17/09/2024
Tooth pain is a universal experience, often immediately associated with the dreaded cavity. While a hole in your tooth is indeed a common cause, the reality is far more intricate. The oral cavity is a complex network of nerves, muscles, and bone, meaning discomfort can stem from a myriad of sources, many of which are entirely unrelated to tooth decay. Understanding these alternative causes is crucial for accurate diagnosis and effective relief, especially when no cavity is apparent, or when pain lingers after a trip to the dentist.
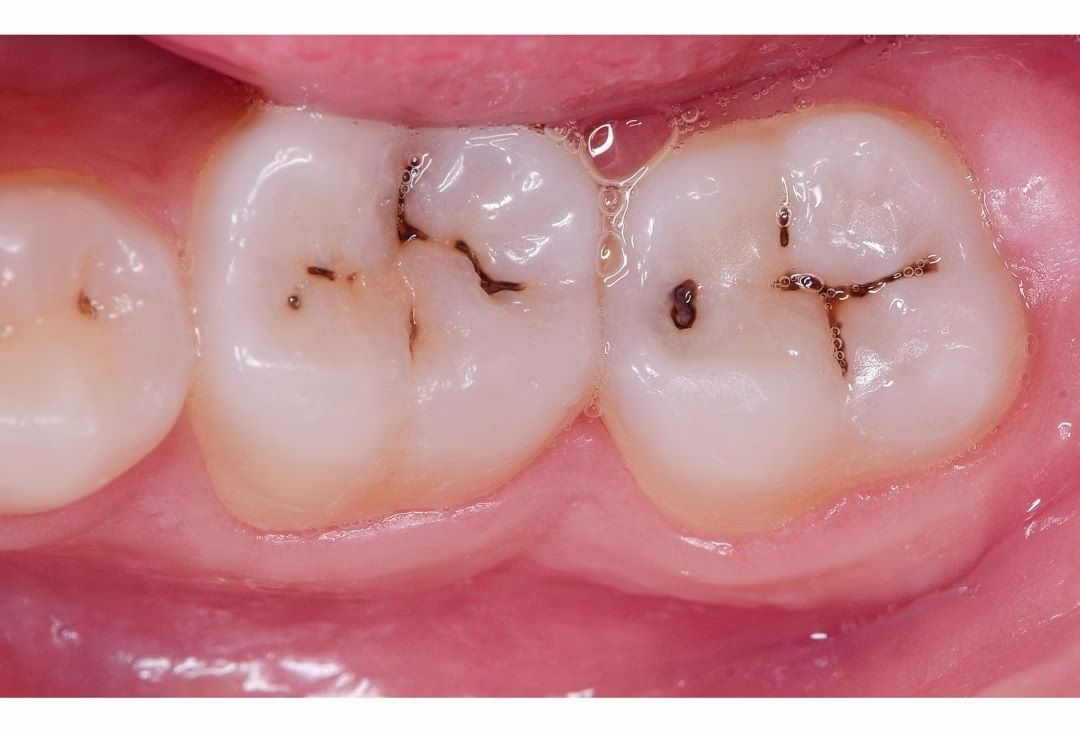
This comprehensive guide delves into the less obvious reasons for toothaches, exploring everything from neighbouring anatomical structures to underlying dental habits and post-treatment sensitivities. By shedding light on these often-overlooked culprits, we aim to equip you with the knowledge needed to pinpoint the potential source of your discomfort and take the right steps towards regaining your oral comfort.
- Beyond the Cavity: Surprising Causes of Tooth Pain
- Sinusitis: The Unsuspected Culprit
- Jaw Pain and Temporomandibular Disorders (TMD)
- Impacted Wisdom Teeth: A Growing Problem
- Gum Disease: The Silent Destroyer
- Dental Wear and Tear
- Tooth Trauma and Fractures
- Receding Gums: Exposed Sensitivity
- Abscesses: Pockets of Infection
- Referred Pain: When the Source Isn't the Tooth
- Understanding Pain After a Dental Visit
- When to See a Dentist (or Doctor)
- Prevention is Key: Maintaining Optimal Oral Health
- Frequently Asked Questions (FAQs)
- Q: Can a cold or flu cause tooth pain?
- Q: Why does my tooth hurt when I bite down, but there's no cavity?
- Q: Is tooth sensitivity after a dental filling normal?
- Q: How can I tell if my tooth pain is from a sinus infection versus a dental problem?
- Q: What's the difference between gum pain and tooth pain?
Beyond the Cavity: Surprising Causes of Tooth Pain
When your dentist confirms there’s no decay, yet your tooth continues to ache, it can be perplexing. However, several conditions can mimic a toothache, making it feel as though the problem lies squarely within a tooth.
Sinusitis: The Unsuspected Culprit
One of the most common non-dental causes of tooth pain is a sinus infection, or sinusitis. Your maxillary sinuses, located just above your upper back teeth, can become inflamed and filled with fluid due to infection or allergies. The pressure from this inflammation can press down on the roots of your upper teeth, leading to a dull, aching pain. This discomfort typically affects multiple upper teeth on both sides and is often accompanied by nasal congestion, facial tenderness around the cheeks and eyes, and a feeling of fullness in the face. If your toothache worsens when you bend over or lie down, and you have cold or allergy symptoms, sinusitis is a strong possibility. Consulting your general practitioner may be beneficial for diagnosis and treatment of the underlying sinus issue.
Jaw Pain and Temporomandibular Disorders (TMD)
Pain that feels like it’s emanating from your teeth but is actually originating in your jaw joint is a hallmark of temporomandibular disorders, commonly referred to as TMJ. The temporomandibular joint connects your jawbone to your skull and can cause significant discomfort if it’s injured, inflamed, or misaligned. Symptoms of TMD often include pain or tenderness in the jaw, face, neck, and shoulders, as well as difficulty chewing, a clicking or popping sound when opening or closing your mouth, and even locked jaw. Causes can range from direct injury or trauma to the jaw, to chronic teeth grinding (bruxism) or various forms of arthritis affecting the joint. If the pain is more widespread in your jaw and radiates, rather than being confined to a single tooth, TMD should be considered.
Impacted Wisdom Teeth: A Growing Problem
For those who still have their wisdom teeth (third molars), an impacted wisdom tooth can be a significant source of pain. Impaction occurs when there isn't enough space in the back of your mouth for these teeth to emerge properly, causing them to grow at an angle, press against neighbouring teeth, or remain trapped beneath the gums. This can lead to persistent jaw pain, swelling, tenderness, and sometimes even infection. The pain often feels like a deep ache in the back of the jaw, occasionally radiating towards the ear or throat. Dental x-rays are crucial for diagnosing impacted wisdom teeth, and extraction is frequently recommended to alleviate the pain and prevent further complications.
Gum Disease: The Silent Destroyer
While not a tooth issue directly, gum disease can cause pain that the body struggles to differentiate from tooth pain. Gingivitis, the mildest form, causes gums to become red, swollen, and prone to bleeding. Left untreated, it can progress to periodontitis, a more severe infection where pockets form in the gums, leading to bone loss and potential tooth mobility. The inflammation and infection associated with gum disease can cause a generalised ache or sensitivity that might be mistaken for a toothache. Factors like poor oral hygiene, smoking, certain medications, and underlying health conditions such as diabetes can increase the risk of gum disease. Regular brushing, flossing, and professional dental cleanings are vital for prevention and management.
Dental Wear and Tear
Our teeth are incredibly strong, but they are not impervious to wear. Chronic habits or conditions can erode enamel and expose the sensitive underlying dentin, leading to pain. This includes:
- Bruxism (Teeth Grinding/Clenching): Often occurring unconsciously, especially during sleep, bruxism puts immense pressure on teeth, leading to cracks, fractures, and widespread sensitivity or pain. It can also contribute to headaches, earaches, and stiff facial muscles.
- Aggressive Brushing: Brushing too hard or using a hard-bristled toothbrush can wear away enamel and gum tissue, exposing sensitive root surfaces.
- Acid Erosion: Frequent consumption of highly acidic foods and drinks (like citrus fruits or fizzy drinks), or conditions like chronic acid reflux (GERD) or frequent vomiting, can dissolve tooth enamel over time, making teeth more susceptible to pain.
These forms of wear can cause sharp, fleeting pain when exposed to hot, cold, or sweet stimuli, or a dull, persistent ache.
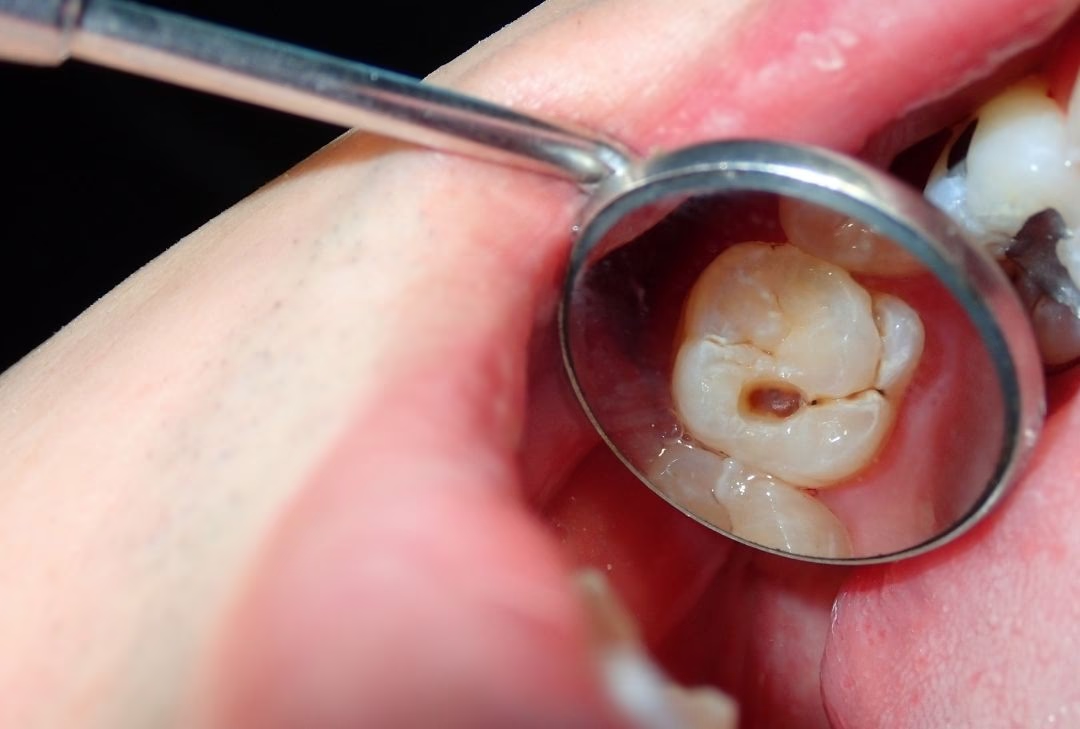
Tooth Trauma and Fractures
Even if you haven't had an obvious accident, trauma to a tooth can cause pain. This can be from a minor impact, biting down on something hard, or even vigorous clenching. Inside each tooth are delicate arteries, veins, and nerves. Injury can lead to swelling within the rigid structure of the tooth, causing pressure and pain. Furthermore, a crack or fracture in a tooth, which might not always be visible, can cause significant pain, especially when biting down. If the crack extends into the pulp, it can lead to infection. Depending on the severity, treatment can range from a simple bonding to a cap, crown, or even an implant. Using a mouthguard during contact sports or if you grind your teeth can help prevent such injuries.
Receding Gums: Exposed Sensitivity
Gum recession occurs when the gum tissue pulls back, exposing the root surface of the tooth. Unlike the crown, the root is not protected by enamel and contains thousands of tiny tubules leading to the tooth's nerve. When exposed, these tubules allow hot, cold, or acidic stimuli to reach the nerve, causing sharp, temporary pain. Factors contributing to gum recession include aggressive brushing, periodontal disease, smoking, and genetic predisposition. While recession cannot be reversed without surgical intervention, using desensitising toothpaste and adopting gentler brushing techniques can help manage the sensitivity.
Abscesses: Pockets of Infection
An abscess is a pocket of pus caused by a bacterial infection, typically forming at the tip of the tooth root (periapical abscess) or in the gums (periodontal abscess). While often a result of untreated tooth decay, an abscess can also stem from a cracked tooth, severe gum disease, or even food particles jammed deep between teeth, leading to inflammation and infection. Symptoms include severe, throbbing pain, swelling in the gum or face, fever, and a bad taste in the mouth. An abscess requires immediate dental attention as the infection can spread and lead to serious health complications if left untreated.
Referred Pain: When the Source Isn't the Tooth
Sometimes, the pain you feel in your tooth isn't actually coming from the tooth itself. This phenomenon is known as referred pain, where discomfort originates in one area but is perceived in another. As mentioned with TMD and sinusitis, the complex nerve pathways in the head and neck can confuse the brain about the pain's true origin. Pain from muscle tension in the face or neck, ear infections, or even issues with cervical vertebrae can manifest as a toothache. This type of pain might be accompanied by other symptoms like headaches, earaches, or stiffness in the neck or jaw, further indicating a non-dental source.
Understanding Pain After a Dental Visit
It can be disheartening to experience tooth pain shortly after a dental appointment, but it's often a normal part of the healing process or a sign of an issue that needs attention.
Post-Orthodontic Discomfort
If you're undergoing orthodontic treatment, such as braces or clear aligners, experiencing pain after an adjustment is very common. Orthodontic work involves carefully controlled forces applied to your teeth to gradually move them into new positions. This pressure affects the ligaments and bone surrounding the teeth, leading to temporary inflammation and discomfort. The pain typically subsides within a few days. Over-the-counter anti-inflammatory medications can help manage this discomfort, but if the pain is severe or persistent, it's essential to discuss it with your orthodontist.
Filling Woes: Lost or Damaged Fillings
A dental filling is designed to repair a tooth damaged by decay. However, fillings can sometimes fall out or become damaged due to excessive biting force, material breakdown over time, or new decay forming around or underneath the existing filling. When a filling is lost, the newly exposed tooth structure can become highly sensitive to temperature changes and pressure. Food can also get packed into the void, causing discomfort and pressure. If you suspect a lost or damaged filling, contact your dentist promptly to prevent further decay or damage to the tooth.
General Sensitivity After Procedures
It's common to experience some degree of sensitivity or mild pain after routine dental procedures like fillings, deep cleanings, or even professional whitening. This is because the tooth's nerve can be temporarily irritated during the procedure. Sensitivity to hot, cold, or biting usually resolves within a few days or weeks. If the pain is severe, lingers for an extended period, or worsens, it could indicate a more serious issue such as a high filling (where the filling is slightly too tall, causing uneven bite pressure), pulp inflammation, or even a micro-fracture. Always communicate persistent or worsening pain to your dental professional.

When to See a Dentist (or Doctor)
Given the wide array of potential causes for tooth pain, professional diagnosis is paramount. While some discomfort might resolve on its own, ignoring persistent or severe pain can lead to more serious complications. It's always advisable to consult a dental professional if you experience:
- Pain that lasts for more than a day or two.
- Severe pain that interferes with eating, sleeping, or daily activities.
- Swelling in your gums, face, or jaw.
- Fever or general malaise accompanying the tooth pain.
- A foul taste in your mouth, which could indicate an infection.
- Pain after a dental procedure that is severe, worsening, or doesn't subside within a reasonable timeframe.
During your visit, your dentist will conduct a thorough examination, which may include x-rays, visual inspection for discolouration or cracks, and tests to identify sensitivity or pain points. They may also ask about your medical history and lifestyle habits to uncover potential non-dental causes.
Prevention is Key: Maintaining Optimal Oral Health
While not all causes of tooth pain are preventable, many can be avoided or mitigated with good oral hygiene practices and lifestyle adjustments:
- Brush Regularly: Brush your teeth twice a day for two minutes with a fluoride toothpaste.
- Floss Daily: Clean between your teeth daily to remove plaque and food particles that brushing alone can't reach.
- Regular Dental Check-ups: Visit your dentist for routine check-ups and professional cleanings, typically every six months. This allows early detection and treatment of issues before they become painful.
- Avoid Tobacco Products: Smoking and smokeless tobacco significantly increase the risk of gum disease and other oral health problems.
- Use a Mouthguard: If you grind or clench your teeth (bruxism), a custom-fitted mouthguard worn at night can protect your teeth from excessive wear and fracture. Similarly, use a mouthguard during contact sports.
- Manage Stress: Stress is a common trigger for bruxism. Incorporate relaxation techniques like yoga, meditation, or deep breathing into your routine.
- Be Mindful of Your Diet: Limit sugary and acidic foods and drinks, which can erode enamel and contribute to decay.
- Stay Hydrated: Drinking plenty of water helps wash away food particles and neutralise acids.
Frequently Asked Questions (FAQs)
Q: Can a cold or flu cause tooth pain?
A: Yes, absolutely. The pressure from inflamed sinuses during a cold, flu, or allergy flare-up can cause pain in your upper teeth, mimicking a toothache. This is often accompanied by nasal congestion and facial pressure.
Q: Why does my tooth hurt when I bite down, but there's no cavity?
A: This could be due to several reasons, including a cracked tooth (which might not be visible), a loose or damaged filling, an issue with your bite (occlusal trauma), or even early stages of gum disease. TMJ disorders can also cause pain when chewing.
Q: Is tooth sensitivity after a dental filling normal?
A: Mild sensitivity to hot, cold, or pressure after a filling is common and usually subsides within a few days to a couple of weeks as the tooth heals. However, if the pain is severe, constant, or worsens, you should contact your dentist as it could indicate a deeper issue or an uneven bite.
Q: How can I tell if my tooth pain is from a sinus infection versus a dental problem?
A: Sinus-related tooth pain typically affects multiple upper teeth, often on both sides of your face, and is usually accompanied by nasal congestion, facial tenderness, or pressure. It might also worsen when you lean forward. Dental pain, especially from a cavity or fracture, is often more localised to a single tooth and might be sharp or throbbing.
Q: What's the difference between gum pain and tooth pain?
A: It can be challenging to differentiate, as pain from the gums can radiate and feel like it's coming from a tooth. However, gum pain often involves visible signs like redness, swelling, bleeding, or tenderness of the gum tissue itself. Tooth pain is more likely to be sharp, throbbing, or sensitive to temperature directly from the tooth structure.
| Symptom | Possible Cause(s) | Key Indicators |
|---|---|---|
| Dull, aching pain in upper teeth (multiple) | Sinusitis | Accompanied by nasal congestion, facial pressure; worsens when bending over. |
| Jaw pain, clicking/popping, difficulty chewing | TMJ Disorders | Pain radiates to face, neck, ears; jaw stiffness, headaches. |
| Sharp pain when biting down, often fleeting | Cracked Tooth, Lost Filling, Bruxism | Can be hard to pinpoint; pain specific to biting force. |
| Sensitivity to hot/cold, especially at gum line | Receding Gums, Dental Wear, Aggressive Brushing | Pain is usually sharp and temporary; visible gum recession. |
| Throbbing pain, swelling, fever, bad taste | Abscess, Severe Gum Infection | Localised swelling, pus, systemic symptoms. |
| Generalised ache in back of jaw | Impacted Wisdom Tooth | Pain from erupting or trapped molar; often in late teens/early twenties. |
Understanding the varied origins of tooth pain is the first step towards finding relief. While cavities are a common culprit, the body's intricate systems mean that discomfort can arise from numerous other sources, both dental and non-dental. If you are experiencing persistent or severe tooth pain, do not hesitate to seek professional advice. A timely and accurate diagnosis from your dentist or doctor is essential for effective treatment and maintaining your overall oral health and well-being.
If you want to read more articles similar to Beyond the Cavity: Unravelling Tooth Pain, you can visit the Automotive category.
