16/10/2012
Calf muscle pain is a common ailment that can range from a mild inconvenience to a debilitating condition. While often attributed to strenuous exercise or simple muscle fatigue, persistent or severe calf pain can sometimes signal a more serious underlying health issue. It's crucial to understand the potential causes, recognise the warning signs, and know when to seek professional medical advice. This comprehensive guide will delve into the various reasons behind calf pain, focusing on differentiating between benign causes and potentially life-threatening conditions like Deep Vein Thrombosis (DVT).
When to Seek Immediate Medical Attention (Go to the ER)
While most calf pain is not an emergency, certain symptoms warrant an immediate visit to the nearest emergency room. Ignoring these could have severe consequences. If you experience calf pain accompanied by any of the following, do not delay seeking help:
- Swelling, redness, or discolouration (e.g., bluish or unusually pale skin) and/or warmth in the calf or any part of the leg.
- Severe dehydration, indicated by no urination, inability to keep fluids down, confusion, or persistent vomiting/diarrhoea.
- Difficulty or inability to walk or move your leg, especially after significant leg trauma (e.g., from an accident or sports injury).
- Open, non-healing sores or unusual skin discolouration on the leg, feet, or toes.
- Sudden, severe pain described as being struck violently in the back of the leg, sometimes with an audible "pop."
- Lower back or leg pain accompanied by sudden weakness, loss of sensation, or issues with bladder/bowel control (retention or incontinence).
When to Contact Your Healthcare Provider
Even if your calf pain isn't an emergency, it's important to consult a healthcare professional if the pain persists despite home remedies. You might have an underlying condition affecting your nerves, hormones, or joints that requires specific treatment. Contact your doctor if you experience calf pain along with:
- Fever, night sweats, or unintentional weight loss.
- A weakened or suppressed immune system.
- You are taking blood-thinning medication or any medication known to cause muscle cramps as a side effect.
- A history of or current cancer diagnosis.
- You are aged 60 or over.
Common Causes of Acute Calf Pain and Their Treatments
Calf pain can stem from various issues affecting the muscles, tendons, nerves, and blood vessels in the lower leg. Here are some of the most frequent culprits:
Muscle Cramps
Calf cramps are sudden, involuntary, and often painful contractions of the calf muscles. They can cause stiffness and a visible knotting of the muscle, with lingering stiffness for days. Common causes include:
- Nocturnal leg cramps (occurring at night).
- Exercise-related cramps due to muscle fatigue or electrolyte imbalances (e.g., low potassium or magnesium).
- Certain medications, such as diuretics.
Treatment: For common cramps, stretching the calf muscle (pulling toes and foot upwards) and staying hydrated, potentially with electrolyte supplements for exercise-related cramps, are often effective. If cramps are persistent or severe, it may indicate a more serious underlying condition.
Calf Strain
A calf strain is an injury where the muscle fibres or tendons at the back of the lower leg are torn. This is common in athletes involved in activities like running, jumping, football, soccer, tennis, or basketball. The pain can be sudden or gradual, feeling tight, cramping, gripping, sharp, or sore, and may be accompanied by swelling and weakness.
Treatment: The RICE protocol is the standard approach:
- Rest: Avoid activities that cause pain until you can walk without a limp. A walking boot or crutches may be necessary.
- Ice: Apply ice to the calf for 10-20 minutes at a time, four times daily, to reduce swelling.
- Compression: Use a compression sleeve to help manage swelling.
- Elevation: Keep the affected leg raised above heart level to minimise swelling.
Over-the-counter pain relievers like paracetamol (acetaminophen) or NSAIDs (ibuprofen, naproxen) can help manage pain and inflammation. Physical therapy or home exercises are crucial for regaining strength and movement. Surgery is rarely required and reserved for severe tears.
Achilles Tendonitis
This condition involves inflammation or irritation of the Achilles tendon, the strong band connecting calf muscles to the heel bone, typically due to overuse. Symptoms include soreness and stiffness along the tendon and the back of the leg, often worse after activity and in the morning. Other signs include thickening of the tendon, pain that worsens the day after exercise, and pain at the back of the heel when wearing shoes.
Treatment:
- Resting the leg and avoiding aggravating activities.
- Icing the lower leg for 15-minute intervals every six hours for the first 48 hours.
- Taking NSAIDs for pain and inflammation.
- Wearing supportive footwear or using heel lifts.
- Physical therapy for strengthening and massage.
Varicose Veins
These are enlarged, twisted superficial veins, commonly seen on the legs, including the calves. They are usually harmless but can cause a heavy, burning, tired, or aching sensation, often worse after prolonged standing or sitting. Itching and skin discolouration may also occur.
Treatment: Focuses on symptom relief and preventing progression:
- Avoiding prolonged sitting or standing.
- Maintaining a healthy weight.
- Elevating legs regularly.
- Wearing compression stockings.
- Sclerotherapy (vein injection) may be used for cosmetic reasons or symptom relief.
Baker's Cyst
A Baker's cyst is a fluid-filled sac behind the knee, often linked to arthritis or knee injuries. While many are asymptomatic, some can cause a feeling of fullness and mild pain or stiffness. If the cyst ruptures, fluid can leak into the calf, causing swelling, redness, tenderness, and bruising, mimicking a DVT.
Treatment: If asymptomatic, no treatment is usually needed. Symptomatic cysts can be managed with NSAIDs, steroid injections into the knee joint, cyst drainage followed by steroid injection, or rarely, surgical removal.
Sciatica
Sciatica refers to pain radiating along the path of the sciatic nerve, which runs from the lower back through the buttocks and down the leg. It's often caused by nerve compression from a herniated disc or bone spurs. Symptoms can range from a dull ache to shooting pain, often accompanied by numbness or weakness, potentially affecting the calf.
Treatment: Typically involves physical therapy, pain medication (NSAIDs or nerve pain drugs), and lifestyle adjustments. Steroid injections or surgery may be considered for severe or persistent pain.
Lower Leg Fracture
A fracture of the fibula (the smaller calf bone) can occur due to twisting injuries or direct blows. Pain intensity varies with severity. Even with minor fractures, walking may worsen the pain. Swelling, bruising, and skin breaks can occur. More severe trauma can result in fractures of both the tibia and fibula.
Treatment: Nondisplaced fibular fractures are usually treated with immobilisation (splint or cast), ice, elevation, and pain medication. Physical therapy aids recovery. Significant fractures or those involving multiple bones require specialist orthopedic care.

Claudication
Claudication is muscle pain, typically cramping, felt in the calves, thighs, or buttocks during activity due to reduced blood flow. It's usually caused by Peripheral Artery Disease (PAD), where arteries narrow due to plaque buildup. Calf pain is the most common symptom, worsening with exertion and relieved by rest.
Treatment: Involves lifestyle changes (smoking cessation, managing diabetes, high blood pressure, cholesterol), supervised walking programs, and medication (e.g., cilostazol). Procedures like angioplasty or bypass surgery may be necessary for severe cases.
Neurogenic Claudication
Also known as pseudoclaudication, this is linked to lumbar spinal stenosis (narrowing of the spinal canal in the lower back), leading to nerve compression. Symptoms include tingling, aching, or cramping pain in the buttocks, thighs, or calves, often worse with walking or standing and relieved by leaning forward or sitting. Numbness and weakness can also occur.
Treatment: Painkillers, physical therapy, epidural steroid injections, and sometimes complementary therapies. Surgery (laminectomy) may be performed to relieve nerve compression.
Bone Infection (Osteomyelitis)
An infection in the bone, usually bacterial, can spread from nearby tissues or the bloodstream. Significant leg injuries can also lead to bone infection. Symptoms include a dull, constant pain, swelling, and sometimes fever.
Treatment: Involves surgery to remove infected tissue and bone, followed by prolonged courses of antibiotics or antifungals.
Chronic Compartment Syndrome
Often associated with athletic activity, this condition involves increased pressure within muscle compartments, temporarily impeding blood flow to nerves and muscles. It causes cramping pain that intensifies during activity and resolves shortly after stopping. Numbness and muscle bulging can also occur.
Treatment: While not dangerous as symptoms resolve with rest, measures like physical therapy, modifying activity, or using orthotics can help prevent it. Surgery (fasciotomy) may be considered if conservative treatments fail.
Diabetic Peripheral Neuropathy
Nerve damage caused by diabetes, particularly affecting the small blood vessels supplying peripheral nerves. Symptoms, often worse at night, include burning pain, numbness (starting in the feet), and tingling, which can progress up the legs.
Treatment: Focuses on managing blood sugar levels, adopting healthy lifestyle habits, and taking nerve pain medications (e.g., duloxetine, pregabalin).
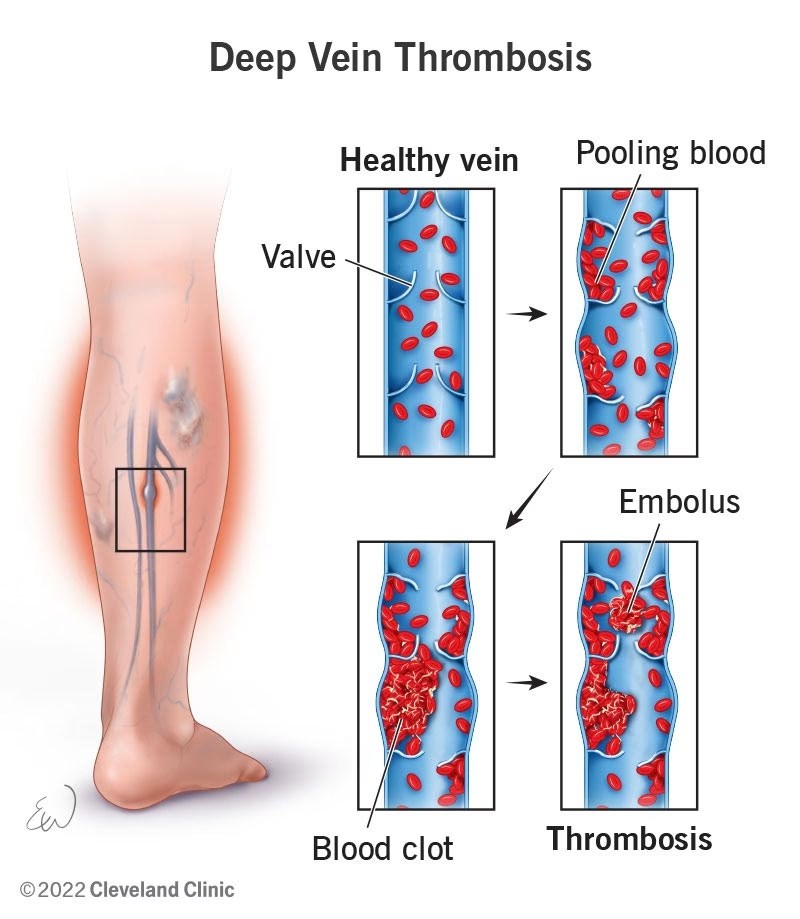
Deep Vein Thrombosis (DVT): A Serious Concern
Deep Vein Thrombosis (DVT) is a blood clot that forms in a deep vein, most commonly in the leg. While some DVTs are asymptomatic, others can cause swelling, pain, warmth, and redness or discolouration in the affected calf.

The critical danger of DVT is a Pulmonary Embolism (PE). A DVT clot can break free and travel to the lungs, blocking a main artery. A PE is a life-threatening emergency and requires immediate medical attention. Symptoms of PE include chest pain, rapid heartbeat, and difficulty breathing.
Risk Factors for DVT include: prolonged sitting (long flights, car journeys), obesity, sedentary lifestyle, smoking, birth control pill use, older age, recent surgery (joint replacement, abdominal), and a history of cancer.
Can calf pain from DVT come and go? Generally, a blood clot causing pain is a persistent issue; it doesn't typically "come and go" intermittently. If calf pain recurs or fluctuates, it's more likely due to other causes like muscle strain. However, if you experience calf pain, especially with risk factors for DVT, and particularly if accompanied by swelling, warmth, or redness, seek medical evaluation promptly.
Treatment for DVT: Standard treatment involves anticoagulant medication (blood thinners) to prevent clot formation and complications like PE. Other options may include clot-busting drugs (thrombolytics) or the placement of an inferior vena cava (IVC) filter.
Distinguishing DVT from Muscle Strain
It can be challenging to differentiate between a simple muscle strain and a DVT based on pain alone. However, key differences exist:
| Symptom | DVT | Muscle Strain |
|---|---|---|
| Pain Character | Often constant, deep ache or cramp; can be severe. | Tends to be activity-related, sharp or sore; may subside at rest. |
| Onset | Can be sudden or gradual. | Often related to specific activity or sudden movement. |
| Swelling | Common, often unilateral (one leg). | May occur but usually less pronounced than with DVT. |
| Redness/Warmth | Often present. | Rarely present. |
| Skin Discolouration | Possible (bluish or pale). | Unlikely. |
| Ability to Walk | May be difficult or impossible if severe. | Pain may worsen with walking, but usually possible. |
| Recurrence | The clot itself is a single event. Pain may persist. | Pain can be intermittent, improving with rest and returning with activity. |
Frequently Asked Questions (FAQs)
Q1: Can a blood clot cause intermittent calf pain?
Generally, calf pain caused by a DVT is more constant. If your calf pain comes and goes, it is more likely a muscular issue, but if you have any risk factors for DVT or other concerning symptoms, it's best to get it checked by a doctor.
Q2: What are the most common causes of calf pain?
The most frequent causes include muscle cramps, muscle strains, Achilles tendonitis, and issues related to varicose veins. However, more serious conditions like DVT, sciatica, and arterial claudication also present with calf pain.
Q3: How can I tell if my calf pain is serious?
Look for warning signs such as sudden severe pain, swelling, redness, warmth, skin discolouration, inability to walk, fever, or pain accompanied by weakness or numbness. If you experience these, seek immediate medical attention.
Q4: What should I do for a mild calf cramp?
For mild cramps, stretching the calf muscle by gently pulling your toes towards your shin can provide relief. Staying hydrated is also important. If cramps are frequent or severe, consult your doctor.
Q5: Is calf pain always a sign of DVT?
No, calf pain is very common and has many causes, most of which are not DVT. However, because DVT is a serious and potentially fatal condition, it's essential to be aware of its symptoms and seek medical evaluation if you suspect it.
In summary, calf pain can be attributed to a wide array of conditions. While many are benign and manageable with home care, it is imperative to recognise the symptoms that indicate a potentially serious or life-threatening issue, such as Deep Vein Thrombosis. Prompt medical evaluation is key when in doubt or when experiencing concerning symptoms.
If you want to read more articles similar to Calf Pain: Causes, Symptoms, and When to Seek Help, you can visit the Automotive category.
