12/10/2016
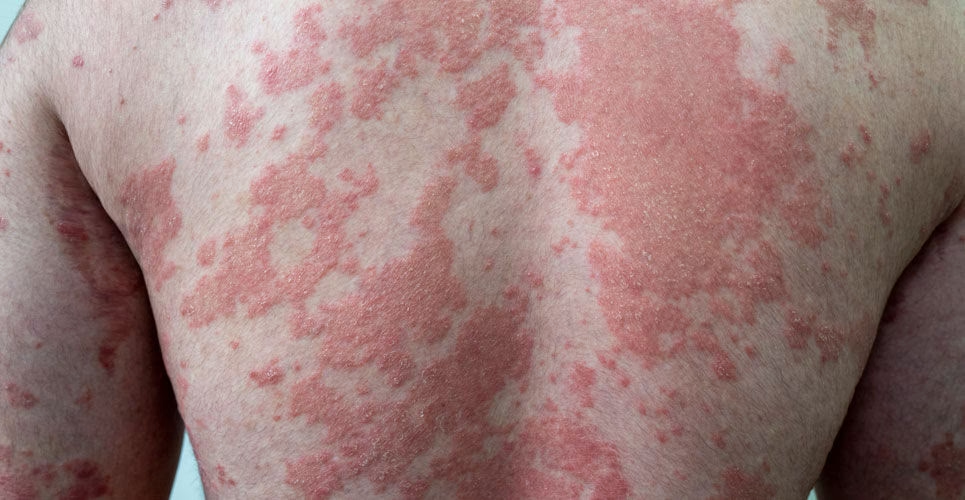
Psoriasis is a chronic, immune-mediated inflammatory skin condition affecting millions across the UK. It manifests as red, scaly plaques on the skin, a result of skin cells multiplying too quickly. While there's no cure, a variety of treatments can effectively manage symptoms and improve quality of life. Among the first-line options often prescribed by healthcare professionals are topical vitamin D treatments, which harness the power of this vital 'sunshine vitamin' to restore skin health.
These treatments, designed for direct application to the skin, play a crucial role in slowing down the excessive production of skin cells and exerting an important anti-inflammatory effect. Unlike oral vitamin D supplements, which are taken by mouth for general health and bone metabolism, topical vitamin D acts locally to address the specific cellular dysregulation seen in psoriatic lesions. This targeted approach makes them an invaluable part of a comprehensive psoriasis management plan.
- Understanding How Topical Vitamin D Works
- Forms and Availability of Topical Vitamin D in the UK
- When and How to Use Topical Vitamin D Treatments
- The Link Between Vitamin D Deficiency and Psoriasis
- Vitamin D and Psoriatic Arthritis
- Treating Scalp Psoriasis with Topical Vitamin D
- Frequently Asked Questions (FAQs)
- Is topical vitamin D the same as vitamin D supplements I take orally?
- How long does it take for topical vitamin D treatments to work?
- Can I buy topical vitamin D treatments without a prescription in the UK?
- Does having a vitamin D deficiency cause psoriasis?
- Can oral vitamin D supplements cure my psoriasis?
- Conclusion
Understanding How Topical Vitamin D Works
At the heart of psoriasis is the rapid turnover of skin cells, specifically keratinocytes. Normally, these cells mature and shed over a period of about 28 days. In psoriasis, this process accelerates dramatically, sometimes occurring in as little as 3-4 days, leading to the characteristic thick, scaly plaques. Topical vitamin D derivatives work by encouraging the normal growth and differentiation of these skin cells, effectively putting the brakes on their runaway production.
The active form of vitamin D, calcitriol, and its synthetic analogues (such as calcipotriol, tacalcitol, and maxacalcitol) bind to vitamin D receptors (VDRs) found in various cells throughout the body, including keratinocytes in the skin. This binding initiates a series of genetic mechanisms that inhibit keratinocyte proliferation and promote their normal differentiation. Furthermore, vitamin D has significant immunomodulatory properties. It can down-regulate the expression and production of pro-inflammatory cytokines like TNF-α, IL-1β, IL-6, and IL-8, which are key drivers of inflammation in psoriatic lesions. By modulating the immune response and reducing inflammation, topical vitamin D treatments help to alleviate the redness, itching, and scaling associated with psoriasis.
Forms and Availability of Topical Vitamin D in the UK
Topical vitamin D treatments come in various formulations to suit different body areas and patient preferences. These include:
- Ointments: Often preferred for drier, thicker plaques, providing a more occlusive barrier.
- Gels: Lighter, less greasy, suitable for hairy areas like the scalp.
- Lotions: Spread easily over larger body areas.
- Foams: Can be particularly useful for scalp psoriasis due to their ease of application.
In the United Kingdom, most topical vitamin D treatments are available only on prescription from a GP or dermatologist. However, there is one notable exception: Dovonex ointment (which contains calcipotriol) can sometimes be purchased directly from a pharmacist without a prescription, provided you have a confirmed diagnosis of psoriasis. It's worth noting that the cost of Dovonex bought over the counter is typically significantly higher than if it's obtained via an NHS prescription.

When and How to Use Topical Vitamin D Treatments
Topical vitamin D treatments are versatile and can be used in several ways depending on the severity and location of your psoriasis:
- Monotherapy: For mild to moderate psoriasis, they may be used as the sole treatment.
- Combination Therapy: They are often used in conjunction with topical steroid treatments. This combination can be particularly effective, as steroids provide rapid anti-inflammatory action, while vitamin D derivatives work on long-term cell normalisation. Combining therapies can also help to reduce the frequency and amount of steroid use, minimising potential side effects like skin thinning.
- Rotation Therapy: Some individuals may alternate between topical vitamin D and other treatments to prevent tachyphylaxis (reduced response over time) to certain medications or to manage side effects.
It is crucial to follow your doctor's instructions regarding application frequency and duration. Typically, a review appointment is recommended approximately four weeks after starting a new topical treatment (or two weeks for children) to assess its effectiveness and address any concerns. Like many topical treatments, it can take several weeks of consistent use for topical vitamin D to become fully effective. Patience and adherence to the treatment plan are key to achieving optimal results.
One significant advantage of topical vitamin D analogues is that they do not exhibit tachyphylaxis, unlike corticosteroids. This means their effectiveness does not diminish with prolonged use, allowing for continuous application without serious adverse side effects. This makes them particularly helpful for hard-to-treat areas such as the face or inguinal regions, which are sensitive to steroid-induced atrophy. They are also considered safe and effective for treating psoriatic skin lesions in children and the elderly.
The Link Between Vitamin D Deficiency and Psoriasis
Research has established a link between vitamin D deficiencies and psoriasis. While a deficiency doesn't directly *cause* psoriasis, it may impair the body's ability to maintain healthy skin, potentially increasing the frequency or severity of flares. This connection underscores the broader importance of adequate vitamin D levels, not just for bone health but for immune function and skin integrity.
The epidermis, the outermost layer of the skin, is the natural site for vitamin D synthesis when exposed to UVB sunlight. Many individuals with psoriasis may have lower vitamin D levels, possibly due to avoiding sun exposure (to prevent sunburn or due to concerns about skin cancer) or because the disease itself impacts vitamin D metabolism. Checking your vitamin D levels through a blood test is a good idea, as maintaining levels above 30 nanograms per milliliter (ng/mL) is generally recommended for overall health.

Beyond Topical: Oral Vitamin D and Dietary Sources
While topical vitamin D is applied directly to psoriatic lesions, oral vitamin D supplements and diet can contribute to overall vitamin D status, which may indirectly support skin health. However, it's vital to distinguish their roles:
Oral Supplements: Available in pill or liquid forms, these are easy to incorporate into a daily routine. Healthcare professionals often recommend 400 to 1,000 International Units (IU) per day, though higher doses may be prescribed for deficiencies. While raising overall vitamin D levels can have broad health benefits and potentially reduce inflammatory responses, recent meta-analyses have indicated that oral vitamin D supplementation alone may not significantly improve the Psoriasis Area and Severity Index (PASI) score, a common measure of psoriasis severity. This suggests that while addressing a deficiency is important for general health, it may not directly lead to a dramatic reduction in skin lesions for all patients.
Foods Rich in Vitamin D: Increasing dietary intake of vitamin D can also help. Few foods naturally contain significant amounts, but options include:
- Fatty fish (salmon, tuna, mackerel, herring)
- Cod liver oil
- Egg yolks
- Cheese
- Fortified foods (some cereals, orange juices, dairy products)
Phototherapy: Controlled exposure to sunlight or the use of sun lamps/light boxes (phototherapy) can also increase the body's natural vitamin D production. This treatment should be approached with caution and under medical supervision due to the risk of skin cancer with excessive sun exposure.
Vitamin D and Psoriatic Arthritis
Psoriasis is increasingly recognised as a systemic pathology, often associated with other conditions like psoriatic arthritis, obesity, and metabolic syndrome. Psoriatic arthritis is an inflammatory condition affecting the joints, tendons, and ligaments, and it occurs in up to 30% of people with psoriasis. Given vitamin D's known role in regulating calcium-phosphorus homeostasis and its emerging role as a key modulator of immune and inflammatory mechanisms, its potential involvement in psoriatic arthritis has been explored.
While topical vitamin D is a cornerstone for skin lesions, the effectiveness of oral vitamin D supplementation as an adjunctive treatment option for psoriatic arthritis patients remains somewhat controversial in clinical trials. Some studies suggest an inverse link between serum vitamin D levels and disease activity in psoriatic arthritis, implying that lower vitamin D levels might be associated with more severe joint disease. However, consistent evidence demonstrating a direct beneficial effect of oral supplementation on joint symptoms (similar to its established role in skin) is still developing. Nutritionists often highlight the broader benefits of vitamin D supplementation for preventing comorbidities associated with psoriasis, such as hypertension and metabolic syndrome, through its anti-inflammatory effects.

Comparison of Topical Psoriasis Treatments
Here's a brief comparison between topical Vitamin D analogues and topical corticosteroids, which are often used in conjunction or rotation:
| Feature | Topical Vitamin D Analogues | Topical Corticosteroids |
|---|---|---|
| Mechanism of Action | Slows cell proliferation, promotes normal differentiation, anti-inflammatory. | Potent anti-inflammatory, immunosuppressive, vasoconstrictive. |
| Onset of Action | Takes several weeks for full effect. | Often rapid, noticeable improvement within days. |
| Long-Term Use | Can be used indefinitely without tachyphylaxis or significant side effects. | Risk of tachyphylaxis, skin thinning, stretch marks, and other side effects with prolonged use. |
| Suitability for Sensitive Areas | Good for face, skin folds (groin, armpits). | Use with caution and for limited durations on sensitive areas due to side effect risk. |
| Availability (UK) | Mostly prescription-only (Dovonex ointment sometimes OTC). | Prescription-only, varying potencies. |
Treating Scalp Psoriasis with Topical Vitamin D
Scalp psoriasis can be particularly challenging to treat due to hair and the sensitive nature of the scalp. For patients with mild to moderate scalp psoriasis who cannot use or prefer to avoid topical corticosteroids, topical vitamin D or its analogues are often recommended as a primary treatment. These formulations, especially gels or foams, are designed to penetrate the hair and reach the scalp effectively. If topical vitamin D treatment for up to 8 weeks does not yield a satisfactory response, a coal tar preparation may be offered, or the patient may be referred to a specialist for further options.
Frequently Asked Questions (FAQs)
Is topical vitamin D the same as vitamin D supplements I take orally?
No, they are distinct. Topical vitamin D treatments are applied directly to the skin to act locally on psoriatic lesions by slowing skin cell growth and reducing inflammation. Oral vitamin D supplements are taken by mouth for systemic health benefits, primarily bone health and overall immune function, and their direct impact on psoriasis skin lesions is less consistent in studies.
How long does it take for topical vitamin D treatments to work?
It can take several weeks of consistent use for topical vitamin D treatments to become fully effective. Your doctor will likely schedule a review appointment a few weeks after you start treatment to assess progress.
Can I buy topical vitamin D treatments without a prescription in the UK?
Most topical vitamin D treatments require a prescription from a doctor. However, Dovonex ointment (calcipotriol) can sometimes be purchased over the counter from certain pharmacies if you have a confirmed psoriasis diagnosis, though it may be significantly more expensive than with a prescription.

Does having a vitamin D deficiency cause psoriasis?
While research shows a link between vitamin D deficiency and psoriasis, a deficiency isn't considered a direct cause of the condition. However, low vitamin D levels may affect the body's ability to maintain healthy skin and could potentially lead to more frequent or severe psoriasis flares.
Can oral vitamin D supplements cure my psoriasis?
No, oral vitamin D supplements are not a cure for psoriasis. While maintaining healthy vitamin D levels is beneficial for overall well-being and immune health, and may indirectly support skin health, large-scale studies have not consistently shown that oral supplementation significantly reduces the severity of psoriasis plaques (measured by PASI scores).
Conclusion
Topical vitamin D treatments are a cornerstone in the management of psoriasis in the UK, offering an effective and generally well-tolerated option for many individuals. By directly influencing skin cell growth and calming inflammation, these formulations help to restore skin health and reduce the characteristic plaques. While oral vitamin D supplements are important for general health and addressing deficiencies, their role in directly improving skin lesions is nuanced. Always consult with your GP or dermatologist to determine the most appropriate treatment plan for your specific type and severity of psoriasis, ensuring you make the most of the 'sunshine vitamin' for healthier skin.
If you want to read more articles similar to Topical Vitamin D for Psoriasis: A UK Guide, you can visit the Automotive category.
