07/02/2024
Adjusting to life with a stoma brings many changes, and one of the most common concerns for individuals in the UK is understanding what they can, and should, eat. It's a journey of discovery, as your body adapts and you learn what works best for you. While there isn't a one-size-fits-all answer, this guide aims to provide clear, practical advice on managing your diet, ensuring you maintain a balanced nutritional intake and enjoy your food with confidence after stoma formation.

Your diet plays a crucial role not only in your overall well-being but also in how your stoma functions. Eating healthily can significantly reduce discomfort, manage output, and help your body heal. Remember, the goal is to return to as normal a diet as possible, making gradual adjustments as you go.
- Understanding a Healthy Diet with a Stoma
- Eating Just After Stoma Formation: The Initial Weeks
- Dietary Considerations for Different Stoma Types
- Managing Common Stoma-Related Dietary Issues
- Alcohol and Your Stoma
- Debunking Common Stoma Diet Myths
- Frequently Asked Questions About Stoma Diet
- Seeking Professional Advice
Understanding a Healthy Diet with a Stoma
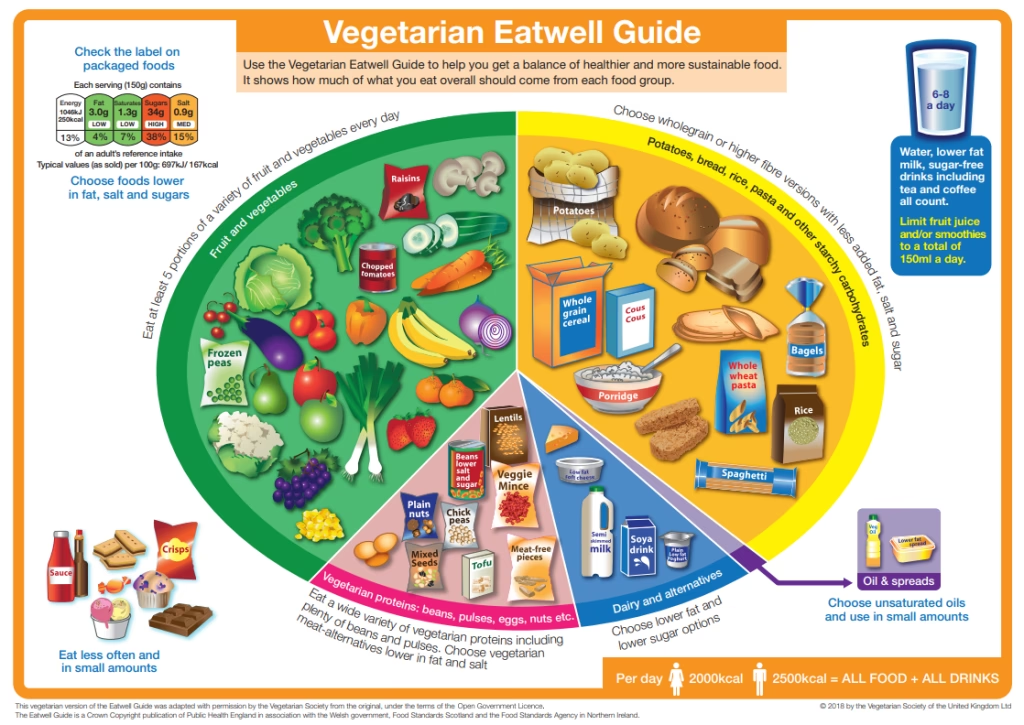
Even with a stoma, the principles of a healthy diet remain largely the same as those recommended by the Eatwell Guide. The key is often in the preparation, portion sizes, and understanding how different foods interact with your unique digestive system. Here's a breakdown of the essential food groups:
- Starchy Foods (Carbohydrates): These are your primary energy source. Include items like bread, breakfast cereals, pasta, rice, potatoes, noodles, crackers, crispbread, or couscous at each meal. In the initial weeks post-surgery, opting for white varieties over wholegrain can be beneficial as they are lower in fibre and easier to digest.
- Protein Foods: Essential for healing and muscle maintenance. Aim for two portions per day from sources such as meat, poultry, fish, eggs, lentils, tofu, beans, or plant-based alternatives like Quorn. Well-cooked, lean, and skinless options are generally preferred, especially early on.
- Dairy Products: Milk, cheese, and yoghurt are excellent sources of calcium, protein, and energy. Try to include two to three portions daily. Plain varieties are often better tolerated than those with added fruit or nuts.
- Fruit and Vegetables: Crucial for vitamins, minerals, and fibre. Aim for at least five portions daily. However, for stoma patients, preparation is key. Peeled, cooked, tinned, or pureed fruits and vegetables are often easier to digest, particularly in the initial recovery phase.
- Fats and Sugary Foods: These should be consumed in moderation. However, if you have a poor appetite or are struggling to maintain weight, small amounts of mayonnaise, butter, cheese, oil, cream, sugar, chocolates, fizzy drinks, and juice drinks can provide extra energy.
- Fluid: Staying hydrated is paramount. Aim for at least 8 to 10 glasses (1.5 to 2 litres/3 to 4 pints) of fluid per day, increasing this during warm weather or physical activity. Sports drinks can be very useful for replacing essential salts and glucose, especially for those with an ileostomy. Be mindful that tea and coffee may increase output, so keep these to a minimum if you're experiencing high output.
- Salt: For individuals with an ileostomy, increasing salt intake is often recommended to compensate for increased losses through the stoma. Adding salt to food and enjoying salty snacks like soups, Bovril, or crisps can be beneficial.
Eating Just After Stoma Formation: The Initial Weeks
The period immediately following stoma surgery, typically the first 6-8 weeks, is a sensitive time for your body. Your digestive system is adjusting, and a cautious approach to diet is essential to promote healing and minimise discomfort. During this phase, you might experience a sensitive gut or bladder, leading to symptoms like cramping, bloating, or a more liquid stool.
Hospitals often begin the process of eating and drinking soon after surgery to aid healing. It’s beneficial to consume small, frequent meals rather than large ones, and to chew your food thoroughly to assist digestion. Maintaining a daily fluid intake of around 1500-2000 ml is also vital.
Gradual Reintroduction of Foods
There are no strict, universal guidelines for reintroducing foods, as everyone's recovery is unique. If you had emergency surgery or significant internal swelling, you might need to proceed even more cautiously. Start with small portions of bland foods and observe your body's response. Spicy and fatty foods are best avoided during this initial period until the swelling has subsided.
When gradually reintroducing foods, especially higher-fibre options like fruits and vegetables, start with small amounts. These can sometimes lead to increased gas, looser stools, or abdominal discomfort. Cooked fruits and vegetables are generally better tolerated than raw ones, and root vegetables often cause fewer issues than above-ground varieties. Experimentation is key to finding what works for you.
Foods to Consider During Initial Recovery (0-8 Weeks)
The table below provides a general guide for foods to reduce or avoid, and those to include, during the sensitive post-operative period. Remember, individual tolerance varies.
| Food Group | Foods to Reduce or Avoid | Foods to Include |
|---|---|---|
| Starchy Carbohydrates | Wholemeal/granary bread with nuts, seeds, dried fruit; wholegrain/brown/wild/undercooked rice; bulgar wheat, couscous, buckwheat; unpeeled/hard potatoes, yam, cassava, taro; high-fibre cereals (Weetabix, Shredded Wheat, Bran Flakes, porridge, muesli, granola); crackers with nuts, seeds, dried fruit. | White or 'best of both' bread/rolls; tacos, tortillas; white rice, pasta, polenta, noodles; peeled/well-cooked white/sweet potatoes, yam, cassava, taro; non-fibrous cereals (Rice Krispies, Cocopops, corn flakes); crackers without nuts, seeds, dried fruit (Digestives, original Ryvita). |
| Meat, Poultry, Fish & Vegetarian Proteins | Steak, gristle-containing, tough or very dry meat, poultry or fish; skins (chicken/fish); bones; pulses and lentils (chickpeas, beans); houmous/hummus; battered, pastry-covered or bread-crumbed proteins. | Well-cooked, non-dry, skinless meat, poultry or fish (pork chop, chicken/fish fillet, mince); eggs (any form); tinned fish (easily chewable bones); tofu, tempeh, textured vegetable protein, mycoprotein (Quorn). Tip: Serve with sauce or gravy for moisture. |
| Dairy & Alternatives | Yoghurt or cheeses with nuts, seeds, dried fruit and granola-like cereals; yoghurts with fruit pulp (e.g., Muller fruit corner). | Yoghurts or cheeses without nuts, seeds and dried fruit; all types of milk (cow's, plant-based like soya or almond). |
| Fruits | Dried fruit (raisins, sultanas, figs); fruit with skin or that is stringy/fibrous (unpeeled apples, oranges with lots of pith, rhubarb, pineapple, figs, dates, coconut); under-ripe fruit (green bananas/mangos); fruit with pips or seeds (raspberries, blackberries). | Peeled fruits (apples, grapes, peaches, plums); oranges and similar fruits without the pith; soft berries (strawberries); bananas, melon, other soft fruits. Tinned, pureed or cooked fruit (without skin, pips or stones). Tip: Tinned or jelly fruit pots are easy snack choices. |
Dietary Considerations for Different Stoma Types
While general healthy eating applies to all, each stoma type has specific considerations due to where it's formed in the digestive tract.
Eating with a Colostomy
A colostomy typically produces soft, formed stools once a day, though this can vary. Fibre is your friend here, as it helps prevent constipation. Ensure your diet includes fruit, vegetables, and wholemeal or wholewheat versions of starchy foods. If wind becomes an issue, consider avoiding gassy drinks, eating too quickly, chewing gum, or smoking, as these can increase swallowed air.
Eating with an Ileostomy
An ileostomy usually results in looser stool, requiring more frequent bag emptying (often four to six times daily). Many people with an ileostomy find that a lower-fibre diet, such as white bread instead of wholewheat, helps to thicken output and make it easier to manage. Root vegetables like carrots are often better tolerated than leafy greens or small, hard vegetables such as sweetcorn.
Hydration is critically important for ileostomy patients to prevent dehydration, as significant fluids and salts are lost. Aim for 1500-2000 ml of fluid daily, increasing this in hot weather or during exercise. Additionally, replenishing lost salt by adding extra to your diet or consuming salty snacks is often recommended, unless you already consume many processed foods.
Eating with a Urostomy
For those with a urostomy, which passes urine, the main dietary focus is on maintaining adequate fluid intake to flush the kidneys. Aim for around 2000 ml of fluid each day. After the initial recovery weeks, most individuals with a urostomy can eat a wide variety of foods without specific dietary restrictions related to the stoma itself.
Gas and Odour
Certain foods are known to produce more gas and odour. These include asparagus, broccoli, Brussels sprouts, cabbage, cauliflower, onions, legumes (like lentils, beans, and peas), nuts, carbonated beverages, and alcohol (especially beer). Eating too quickly, drinking through straws, chewing gum, and smoking can also increase swallowed air, leading to gas. While these foods don't need to be eliminated entirely, being aware of their effects can help you manage symptoms. Yoghurt, buttermilk, cranberry juice, and parsley are sometimes found to help reduce odour.
Diarrhoea or Loose Output
If you experience very loose output, certain foods can help thicken your stool. These include bananas, applesauce, cheese, smooth peanut butter, white rice, and broth. Foods that can contribute to diarrhoea, such as prune juice, raw fruits and vegetables, baked beans, high-sugar foods, spicy foods, and alcohol, may need to be limited. Some people find gelatine-based foods like marshmallows or jelly sweets may help, though evidence for this is limited.
Constipation or Hard Output
If your stoma output is too hard, you can try increasing your intake of warm or hot drinks, cooked fruits and vegetables, raw fruits and vegetables (if tolerated), and fruit juice. Gradually increasing the amount of fibre in your diet can also help to prevent constipation, particularly for colostomy patients.

Alcohol and Your Stoma
Generally, drinking alcohol in moderation is acceptable for people with a stoma, within recommended limits (no more than 14 units a week, spread over several days with alcohol-free days). However, there are a few considerations:
- Colostomy: Gassy alcoholic drinks might increase wind. Stronger drinks like stout can alter stool odour.
- Ileostomy: Alcohol can increase the amount of output and make stool looser, increasing the risk of dehydration. Be mindful of your fluid intake.
- Urostomy: Alcohol acts as a diuretic, meaning you'll pass more urine. This might require more frequent emptying of your urostomy bag, and using a night drainage bag is advisable if you drink alcohol in the evening.
Always be careful not to drink so much that you forget to empty or change your bag.
Debunking Common Stoma Diet Myths
There are many misconceptions about what you can and cannot eat with a stoma. Let's clarify some common ones:
- Myth: Higher fibre foods cause blockage. While it's true that some high-fibre foods like sweetcorn, mushrooms, or peas can increase output or produce more wind, they rarely cause a blockage on their own. Problems usually arise from large servings of high-fibre foods combined with insufficient fluid intake. Moderation is key; there's no need to avoid these foods entirely.
- Myth: Fish and sprouts cause more odour. It's true that certain foods, including fish and sprouts, can produce more odour. However, this odour is typically contained within your ostomy pouch. You usually only notice it when emptying the pouch. Carrying an odour control spray can be helpful if you're concerned about leaving a smell in a public cubicle.
- Myth: Gluten makes you bloated. Gluten, a protein found in flour-based foods like bread and pasta, often gets a bad reputation. Unless you have a diagnosed gluten sensitivity or coeliac disease, it's unlikely to be the sole cause of bloating or excessive wind. If you consistently experience these symptoms after eating gluten, it might be related to irritable bowel syndrome (IBS), which affects a significant portion of the population and can be managed with medical advice. It's generally not recommended to cut gluten from your diet unnecessarily.
Frequently Asked Questions About Stoma Diet
Q: Can I eat spicy foods with a stoma?
A: During the initial recovery period (first 6-8 weeks), it's generally advisable to avoid spicy foods as they can irritate a sensitive gut and potentially lead to increased output or discomfort. After this period, you can gradually reintroduce small amounts of spicy food to see how your body reacts. Many people with established stomas can tolerate moderate spice.
Q: How much fluid should I really drink?
A: The general recommendation is 1.5 to 2 litres (8-10 glasses/3-4 pints) of fluid per day. However, this is especially crucial for individuals with an ileostomy, who lose more fluid and electrolytes. In hot weather, during exercise, or if you have a high stoma output, you will need to increase your fluid intake significantly to prevent dehydration.
Q: What should I do if I suspect a stoma blockage?
A: A stoma blockage can cause symptoms like abdominal pain or cramping, swelling around the stoma, a lack of output, or watery discharge. If you suspect a blockage, it's important to stop eating solid foods, drink plenty of fluids (especially warm drinks), gently massage your abdomen around the stoma, and lie down with your knees bent. If symptoms persist or worsen, or if you have no output for several hours, contact your specialist stoma nurse or GP immediately.
Q: Are there any foods that can change the colour of my stoma output?
A: Yes, certain foods can temporarily change the colour of your stoma output. For example, beetroot can make it appear red, while green leafy vegetables might give it a greenish tint. This is usually harmless and simply reflects the pigments in the food you've eaten.
Seeking Professional Advice
The best person to consult for personalised dietary advice regarding your stoma is your specialist stoma nurse. They can provide tailored information, offer practical tips, and signpost you to reputable resources. While online information is helpful, individual needs vary greatly, and professional guidance ensures your diet supports your unique health requirements and lifestyle.
If you want to read more articles similar to Navigating Your Diet with a Stoma: The UK Guide, you can visit the Automotive category.
