27/09/2017
Understanding Sore Nipples During Breastfeeding
Experiencing sore, cracked, or painful nipples is a common, yet often distressing, challenge for many new mothers embarking on their breastfeeding journey. It's estimated that over 75 percent of mothers encounter some form of breastfeeding pain within the first two weeks postpartum. This discomfort can be a significant hurdle, and for some, it's the primary reason for discontinuing breastfeeding. However, with the right knowledge and support, most cases of sore nipples can be effectively managed and resolved, allowing for a more comfortable and rewarding breastfeeding experience.
The Most Common Culprit: Latch and Positioning
The vast majority of nipple pain stems from issues with how your baby attaches to the breast, commonly referred to as the 'latch'. A proper latch is crucial for effective milk transfer and, importantly, for preventing nipple trauma. When a baby doesn't take a deep enough mouthful of the breast, their tongue or the roof of their mouth can rub against the nipple, leading to irritation, soreness, and even cracking. This can happen if the baby is only sucking on the nipple itself, rather than encompassing a good portion of the areola.
Key signs of a poor latch include:
- Nipples that appear flattened, pinched, or drained of colour after feeding.
- Cracking, bruising, or bleeding of the nipples.
- A clicking sound during feeding, indicating the baby is losing suction.
- Pain that persists throughout the feed.
Achieving a Good Latch: A Step-by-Step Guide
Ensuring your baby is well-positioned and latches effectively is paramount. Here are some tips:
- Support is Key: Use pillows to bring your baby up to the level of your breast, rather than leaning down to your baby. This helps maintain good posture for both of you.
- Belly-to-Belly: Ensure your baby is facing you directly, chest to chest. They shouldn't have to turn their head to reach the breast.
- Nipple Aim: Aim your nipple towards your baby's nose. As they open wide, bring them to the breast, chin-first. Their chin should press into your breast, with their lips flanged outwards like a fish.
- Comfortable Hold: Experiment with different breastfeeding holds. Laid-back positions can often facilitate a deeper and more comfortable latch as they allow for better control.
- Check for Attachment: Your nipple should sit comfortably against the soft palate at the back of your baby's mouth. If it's closer to the front, it may be against the hard palate, causing pain.
Less Common Causes of Sore Nipples
While latch issues are the most frequent culprits, other factors can contribute to nipple soreness:
1. Engorgement
When your milk first comes in, your breasts can become full and tender. This engorgement can lead to sore nipples if the skin becomes stretched and sensitive. Feeding your baby on demand and offering a warm compress or shower before feeding can help ease discomfort. Cold packs after feeding can also provide relief.
2. Flat or Inverted Nipples
Nipple shape and size vary greatly. While flat or inverted nipples don't typically prevent breastfeeding, they might require extra support with latching initially. Techniques like stimulating the nipple before feeding or using an exaggerated latch position can be beneficial. If you have concerns, seeking advice from a lactation consultant is recommended.
3. Tongue-Tie
Tongue-tie, or ankyloglossia, occurs when the frenulum (the tissue connecting the underside of the baby's tongue to the floor of their mouth) is too short or tight, restricting tongue movement. This can significantly impact a baby's ability to latch properly, leading to sore nipples for the mother. Other signs of tongue-tie include a clicking sound during feeding, difficulty staying latched, and poor weight gain. If you suspect tongue-tie, consult your health visitor or a specialist for assessment and potential intervention, such as a simple frenotomy.
4. Thrush (Candida Infection)
A yeast infection, commonly known as thrush, can affect both the mother's nipples and the baby's mouth. If your nipples become cracked or damaged, they are more susceptible to infection. Symptoms in the mother can include severe, shooting pain in the nipples or breasts that lasts for hours after feeding, even if the latch appears good. In the baby, thrush may present as white patches in the mouth, red or cracked lips, or a persistent nappy rash. If thrush is suspected, both mother and baby will need to be treated with antifungal medication, usually prescribed by a GP.

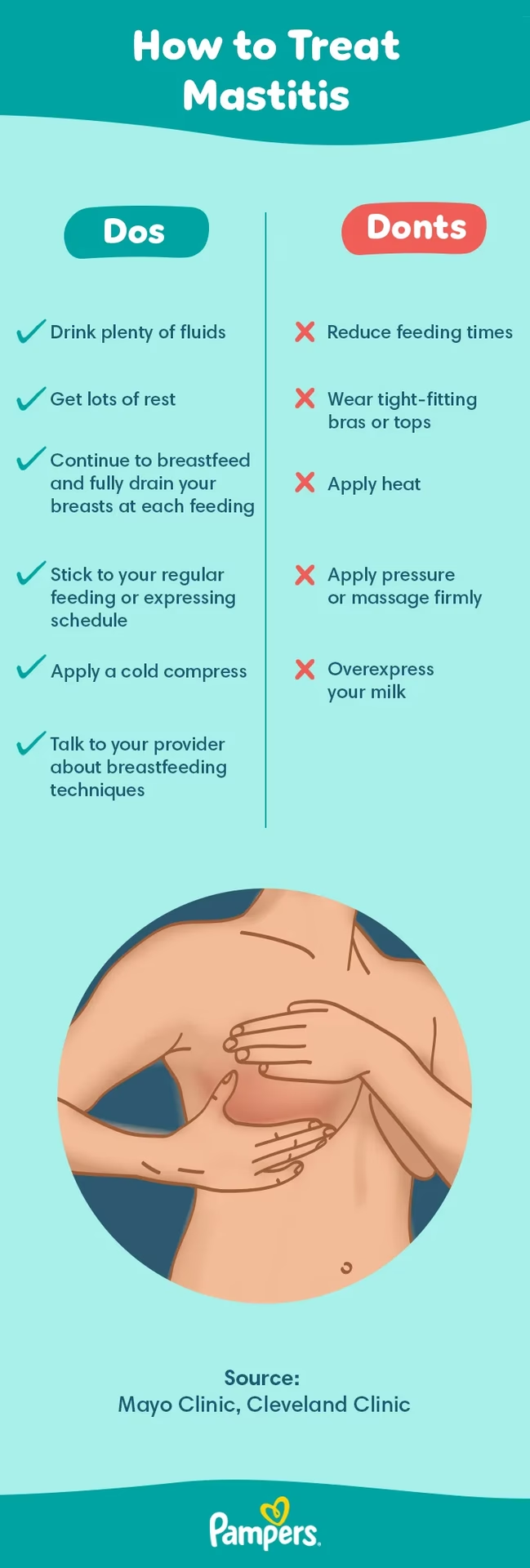
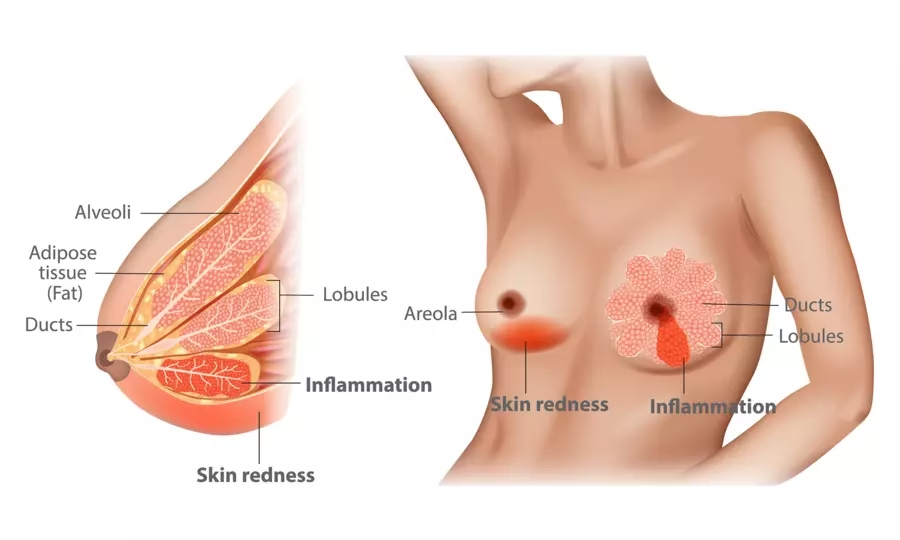
5. Mastitis
Mastitis is an inflammation of the breast, often caused by a blocked milk duct or infection. It can lead to redness, swelling, warmth, and pain in the breast. While mastitis itself doesn't directly cause sore nipples, the underlying issues that lead to mastitis (like poor milk removal) can also contribute to nipple pain. It's crucial to continue breastfeeding from the affected breast and seek medical advice if symptoms are severe or persist.
6. Nipple Vasospasm
Nipple vasospasm occurs when the blood vessels in the nipple constrict, reducing blood flow. This can cause a burning or deep pain, and the nipple may appear white or blanched after feeding. It can be triggered by a shallow latch or exposure to cold. Keeping the nipples warm and ensuring a good latch are key management strategies.

Seeking Support and Relief
It's important to remember that breastfeeding shouldn't be consistently painful. If you are experiencing persistent nipple pain, seeking professional support is highly recommended. Your midwife, health visitor, or a qualified lactation consultant can assess your baby's latch, offer guidance on positioning, and help identify any underlying issues. Local breastfeeding support groups, such as those run by the NCT, can also provide invaluable practical and emotional assistance.
Effective Treatments and Self-Care
While waiting for professional support, several measures can help alleviate nipple pain:
- Proper Latch: Revisit latch techniques and ensure your baby is taking a deep, comfortable hold.
- Nipple Care: After each feed, gently rinse your nipples with clean water and allow them to air dry. Applying expressed breast milk or a purified lanolin cream can help soothe and heal damaged skin.
- Pain Relief: Cool packs, hydrogel pads, or over-the-counter pain relievers (like paracetamol or ibuprofen, as advised by your healthcare provider) can be used between feeds.
- Nipple Shields: In some cases, nipple shields can provide a temporary barrier and allow damaged nipples to heal. However, they are best used under the guidance of a lactation specialist, as they can sometimes affect milk transfer or lead to dependency.
- Expressing Milk: If your nipples are very sore or cracked, you might consider expressing milk manually or using a breast pump until your nipples have healed.
What to Avoid
Certain practices are no longer recommended for managing nipple pain:
- Vigorous or deep massage of the breast.
- Using soaps or harsh cleansers on the nipples.
- Trying to 'pop' or open milk blisters yourself, as this can lead to infection.
- Excessive pumping or attempting to 'empty' the breasts, which can disrupt milk supply regulation.
When to Seek Professional Help
Don't hesitate to reach out for help if:
- Your nipple pain is severe or persistent.
- You notice signs of infection, such as redness, warmth, or fever.
- You suspect your baby has tongue-tie or thrush.
- Your baby is not gaining weight adequately.
Remember, seeking support early can make a significant difference in your breastfeeding journey. With the right approach, sore nipples can be a temporary challenge, allowing you to enjoy the many benefits of breastfeeding your baby.
Frequently Asked Questions
| Question | Answer |
|---|---|
| Can breastfeeding always be painful? | No, while some initial discomfort is common as you learn to breastfeed, persistent or severe pain is not normal and usually indicates an issue that needs addressing, most commonly a poor latch. |
| How can I tell if my baby has a good latch? | A good latch involves your baby taking a large mouthful of breast, with their chin pressed into the breast, lips flanged outwards, and no pain or pinching for the mother. Their cheeks should be rounded, not sucked in. |
| Should I stop breastfeeding if my nipples are sore? | It's generally recommended to continue breastfeeding if possible, as this helps with milk removal and healing. However, if the pain is unbearable, you may need to express milk temporarily until you can get support to correct the underlying issue. |
| Are nipple creams effective? | While many mothers find relief using nipple creams (like purified lanolin), the scientific evidence for their effectiveness in healing cracks is inconclusive. However, they can help to soothe the skin. Applying expressed breast milk is also a common and often effective practice. |
| What if I suspect thrush? | If you suspect thrush, it's essential to see your GP. Both you and your baby will likely need antifungal treatment to clear the infection effectively. |
This information is intended for general guidance only and does not constitute medical advice. Always consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.
If you want to read more articles similar to Sore Nipples: Causes and Relief, you can visit the Automotive category.

