04/09/2012
An abscess is a localised collection of pus within a cavity in the body. It's a common and often uncomfortable condition that arises from an infection, typically bacterial or fungal. While often associated with the skin, abscesses can form in various parts of the body, including internal organs and mucous membranes. Understanding what causes them, how to recognise the signs, and the appropriate course of action is crucial for effective management and recovery.
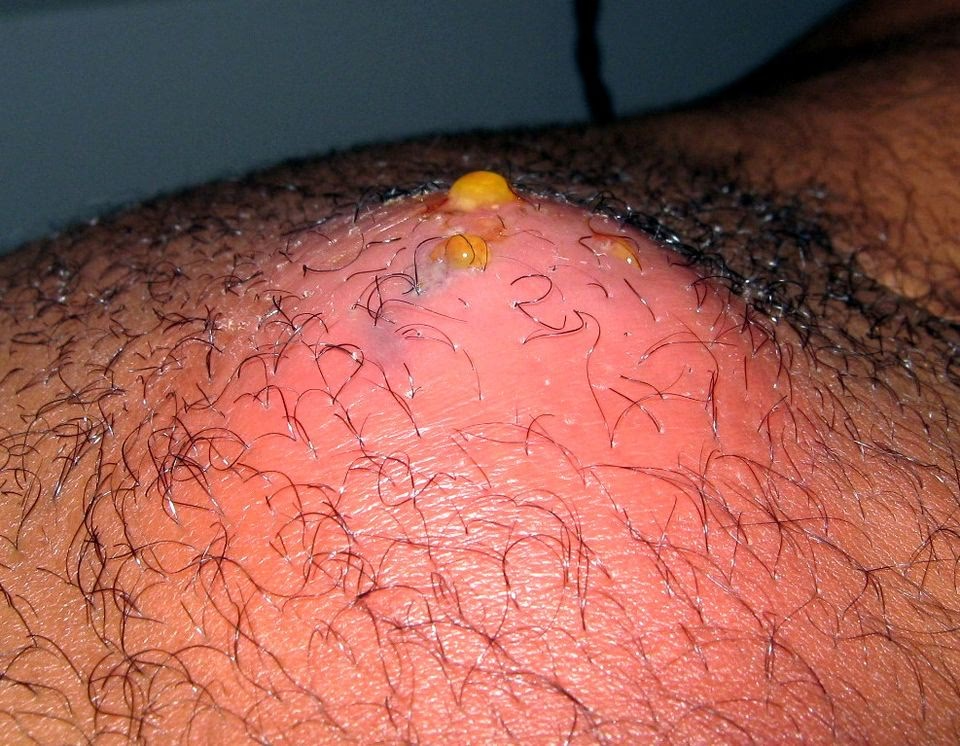
What is an Abscess?
At its core, an abscess is the body's response to an infection. When bacteria or fungi invade tissues, the immune system mobilises white blood cells to fight the invaders. This battle, however, can lead to the death of surrounding cells, both microbial and host. This dead tissue, along with the invading microorganisms and immune cells, forms a thick, often yellowish or greenish, fluid known as pus. This pus then becomes encapsulated, creating a localised pocket or cavity – the abscess.
Abscesses can vary significantly in size, from a small, barely noticeable bump to a large, painful swelling. They can occur anywhere on or within the body. Common locations include the skin (often called boils or furuncles), gums (dental abscesses), and even internal organs like the liver or brain. The formation of an abscess is a sign that the body is trying to contain an infection, preventing it from spreading throughout the bloodstream.
Causes of Abscesses
The primary cause of an abscess is an infection. Several factors can contribute to their development:
- Bacterial Infections: The most common culprits are bacteria, particularly Staphylococcus aureus, which is often found on the skin. These bacteria can enter the body through a break in the skin, such as a cut, scrape, or insect bite.
- Fungal Infections: While less common, certain fungal infections can also lead to abscess formation.
- Parasitic Infections: In some cases, parasitic infections can result in abscesses.
- Foreign Bodies: Splinters, surgical implants, or other foreign objects introduced into the body can also harbour bacteria and lead to an abscess.
- Compromised Immune System: Individuals with weakened immune systems, due to conditions like diabetes, HIV/AIDS, or those undergoing treatments like chemotherapy or corticosteroid therapy, are more susceptible to developing abscesses.
- Poor Hygiene: Inadequate hygiene can create an environment where bacteria can thrive and easily enter the body.
Recognising the Signs and Symptoms
The symptoms of an abscess can vary depending on its location and size, but some common indicators include:
- Pain: Abscesses are often accompanied by throbbing or pulsating pain in the affected area.
- Swelling: The area around the abscess will typically become swollen and raised.
- Redness: The skin over the abscess often appears red and inflamed.
- Warmth: The affected area may feel warm to the touch compared to the surrounding skin.
- Tenderness: The area is usually very sensitive to touch.
- Fever: In some cases, particularly with larger or deeper abscesses, a fever may develop as the body fights the infection.
- Pus Drainage: If the abscess comes to a head, it may rupture and drain pus.
It's important to note that not all skin infections develop into abscesses. However, the presence of these symptoms warrants attention.
When to Seek Medical Advice
While small, superficial skin abscesses might resolve on their own, it is generally advisable to consult a healthcare professional, especially if:
- The abscess is large or very painful.
- The redness and swelling are spreading.
- You have a fever.
- The abscess is located near the eye, in the rectal or genital area, or on the spine.
- You have a weakened immune system or underlying health conditions like diabetes.
- The abscess appears after an injury, as tetanus vaccination status needs to be checked.
- The abscess does not improve after a few days or seems to be getting worse.
Your doctor will be able to accurately diagnose the condition and recommend the most appropriate treatment. Delaying medical attention can lead to complications, including the spread of infection.
Treatment Options for Abscesses
The treatment for an abscess typically depends on its size, location, and severity. The main goals are to drain the pus and eliminate the infection.

1. Drainage
For most abscesses, the primary treatment is to drain the accumulated pus. This is usually a minor surgical procedure performed under local anaesthesia.
- Incision and Drainage (I&D): A doctor will make a small incision in the abscess to allow the pus to drain out. The cavity may be flushed with saline solution to clean it.
- Packing: Sometimes, after drainage, a small amount of gauze or a special dressing may be placed in the wound to keep it open and allow any remaining pus to drain. This dressing is typically changed regularly by a nurse.
It is crucial not to attempt to drain an abscess yourself by squeezing it. This can push the infection deeper into the tissues and potentially cause it to spread.
2. Antibiotics
Antibiotics are not always necessary for treating abscesses, especially if the infection is localised and the abscess can be effectively drained. However, they may be prescribed in certain situations:
- Severe or Widespread Infection: If the infection has spread beyond the localised area or if there are signs of sepsis (a life-threatening response to infection).
- Compromised Immune System: For individuals with weakened immunity, antibiotics help the body fight the infection more effectively.
- High-Risk Locations: Abscesses in certain areas, such as near major blood vessels or internal organs, may warrant antibiotic treatment.
- Recurrent Abscesses: If someone is prone to developing abscesses, antibiotics may be used to prevent future occurrences.
Antibiotics can be administered orally or, in severe cases, intravenously. It is essential to complete the full course of antibiotics as prescribed by your doctor, even if you start to feel better, to ensure the infection is completely eradicated.
3. Wound Care
After drainage, proper wound care is essential to promote healing and prevent re-infection. This typically involves:
- Keeping the wound clean and dry.
- Changing dressings as instructed by your healthcare provider.
- Avoiding pressure or friction on the affected area.
- Monitoring for any signs of worsening infection.
Natural and Home Care Approaches
While medical intervention is often necessary, some natural remedies can be used as complementary approaches, particularly for minor skin abscesses, under the guidance of a healthcare professional.
- Warm Compresses: Applying warm compresses to the abscess can help to promote drainage by increasing blood flow to the area and encouraging the pus to come to a head. This should be done several times a day.
- Aromatherapy: Certain essential oils possess antimicrobial and anti-inflammatory properties. Oils like Tea Tree, Palmarosa, Geranium, or Thyme (linalool) are often recommended. They can be applied topically, either undiluted (if the skin tolerates it) or diluted in a carrier oil such as olive, macadamia, or sweet almond oil. Follow specific dilution guidelines and apply morning and evening. If no improvement is seen within a few days, consult a doctor.
Important Note: If an abscess is already collected (i.e., a significant pocket of pus has formed), self-treatment with natural remedies is not recommended. In such cases, professional medical drainage is essential.
Preventing Abscesses
While not all abscesses can be prevented, good hygiene practices can significantly reduce the risk:
- Keep Skin Clean: Wash your skin regularly with soap and water, especially after activities that may lead to cuts or abrasions.
- Treat Wounds Promptly: Clean and dress any cuts, scrapes, or insect bites immediately to prevent bacteria from entering.
- Avoid Sharing Personal Items: Do not share towels, razors, or other personal items that can transmit bacteria.
- Maintain a Healthy Immune System: A balanced diet, regular exercise, and adequate sleep contribute to a strong immune system, making you less susceptible to infections.
- Manage Underlying Health Conditions: If you have conditions like diabetes, proper management can help prevent complications, including infections.
Frequently Asked Questions
Q1: Can an abscess go away on its own?
A: Small, superficial abscesses might resolve on their own, but larger or deeper ones often require medical intervention, such as drainage, to heal properly and prevent complications.

Q2: Is it safe to pop an abscess?
A: No, it is strongly advised not to pop or squeeze an abscess. This can push the infection deeper, increase pain, and potentially lead to a more severe infection or spread.
Q3: How long does it take for an abscess to heal after drainage?
A: Healing time varies depending on the size and location of the abscess, as well as the individual's health. Typically, it can take anywhere from a few days to a couple of weeks for the wound to heal completely after drainage and appropriate care.
Q4: Can abscesses recur?
A: Yes, abscesses can recur, especially if the underlying cause or contributing factors are not addressed. Factors like a weakened immune system or repeated exposure to bacteria can increase the risk of recurrence.
Q5: What is the difference between an abscess and a boil?
A: A boil (or furuncle) is a type of abscess that specifically affects a hair follicle and the surrounding tissue, typically on the skin. An abscess is a more general term for a collection of pus anywhere in the body.
Conclusion
Abscesses are common infections that, while often painful and uncomfortable, are generally treatable. Understanding the causes, recognising the symptoms, and seeking timely medical advice are key to effective management. Proper wound care and preventive measures can also play a significant role in healing and avoiding future occurrences. Always consult with a healthcare professional for diagnosis and treatment recommendations.
If you want to read more articles similar to Understanding and Managing Abscesses, you can visit the Automotive category.
