nappies and tissues.
- Respiratory Hygiene: Encourage covering the mouth and nose when coughing or sneezing, ideally with a disposable tissue. Dispose of used tissues immediately.
- Surface Cleaning: Regularly clean and disinfect frequently touched surfaces and shared items, such as toys, doorknobs, and tables.
- Laundry Care: Wash soiled clothes, bedding, and towels on a hot cycle in the washing machine to kill any lingering virus particles.
- Avoid Close Contact: During the infectious period, it's best to avoid sharing cups, eating utensils, towels, and other personal items with an infected person. Hugging and kissing should also be avoided.
- Do Not Pierce Blisters: The fluid inside the blisters is infectious. Do not deliberately pierce them, as this can release the virus and increase the risk of spread.
Maintaining these hygiene habits, especially in households with young children, is your best defence against HFMD.
Managing HFMD Symptoms: Comfort is Key
There is no specific antiviral treatment for Hand, Foot & Mouth Disease; the illness simply needs to run its course. The focus of management is entirely on easing symptoms and keeping the affected person, whether a child or an adult, as comfortable as possible until the virus clears. Treatment approaches are generally the same for all age groups.
Controlling a High Temperature
A fever can make anyone feel miserable and irritable. Here's how to help bring down a high temperature and improve comfort:
- Medication: You can give paracetamol or ibuprofen to help lower a fever. Both medicines also act as painkillers, which will help alleviate the soreness in the mouth. For children, these are available in liquid form or as flavoured melt-in-the-mouth tablets. Always follow the dosage instructions on the medicine packet for the appropriate age. These medicines are only necessary if the person is uncomfortable or has a fever.
- Keep Cool: Remove excessive clothing or use light cotton clothes and bedding. Opening windows or using a fan in the room can also help.
- Avoid Cold Sponging: It used to be a common practice, but cold sponging a child with a fever is no longer advised. Cold water can cause blood vessels under the skin to constrict, trapping heat deeper within the body and potentially making the child feel worse. Many children also find it uncomfortable.
Ensuring Adequate Hydration
One of the most crucial aspects of care is ensuring the person stays well-hydrated, especially given the painful mouth ulcers that can make drinking difficult. Dehydration is a rare but serious complication.
- Offer Plenty of Fluids: Encourage frequent sips of water, diluted fruit juice, or oral rehydration solutions.
- Pain Relief First: If the mouth is too sore to drink, consider giving paracetamol or ibuprofen about half an hour before offering drinks. This allows the pain relief to take effect, making it easier to swallow.
- Breastfeeding: If breastfeeding, continue to do so. Breast milk is an excellent source of fluids and nutrients. Offer feeds more often to ensure sufficient fluid intake.
Treating a Sore Mouth
The mouth ulcers can be particularly painful, making eating and drinking a challenge. Soft foods are generally easier to manage. Consider options like soups, ice cream, smoothies, yoghurt, and mashed potato.
While effectiveness varies, some treatments can help with mouth ulcers:
- Lidocaine Gel: This is a local anaesthetic that numbs the area and can be safely used in children.
- Benzydamine Mouthwash or Spray: The spray can be used from 5 years of age, while the mouthwash is suitable for those aged 12 and over.
- Choline Salicylate Gel (e.g., Bonjela®): This should NOT be used in children under 16 years of age or by pregnant women.
- Warm Salty Mouthwashes: A warm solution of salt and water can offer some relief. This should only be used if you are certain your child is old enough to rinse and spit it out without swallowing.
- Pain Relievers: Remember that paracetamol or ibuprofen will also help with the general soreness in the mouth.
When to Seek Medical Advice
While HFMD is usually mild and self-resolving, there are instances when medical attention is warranted. You should contact a doctor promptly if:
- Your child stops drinking due to a sore mouth, as this can lead to dehydration.
- You are concerned about any unusual symptoms developing.
- Your child seems unusually unwell, drowsy, or unresponsive.
- The fever persists for more than a few days, or the symptoms worsen.
- You are pregnant and suspect you have HFMD, especially close to your due date.
Hand, Foot & Mouth and School/Nursery Attendance
Guidance from Public Health England states that children with Hand, Foot & Mouth Disease do not routinely need to be kept off school or nursery/childcare, provided they are well enough to attend. While there is a risk of passing the infection on to others, the illness is generally mild. If your child feels unwell, miserable, or has a severe loss of appetite, you may wish to keep them home until they feel well enough to participate in activities. Always consult your specific school or nursery's policy, as some may have their own guidelines.
Duration and Rare Complications of HFMD
Most cases of Hand, Foot & Mouth Disease are mild and short-lived. The high temperature and skin spots typically clear within a few days. The mouth ulcers, while painful, usually last up to a week. Overall, symptoms commonly resolve within 7 to 10 days without any specific treatment.
In a very small number of cases, serious complications can arise, particularly if the infection is caused by certain strains like Enterovirus 71. These rare complications involve the virus affecting vital organs such as the heart, lungs, or brain, leading to severe inflammation. While these instances can be fatal, it is crucial to stress that such serious complications are exceedingly rare, especially in the UK.

HFMD and Pregnancy: What You Need to Know
A common concern among expectant mothers is the risk of contracting Hand, Foot & Mouth Disease during pregnancy. Fortunately, current evidence suggests that HFMD does not pose a significant risk to the developing baby. It does not appear to cause miscarriages or abnormalities.
However, if you develop symptoms of HFMD close to your delivery date (within three weeks of your due date), it is advisable to see your doctor. There is a small possibility that you could pass the infection to your newborn baby during birth. While most newborn babies who contract HFMD experience a very mild illness, it can occasionally be severe in this very young age group. Your doctor can provide specific advice and monitor the situation if you are close to delivery.
Frequently Asked Questions About HFMD
Can you get Hand, Foot & Mouth Disease more than once?
Yes, absolutely. It is possible to get Hand, Foot & Mouth Disease more than once. This is because there are several different strains of the viruses that cause HFMD. Getting infected with one strain provides immunity to that specific strain, but it doesn't protect you from catching a different strain in the future. So, if you or your child encounter a new strain, another bout of HFMD is possible.
Is Hand, Foot & Mouth Disease contagious?
Yes, HFMD is very contagious. It spreads easily through respiratory droplets from coughs and sneezes, contact with the fluid from blisters, and through contaminated faeces. This is why good hand hygiene and cleaning practices are so important in preventing its spread, especially in nurseries and schools.
How long is someone with HFMD contagious for?
Individuals with HFMD are generally most contagious until the spots and mouth ulcers have disappeared. However, the virus can still be present in stools (faeces) for several weeks after symptoms have cleared. This means that even after feeling better, a person can still mildly transmit the virus for a period, highlighting the need for continued vigilance with hygiene.
Is Hand, Foot & Mouth Disease dangerous for children?
For most children, Hand, Foot & Mouth Disease is a mild illness that resolves on its own within 7 to 10 days. Serious complications are extremely rare. The main discomfort comes from the fever and painful mouth ulcers, which can make eating and drinking difficult. Dehydration is a rare concern if a child refuses fluids. If you are ever concerned about your child's symptoms or their overall well-being, it's always best to consult a doctor.
What is the incubation period for HFMD?
The incubation period for Hand, Foot & Mouth Disease is typically between 3 to 5 days. This is the time it takes from being infected with the virus to the first appearance of symptoms. Because of this incubation period, a person can be contagious before they even show signs of the illness.
If you want to read more articles similar to Hand, Foot & Mouth: Can You Catch It Twice?, you can visit the Automotive category.
