29/12/2020
Imagine this common scenario: you're at the doctor's surgery, perhaps with a troublesome sore throat. When asked about allergies, without a moment's hesitation, you state, “Penicillin.” It’s a declaration you’ve made for years, possibly since childhood, perhaps because a parent informed you of it. The medical professional nods, makes a note, and proceeds with the consultation. Yet, here's the surprising truth: there's a significant chance your long-held belief about a penicillin allergy is incorrect. Astonishingly, whilst 10% to 20% of Britons report having a penicillin allergy, fewer than 1% actually do.
As specialists in infectious disease and drug allergies, including the intricacies of penicillin allergies, we understand the profound implications of this widespread misunderstanding. An inaccurate penicillin allergy label can unfortunately prevent you from receiving the most appropriate and safest treatment for an infection. Furthermore, it significantly increases your risk of antimicrobial resistance, a critical global health concern where antibiotics cease to be effective against bacteria. The good news, however, is that identifying your true allergy status has become remarkably easier in recent years. Healthcare professionals are increasingly aware that many penicillin allergy labels are mistaken, and there are straightforward, safe methods to ascertain the facts.
- The Penicillin Paradox: Debunking Common Misconceptions
- Penicillin: A Steadfast Lifesaver and Its Advantages
- The Hidden Dangers of an Incorrect Allergy Label
- Unravelling Your True Penicillin Allergy Status
- Recognising a True Penicillin Allergy: Signs and Symptoms
- What About Other Beta-Lactam Antibiotics?
- Frequently Asked Questions (FAQs)
- Can a penicillin allergy disappear over time?
- What are the common signs of a penicillin allergy?
- If I had a rash as a child while taking penicillin, does that mean I'm allergic?
- Are penicillin allergies hereditary?
- Why is it important to confirm my penicillin allergy status?
- How can I find out if I am still allergic to penicillin?
The Penicillin Paradox: Debunking Common Misconceptions
The discrepancy between reported and actual penicillin allergies is a pervasive issue within healthcare. Many individuals carry this label throughout their lives based on events that were misinterpreted or have simply faded over time. Understanding why this mismatch occurs is the first step towards rectifying it.
The Misleading Childhood Rash
One of the most frequent reasons for an incorrect allergy label stems from childhood. It's common for children to develop skin rashes alongside various infections, many of which are viral and not related to medication. If a child happens to be taking an antibiotic at the time such a rash appears, it’s often mistakenly attributed to the drug, leading to a penicillin allergy diagnosis that persists into adulthood. The rash may have been caused by the illness itself, not the antibiotic.
Side Effects vs. True Allergies
Antibiotics, like many medications, can cause side effects such as nausea, diarrhoea, or headaches. These reactions are often unpleasant but do not indicate a true allergic response. A genuine allergy involves an abnormal immune system reaction, whereas side effects are typically predictable physiological responses to the drug. These common, non-allergic reactions usually resolve on their own or can be managed with advice from a doctor or pharmacist, who can offer strategies to mitigate them.
Is It Hereditary?
Another common misconception is the belief that penicillin allergies are hereditary. Many people assume that if a family member has an allergy, they must also be allergic. However, medical research clearly indicates that having a relative with a penicillin allergy does not mean you are allergic yourself. Penicillin allergies are not inherited, challenging a long-held myth for many families.
The Fading Allergy: How Long Does It Really Last?
Perhaps the most compelling reason for the high rate of mislabelled allergies is the fact that true penicillin allergies can diminish over time. Approximately 80% of individuals with a confirmed penicillin allergy will lose that allergy after about 10 years. This means that even if you experienced a genuine allergic reaction to penicillin in the past, your body's immune response may have changed, rendering you non-allergic today. The timing of your last reaction is therefore crucial in determining your current allergy status.
Penicillin: A Steadfast Lifesaver and Its Advantages
Discovered by Alexander Fleming in 1928 and widely adopted for treating infections in the 1940s, penicillin was the world's first antibiotic drug. Extracted from a type of mould called penicillium, it, along with closely related antibiotics like amoxicillin and amoxicillin/clavulanate (known by the brand name Augmentin), remains a cornerstone in modern medicine. These antibiotics are frequently prescribed for common infections such as ear infections, strep throat, urinary tract infections, pneumonia, and various dental infections.
Narrow-Spectrum vs. Broad-Spectrum Antibiotics
Penicillin antibiotics are classified as narrow-spectrum antibiotics. This means they are highly targeted, effectively combating specific types of bacteria. This specificity is a significant advantage, as it minimises the impact on beneficial bacteria residing in the body. In contrast, individuals mistakenly labelled as penicillin-allergic are often prescribed broad-spectrum antibiotics. These drugs kill a wide array of bacteria, including the helpful ones that contribute to a healthy microbiome. This indiscriminate action makes it easier for resistant bacteria to survive and proliferate, accelerating the development of antibiotic resistance – a severe threat to public health. Moreover, broad-spectrum antibiotics can be less effective for specific infections and are often considerably more expensive than their narrow-spectrum counterparts.
| Feature | Narrow-Spectrum Antibiotics (e.g., Penicillin) | Broad-Spectrum Antibiotics |
|---|---|---|
| Target Range | Targets specific types of bacteria | Targets a wide range of bacteria (including helpful ones) |
| Impact on Beneficial Bacteria | Minimal impact | Significant impact, killing off beneficial bacteria |
| Risk of Antimicrobial Resistance | Lower risk due to targeted action | Higher risk due to widespread bacterial elimination |
| Effectiveness | Often highly effective for specific infections | Can be less effective for specific infections, sometimes unnecessary |
| Cost | Generally more affordable | Often more expensive |
| Side Effects | Typically fewer side effects | Potentially more side effects due to broader impact |
Believing you have a penicillin allergy when you don't carries significant negative health consequences. It's not merely an inconvenience; it can directly impact the quality and efficacy of your medical care.
- Suboptimal Treatment: You are more likely to receive stronger, broad-spectrum antibiotics that may not be the best fit for your specific infection and can come with more pronounced side effects.
- Increased Antimicrobial Resistance: The overuse of broad-spectrum antibiotics contributes to the global crisis of antibiotic resistance, making future infections harder to treat.
- Higher Infection Risk: Individuals with an incorrect penicillin allergy label may face an increased risk of infection after surgery.
- Extended Hospital Stays: When hospitalised for an infection, you might spend longer in care due to less effective initial treatment options.
- Elevated Medical Costs: The use of more expensive, alternative drugs can lead to significantly higher medical bills.
Given that penicillin and its close relatives are often the optimal tools for treating a multitude of common infections, confirming you are not truly allergic can unlock access to safer, more effective, and more affordable treatment options, ultimately leading to better health outcomes.
Unravelling Your True Penicillin Allergy Status
If you suspect your penicillin allergy label might be incorrect, or if it's been many years since your last reaction, it’s highly recommended to investigate your true allergy status. The process is safe, straightforward, and increasingly accessible.
The Initial Consultation: Your Story Matters
The first step is always to consult a healthcare professional, such as your general practitioner or a pharmacist. They will engage in a detailed discussion about your allergy history. Expect questions such as: What exactly happened during the reaction? How soon after taking the antibiotic did the reaction occur? Was any medical treatment needed for the reaction? Have you taken any similar medications since then? This thorough interview can often distinguish between a true allergy and a non-allergic reaction. In many cases, this initial conversation is sufficient to confidently determine that you are not allergic to penicillin.
Penicillin Skin Testing: A Closer Look
If the initial interview doesn't provide a definitive answer, further testing may be recommended. One common method is penicillin skin testing. This involves tiny pricks on the skin and small injections just under the skin's surface, using components related to penicillin. These tests are designed to safely check for an immediate allergic reaction. If no reaction occurs during the skin testing, the next step typically involves taking a small, supervised dose of amoxicillin at your doctor's office to ensure complete safety and confirm you can tolerate the medication.

The Oral Challenge: A Direct Approach
Recent studies have shown that in many situations, particularly for low-risk individuals, skipping the skin test and proceeding directly to a small oral test dose (an 'oral challenge') can also be a safe and effective way to confirm allergy status. In this method, patients are given a low dose of amoxicillin and are carefully observed for approximately 30 minutes to monitor for any reaction. This streamlined approach highlights the growing confidence within the medical community regarding the safety of penicillin de-labelling.
Recognising a True Penicillin Allergy: Signs and Symptoms
A true penicillin allergy is an abnormal reaction of your immune system to the antibiotic drug. It's crucial to differentiate between mild reactions and severe, life-threatening responses.
| Severity | Common Signs & Symptoms | Recommended Action |
|---|---|---|
| Mild to Moderate |
| Consult a healthcare professional. These symptoms often resolve on their own, but medical advice is important for management and future drug choices. |
| Severe (Anaphylaxis) |
| This is a life-threatening medical emergency. Seek IMMEDIATE medical attention. Call emergency services (e.g., 999 in the UK) without delay. |
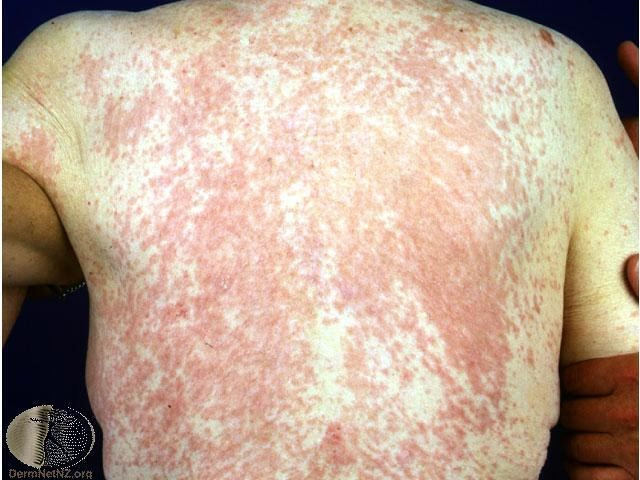
While common signs include hives, rash, and itching, the most severe reaction is anaphylaxis, a condition that affects multiple body systems and requires urgent medical intervention. Given that penicillin allergies are often over-reported, an accurate diagnosis is paramount to ensure you receive the best and most appropriate treatment options for any future infections.
What About Other Beta-Lactam Antibiotics?
Penicillin belongs to a class of antibiotics known as beta-lactams. Other antibiotics, particularly those with similar chemical structures, such as cephalosporins and carbapenems, can theoretically also cause allergic reactions due to cross-sensitivity. However, the risk of cross-sensitivity for individuals with a non-severe penicillin allergy is generally considered low.
For individuals with a non-severe penicillin allergy, the general medical advice is to avoid penicillin itself. However, cephalosporins, carbapenems, and other beta-lactam antibiotics can often be used with caution. Your healthcare professional will assess your specific allergy history and determine the safest course of action, weighing the benefits against the low risk of cross-reactivity. This nuanced approach allows for a broader range of effective antibiotic options even if a mild penicillin allergy is genuinely present.
Frequently Asked Questions (FAQs)
Can a penicillin allergy disappear over time?
Yes, absolutely. Research indicates that approximately 80% of individuals with a true penicillin allergy will lose that allergy after about 10 years. This is a crucial factor, meaning many people who were once genuinely allergic may no longer be.
What are the common signs of a penicillin allergy?
Common signs include skin reactions like hives, rashes, and itching. More severe reactions, though rare, can involve facial swelling, difficulty breathing, and anaphylaxis.
If I had a rash as a child while taking penicillin, does that mean I'm allergic?
Not necessarily. Rashes are very common in childhood infections, often caused by viruses themselves rather than the antibiotic. If you were taking penicillin at the time, the drug might have been incorrectly blamed. It's worth discussing this with a healthcare professional.
Are penicillin allergies hereditary?
No, penicillin allergies are not hereditary. Having a family member with a penicillin allergy does not mean you are predisposed to it yourself.
Why is it important to confirm my penicillin allergy status?
An incorrect allergy label can lead to receiving less effective, more expensive, and broader-spectrum antibiotics, increasing the risk of side effects and contributing to antibiotic resistance. Confirming your status opens up safer and more appropriate treatment options.
How can I find out if I am still allergic to penicillin?
You should speak to a doctor or pharmacist. They will ask detailed questions about your past reaction. If necessary, they may recommend penicillin skin testing or a supervised oral challenge with a small dose of amoxicillin to determine your current status.
In conclusion, the widespread belief in penicillin allergies often outstrips the reality. Many individuals are unnecessarily limited in their treatment options due to an outdated or misdiagnosed allergy label. By understanding how penicillin allergies can fade over time and by engaging with healthcare professionals for accurate testing, countless people can safely reclaim penicillin as a vital and effective option for treating common infections, paving the way for better health outcomes and a stronger fight against antimicrobial resistance.
If you want to read more articles similar to Penicillin Allergy: Is Your Diagnosis Still Valid?, you can visit the Automotive category.
