15/05/2013
Leg pain can be debilitating, often leaving sufferers searching for answers and relief. While many types of leg discomfort exist, one of the most commonly misunderstood and misdiagnosed is sciatica. Far more than just a simple ache, sciatica is a specific type of nerve pain that originates in the lower back and radiates down the leg, capable of causing significant distress and impacting daily life. Understanding what sciatica is, its underlying causes, and how it differs from other forms of back pain is the crucial first step towards effective management and recovery.
- What Exactly Is Sciatica?
- Understanding the Symptoms of Sciatica
- What Causes Sciatica? The Root of the Problem
- Who Gets Sciatica and How Long Does It Last?
- Low Back Pain: A Broader Context
- Diagnosing Sciatica and Low Back Pain
- Managing Sciatica and Low Back Pain
- Frequently Asked Questions About Sciatica
- Complications and Prognosis of Sciatica
- Prevention of Low Back Pain and Sciatica
What Exactly Is Sciatica?
At its core, sciatica is a term used to describe nerve pain or sensory disturbances that occur within the distribution of the sciatic nerve or an associated lumbosacral nerve root. It's important to distinguish true sciatica from general low back pain or radicular leg pain, as in genuine sciatica, the pain directly results from pathology affecting the sciatic nerve or its roots.
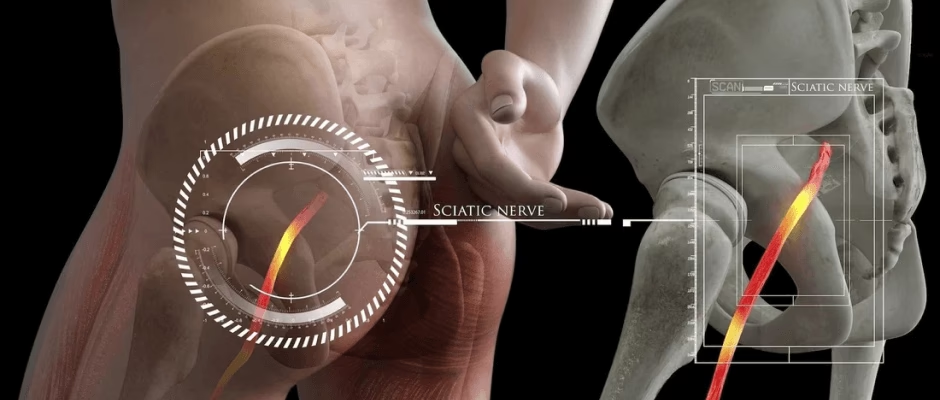
The sciatic nerve is the largest nerve in the human body, formed by a confluence of smaller nerve roots originating from the lower back, specifically from the L4 to S3 spinal levels. It extends from the buttock down into the leg, often reaching the foot and toes. When these nerve roots, or the main sciatic nerve itself, become irritated, compressed, or inflamed, the characteristic symptoms of sciatica manifest.
The Sciatic Nerve: A Closer Look
To fully grasp sciatica, it's helpful to visualise the sciatic nerve's pathway. Emerging from the lumbar and sacral regions of the spinal cord, these nerve roots merge to form the robust sciatic nerve. It then passes through the buttock and travels down the back of the thigh, branching out to supply sensation and muscle control to various parts of the leg and foot. Any interference along this extensive pathway can lead to the symptoms associated with sciatica.
Understanding the Symptoms of Sciatica
The symptoms of sciatica typically affect your bottom and the back of one leg, though they can extend all the way down to your foot and toes. While pain is the most prominent symptom, sciatica can present with a variety of other sensations due to the nerve irritation. Common symptoms include:
- A sharp, burning pain travelling down the back of the leg.
- Tingling sensations, often described as 'pins and needles'.
- Numbness in parts of the leg or foot.
- Muscle weakness in the affected leg.
- Electric shock-type sensations.
More unusual, yet possible, symptoms can include a sensation of coldness or even 'running water' down the leg. This occurs because irritated nerves can send an increased or aberrant number of signals. Conversely, if some signals in the nerve are blocked, you might experience numbness or muscle weakness. The pain is frequently exacerbated by specific movements such as lumbar spine flexion, twisting, bending, or even coughing and sneezing.

While back pain may also be present, it's often not as severe as the pain experienced in the leg. Symptoms can appear suddenly or develop gradually, and their intensity can vary significantly from mild to severe, often fluctuating day to day. This unpredictable nature can be very distressing, making it tough to focus on other things, but it's important to remember that sciatica is rarely dangerous.
What Causes Sciatica? The Root of the Problem
Sciatica arises from anything that irritates a nerve root that contributes to the sciatic nerve. The most common cause of this irritation is nerve root compression, often associated with changes in the spinal discs. However, it's crucial to understand that not all disc changes lead to pain.
Common Causes of Nerve Root Irritation:
- Disc-Related Changes: Discs are tough, circular structures that act as shock absorbers between the bones (vertebrae) of the lower back. They are strongly attached to the vertebrae, meaning they cannot truly 'slip'. However, they can bulge or herniate, leading to a condition often referred to as a 'slipped disc' (more accurately, a disc prolapse). When a disc prolapses, its soft inner material can press on an adjacent nerve root, causing irritation and inflammation. The good news is that nerve roots are remarkably resilient; they often have 'wiggle room', and many disc-related changes can shrink over time, allowing the nerve roots to recover.
- Inflammation: In some cases, nerve roots can become irritated by inflammation even without direct compression. This can be just as painful as mechanical compression.
- Spinal Stenosis: A narrowing of the spinal canal, which can put pressure on the spinal cord and nerve roots.
- Spondylolisthesis: A condition where one vertebra slips forward over another, potentially compressing nerve roots.
- Other Conditions: Less common causes include tumours, infections, or injuries to the spine.
General Contributing Factors:
Beyond direct nerve irritation, several general factors can influence pain perception and contribute to the development or persistence of sciatica:
- Reduced sleep quality
- High levels of stress
- Overall emotional wellbeing
- Highly demanding jobs, prolonged standing, and awkward lifting are consistent predisposing factors for low back pain, which can often lead to sciatica.
- Obesity increases the risk.
- Psychosocial work-related stress and a family history of back pain can also play a role.
Who Gets Sciatica and How Long Does It Last?
Sciatica can affect people of all ages, but it is most commonly observed in individuals in their forties and fifties. The pain is typically at its worst during the first few weeks, with significant improvement usually seen over the first few months. Approximately half of people with sciatica will have significantly improved by twelve weeks, and about three-quarters will have recovered within a year. However, for a subset of individuals, pain may not improve as expected, or recovery may take a considerably longer time. This variability often relates to how individuals adapt and cope with their symptoms.
Low Back Pain: A Broader Context
While sciatica is a specific type of leg pain, it often coexists with or is mistaken for general low back pain. Low back pain is an extremely common problem, demanding significant medical resources and serving as a major cause of physical, psychological, and social disability. Most cases of back pain are simple and self-limiting, but it is crucial to recognise when the pain signals something more serious.

Definitions of Back Pain Types:
Understanding the different classifications of back pain can aid in diagnosis and management:
| Type of Back Pain | Characteristics | Potential Causes |
|---|---|---|
| Mechanical Back Pain | Varies with posture, exacerbated by movement. | Spinal joints, vertebrae, soft tissues; may include intervertebral disc prolapse, vertebral fracture, facet joint injury. |
| Nonspecific Low Back Pain | Cannot be attributed to a specific identifiable cause. | Diagnosed when no specific pathology is found. |
| Inflammatory Low Back Pain | Pain and stiffness on waking, improved by movement. Insidious onset, chronic course. | Rheumatoid conditions (e.g., ankylosing spondylitis) affecting spinal joints. |
Low back pain can also be classified by duration: acute (present for less than six weeks) or chronic (present for more than six weeks).
Epidemiology of Low Back Pain in the UK
Low back pain is a global health challenge and the leading cause of disability worldwide, with a lifetime prevalence exceeding 80%. In the UK, approximately 20% of people with low back pain consult their GP each year. It accounts for a significant portion of sickness absence within the NHS and costs the UK economy billions annually. A cross-sectional study found the one-month prevalence of low back pain to be around 30% in adults aged 25+, peaking between 41-50 years, with chronic low back pain affecting about 1% annually.
Diagnosing Sciatica and Low Back Pain
Diagnosing sciatica is primarily a clinical process, based on a thorough history, the patient's reported symptoms, and a physical examination. In most cases, scans are not typically required for diagnosis as they often don't influence the initial treatment plan. However, there are specific circumstances where diagnostic imaging becomes appropriate.
When to Consider Diagnostic Imaging:
Imaging, such as X-rays, CT scans, or MRI, is generally indicated only if serious or specific pathology is suspected, often highlighted by 'red flags' (see below). For instance:
- Plain X-ray of the lumbar spine: Rarely affects management for simple back pain and involves significant radiation. It's useful if a fracture is suspected, or for detecting metastatic carcinoma, osteoporosis, myeloma, or Paget's disease of bone.
- CT scans: Often best for visualising stress fractures and spondylolisthesis.
- MRI scans: Provide excellent images of soft tissues, including discs, and anything impinging on nerves or the spinal cord. MRI is the most useful investigation for nerve root compression, discitis, and suspected neoplastic disease. It's also appropriate as part of surgical planning or when considering specialist nerve injections.
Blood and Urine Tests:
These may be ordered if cancer, infection, or inflammation is suspected. Tests might include FBC (Full Blood Count), ESR (Erythrocyte Sedimentation Rate), CRP (C-reactive Protein), and urine analysis. LFTs (Liver Function Tests), Alkaline Phosphatase, and PSA (Prostate-Specific Antigen) may also be relevant depending on the suspected underlying condition.

'Red Flags': When to Seek Urgent Medical Advice
Certain symptoms and signs, known as 'red flags', suggest potentially serious spinal pathology requiring urgent assessment. It's important not to base suspicion on a single red flag alone, but rather on combinations of features. These include:
| Red Flag | Potential Serious Condition | Key Symptoms/Signs |
|---|---|---|
| Cauda Equina Syndrome (CES) | Spinal cord compression emergency | Saddle anaesthesia/paraesthesia, recent onset of bladder/bowel dysfunction (incontinence, retention), perianal/perineal sensory loss, unexpected laxity of anal sphincter, severe or progressive neurological deficit in lower extremities. |
| Spinal Fracture | Vertebral injury | Sudden onset of severe central pain relieved by lying down, major trauma (road accident, fall from height), minor trauma/strenuous lifting in osteoporosis, structural deformity, point tenderness over vertebral body. |
| Cancer or Infection | Underlying systemic disease | Pain remaining when lying down, aching night-time pain disturbing sleep, thoracic pain (could also be aortic aneurysm), onset in <20 or >50 years, history of cancer, constitutional symptoms (fever, chills, unexplained weight loss), recent bacterial infection, IV drug misuse, immune suppression, structural deformity, point tenderness. |
If any of these red flags are present, urgent referral to a specialist (e.g., neurosurgeon, orthopaedic surgeon) is necessary. For CES, this means immediate referral.
Managing Sciatica and Low Back Pain
The primary principles of managing low back pain and sciatica involve keeping the patient active and providing appropriate pain relief to facilitate this activity. Gone are the days of prolonged bed rest; now, rest is only considered in exceptional cases and for no longer than 48 hours.
Conservative Treatments:
For most people, a range of conservative management options are highly effective:
- Time and Patience: Nerve roots are resilient, and many cases of sciatica improve significantly over weeks to months as the body heals and adapts.
- Pain Relief Medicines:
- Simple Painkillers: Paracetamol can ease pain and should be taken regularly as directed.
- Anti-inflammatories: Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can help reduce swelling and pain, allowing for freer movement. Always follow packet instructions and discuss safe use with a pharmacist, especially with underlying health conditions. Note that ibuprofen should generally be avoided for 48 hours after an initial injury as it may slow healing.
- Nerve Pain Control: If simple pain relief is insufficient, your GP may prescribe drugs specifically for nerve pain, such as Amitriptyline, in line with NICE guidance. Gabapentinoids, other antiepileptics, oral corticosteroids, or benzodiazepines are generally not recommended for sciatica due to lack of overall evidence of benefit and potential for harm.
- Weak Opioids: Only considered if NSAIDs are ineffective, contraindicated, or not tolerated. Paracetamol monotherapy is generally not recommended as it has been shown to be ineffective.
- Exercise and Activity: Gradual, progressive exercise is safe and highly beneficial. While initial rest might be sensible during a flare-up, maintaining activity helps reduce inflammation and maintain function. There's no single 'best' exercise; choose activities you enjoy and can tolerate, such as walking, swimming, or a specific rehabilitation programme.
- Lifestyle Advice: Addressing factors like smoking cessation and weight management can significantly aid recovery and reduce recurrence risk.
- Postural Adjustments: People with sciatica often find sitting, sleeping, or driving postures painful. While maintaining these postures isn't harmful, exploring different positions or moving more regularly can provide relief during intense pain. As pain becomes more tolerable, relaxing, moving, and exploring a variety of postures are part of rehabilitation.
Specialist Interventions:
In a smaller group of people, if conservative treatment is ineffective or there is severe nerve compression, specialist options may be discussed:
- Epidural Corticosteroid Injections: Can be used to reduce nerve pain in the short term.
- Lumbar Discectomy: Surgical intervention considered for severe nerve compression or persistent symptoms unresponsive to conservative treatment. Techniques include open discectomy, microdiscectomy, or minimally invasive endoscopic approaches.
Patients may reasonably believe that pain is a warning sign to avoid activity. However, with back pain, it's often necessary to work through the pain to overcome it. Psychosocial barriers, known as 'yellow flags', can prolong recovery and lead to chronicity. These include:
- Belief that pain and activity are harmful.
- Sickness behaviours (e.g., extended rest, social withdrawal).
- Emotional problems (low mood, depression, anxiety, stress).
- Work-related problems or dissatisfaction.
- Inappropriate expectations of treatment.
- Lack of support or overprotective family.
Targeting these yellow flags, especially when they are prominent, can lead to positive results and improve prognosis.
Referral Guidance:
Referral to specialists or multidisciplinary services is considered based on the severity and persistence of symptoms:
- Urgent Referral: Immediately for suspected Cauda Equina Syndrome. For progressive, persistent, or severe neurological deficit, urgent neurosurgical or orthopaedic assessment is required.
- Early Referral: If pain or disability remain problematic after a week or two, consider early referral for physiotherapy or other physical therapy.
- Specialist Assessment: If sciatica is still disabling and distressing after six weeks, referral for neurosurgical or orthopaedic assessment is warranted.
- Multidisciplinary Services: If pain or disability continues despite appropriate pharmacotherapy and physical therapy, referral to a multidisciplinary back pain service or chronic pain clinic may be beneficial. These often include cognitive behavioural programmes and back schools.
Frequently Asked Questions About Sciatica
Is the pain travelling down my leg definitely sciatica?
Not necessarily. Only about 8-10% of back-related problems are thought to be truly nerve-related. Pain from sensitive muscles and joints in the back and hip can also cause pain that radiates down the leg. A health professional can perform a physical examination to determine if your symptoms align with sciatica.

Is sciatica a neuropathic pain?
Yes, sciatica, also known as radicular pain or radiculopathy, is considered neuropathic leg pain. It is secondary to compressive lumbosacral nerve root pathology. When it coexists with non-specific back pain, the symptoms of sciatica tend to predominate.
Do I need a scan to diagnose sciatica?
Scans are not usually required to diagnose sciatica. It's a clinical diagnosis based on your history, symptoms, and a physical examination. In many cases, scans do not change treatment plans. They are appropriate for a small group of people as part of surgical planning, when considering a specialist nerve injection, or if a serious medical condition is suspected (e.g., 'red flags').
How painful is sciatica?
Sciatica symptoms can range from mild to severe and fluctuate daily. The pain can be intense, unpredictable, and very distressing, sometimes feeling all-consuming and making it difficult to focus. While scary, sciatica is rarely dangerous. It's important to be supported in managing pain while trying to maintain activities that bring value to your life, such as walks, hobbies, or socialising, as this aids coping and emotional wellbeing.
Can I sit and sleep comfortably with sciatica?
People with sciatica often find sitting, sleeping, or driving postures painful. While maintaining these postures is not harmful, during times of intense pain, it can be helpful to explore different postures or move more regularly. As pain becomes more tolerable, relaxing, moving, and exploring a variety of postures become part of a recovery or rehabilitation programme.

Should I exercise with sciatica?
When pain persists, nerves can become sensitive to movement. While initial rest or resting during a flare-up might be sensible, exercising in a gradual, progressive way is generally safe and helpful. For many, it helps reduce inflammation and maintain function. There isn't a 'best' exercise; choose activities you enjoy and can perform at a tolerable level several times a week, such as walking, swimming, or a specific rehabilitation programme.
Complications and Prognosis of Sciatica
Acute sciatica or low back pain can become chronic if not managed actively or if behaviours predispose to chronicity. Early recognition and management of 'yellow flags' and tailored management based on prognosis can help minimise this risk. Failure to diagnose and act on 'red flags', especially Cauda Equina Syndrome, can lead to long-term neurological damage. While most simple low back pain and sciatica cases lead to full recovery, the timeline can vary. For older individuals, back pain may simply be a feature of advancing years, and staying active remains key.
Prevention of Low Back Pain and Sciatica
Preventing back pain in the workplace depends on the nature of the job. While there's limited evidence for the effectiveness of lumbar supports or general education programmes, much work has focused on secondary prevention once an episode occurs. This involves addressing both physical and psychosocial issues, such as ensuring proper lifting techniques, ergonomic workstation setups (desks, chairs, computer screens), and comfortable seating in vehicles. Maintaining a positive attitude and enthusiasm for recovery, coupled with supportive work environments, also significantly contributes to reducing the risk of recurrence.
If you want to read more articles similar to Sciatica Unveiled: Understanding the Pain & Its Roots, you can visit the Automotive category.
